- LOGIN
- MemberShip
- 2026-04-24 02:52:27
- Company
- Mounjaro reimb for diabetes remains uncertain in KOR
- by Eo, Yun-Ho Apr 08, 2026 07:46am
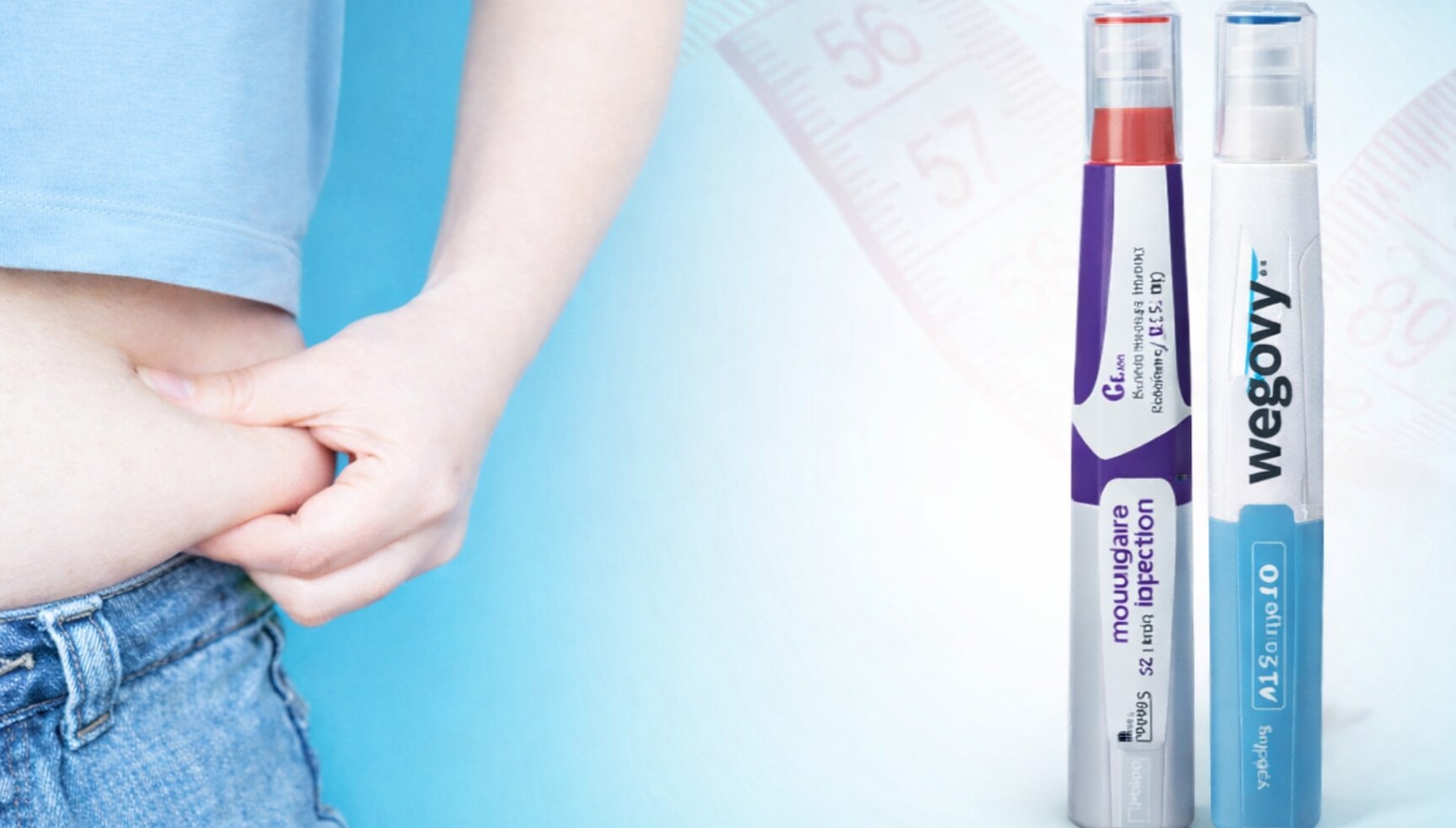
- Mounjaro, the star of the obesity treatment boom, has encountered a roadblock in its expansion of reimbursement for diabetes in Korea.According to industry sources, Eli Lilly Korea and the National Health Insurance Service (NHIS) failed to conclude pricing negotiations for Mounjaro (tirzepatide), a dual GIP/GLP-1 receptor agonist, within the deadline. A decision has now been made to extend the negotiation period.Whether Lilly and the NHIS will be able to reach an agreement and secure reimbursement listing for Mounjaro remains to be seen. Its competitor, Novo Nordisk’s Ozempic (semaglutide), which contains the same active ingredient as Wegovy, has been listed for reimbursement for diabetes since February.Mounjaro had previously passed the Drug Reimbursement Evaluation Committee (DREC) review under the Health Insurance Review and Assessment Service (HIRA) in December last year.Although it has generated exceptional sales as an obesity treatment, Mounjaro is also indicated in diabetes as an “adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes (monotherapy or combination therapy) and for chronic weight management in adults with obesity (initial BMI ≥30 kg/m²) or overweight patients with at least one weight-related comorbidity (hypertension, dyslipidemia, type 2 diabetes, obstructive sleep apnea, or cardiovascular disease), in conjunction with a reduced-calorie diet and increased physical activity.”For both indications, the recommended starting dose is 2.5 mg once weekly (intended for treatment initiation, not for glycemic control or weight management). After four weeks, the dose is increased to 5 mg once weekly. If further dose adjustment is necessary, the dose may be increased by 2.5 mg increments after at least 4 weeks at the current dose, up to a maximum of 15 mg once weekly.Meanwhile, Mounjaro is drawing attention as the first treatment to suggest the possibility of “remission” in diabetes.In the Phase III SURPASS study, which became the basis for its approval, Mounjaro demonstrated its potential for diabetes remission by achieving statistically superior improvements in HbA1c and body weight compared to all control groups, including semaglutide (1 mg, brand name Ozempic), insulin degludec, and insulin glargine.Furthermore, at the European Association for the Study of Diabetes (EASD) meeting held last September, the company presented results from the Phase III SURPASS-CVOT clinical trial, which directly compared Mounjaro with Lilly’s GLP-1 receptor agonist Trulicity, thereby reinforcing data on cardiovascular prevention effects and improvements in overall survival.
- Product
- Obesity drugs 'all-season market'…preference for high dose
- by Kim JiEun Apr 07, 2026 07:22am
- Injectable obesity treatments such as Wegovy and Mounjaro are shifting the market landscape. Moving away from the previous pattern in which demand spiked during specific seasons, a stable year-round demand is emerging, while short-term supply instability is emerging, particularly for high-dose products.According to local pharmacies and the wholesale industry, the obesity treatment market previously was defined as a 'seasonal market,' with prescriptions concentrated during the New Year for weight-loss resolutions or in the period leading up to summer. However, since the launch of Wegovy and Mounjaro, this pattern has been changing rapidly.An official from the wholesale industry explained, "In the past, demand was concentrated in specific seasons, but recently, a steady sales trend has continued regardless of the season," and that "A key characteristic of these items is that sales volatility has not been significant since their launch."Increasing demand for high-dose products is being observed even on pharmacy-exclusive online malls. Preference for the 5mg dose of Mounjaro and the 2.4mg dose of Wegovy is prominent, and at times, supply instability, such as temporary stockouts, has occurred.An official from a pharmacy-exclusive online mall stated, "While the overall sales trend for Wegovy remains stable, demand for high-dose products is particularly high," adding, "There have been instances where temporary supply-demand imbalances appeared."However, critics point out that the distribution structure remains heavily skewed toward hospitals and clinics. Aside from some large-scale pharmacies, many neighborhood pharmacies are giving up on carrying the products altogether.Furthermore, analysis suggests that the trend of patients flocking to clinics is intensifying as rumors regarding 'reimbursement status' for Mounjaro have recently spread.According to industry sources, these rumors appear to have originated from Mounjaro's diabetes indication obtaining 'reimbursement adequacy'. As news spread that it passed the initial hurdle for listing on the reimbursement schedule by passing the Pharmaceutical Reimbursement Evaluation Committee, cases of people misinterpreting this as actual reimbursement have increased.However, the drug is currently at a stage where follow-up procedures, such as price negotiations and deliberations by the Health Insurance Policy Deliberation Committee, remain. Thus, it has not been reimbursed.A pharmacist in Gangnam, Seoul, said, "For pharmacies that haven't previously carried the drug, securing the product itself is not easy," and that "Since nearby clinics are actively prescribing and selling, there isn't much incentive for pharmacies to handle it."The pharmacist added, "As rumors of Mounjaro's reimbursement circulate, demand for direct purchase at hospitals seems to have increased," and that "This trend is concentrating patients at clinics."
- Company
- Drug pricing re-evaluation lawsuit reverses the situation
- by Kim, Jin-Gu Apr 07, 2026 07:22am
- The lawsuit Medica Korea filed to cancel the price reductions on its existing drugs, challenging the government's re-evaluation of maximum prices, has concluded in the pharmaceutical company's favor. This ruling is expected to have a significant impact beyond the relief to an individual company, influencing the implementation of future government drug price reduction measures.In particular, the significance of this ruling has grown as the government announced a reform plan last month that strengthens the drug price reduction rate from the current 15% to 20% when generic standard requirements are not met. Analysis suggests that pharmaceutical companies facing price cuts due to administrative delays now have a clear justification for pursuing legal action.3-Year Legal Battle Concludes... A Litigation Started by 'Re-evaluation of Listed Drugs'The origin of this case was the "Generic drug price system reform" implemented in July 2020. The government decided to apply differential drug prices based on whether two standard requirements were met: ▲ conducting independent bioequivalence tests and ▲ using registered drug master files (DMF). Additionally, the government conducted a re-evaluation by applying these standards to drugs already listed on the reimbursement list.In September 2023, following the re-evaluation, the Ministry of Health and Welfare (MOHW) announced a price reduction for five items, including Medica Korea's 'Telmisartan Tab,' citing noncompliance with standard requirements.Medica Korea responded immediately by filing a lawsuit to cancel the disposition and an application for a stay of execution. Both the first and second-instance courts ruled in favor of the pharmaceutical company. Subsequently, on the 2nd, the Supreme Court finalized the original verdict by dismissing the government's appeal through a "discontinuation of proceedings." The three-year legal dispute ended in a complete victory for the pharmaceutical company. This is considered unusual, given that cases in which pharmaceutical companies win drug price lawsuits against the government have been very rare.“Violation of Administrative Procedures + Abuse of Discretion”... The Court Highlights Three Illegalities in the Government's MeasureAccording to the Article 8(2) issued by the Seoul High Court's ruling, confirmed by the Supreme Court, the court found that the MOHW's disposition not only violated administrative procedural principles but also constituted a deviation and abuse of discretionary power.◆“Administration Cannot Change Its Word” = The court pointed out the "unauthorized change of grounds for disposition" applied by the government to some items. The MOHW initially issued a price reduction for Medica Korea's five items because they failed to meet 'Standard Requirement 1' (independent bioequivalence testing). However, during the lawsuit, they argued that the items also failed to meet 'Standard Requirement 2' (the use of a registered DMF).Regarding this, the court stated that it is unacceptable to present separate facts that lack identity with the original grounds at the time of disposition. This is interpreted as a reaffirmation of the principle that the executive branch must not infringe upon a party's right to defense by arbitrarily changing the basis for a disposition.◆“Substantial Fulfillment is More Important Than Paperwork” = The court ruled that 'substantial fulfillment of requirements' should take precedence over the 'formal completeness of documents.' Medica Korea was unable to submit the final "DMF Change Authorization Certificate" within the government-set deadline. However, they had already submitted an 'Application for change authorization' before this, clearly indicating their intent to use registered drug master files. Despite this, the government issued the price reduction citing 'failure to submit documents within the deadline.'The court judged that “submitting the authorization certificate is merely one means of proving fulfillment, not the sole evidentiary material,” and that “if a pharmaceutical company has made its best efforts, it should be recognized.”◆A Warning Against ‘Administrative Convenience’ = The court clarified that the situation where the Ministry of Food and Drug Safety's (MFDS) review was delayed due to an explosion of change authorization applications following the drug price reform 'cannot be viewed as the responsibility of the plaintiff (pharmaceutical company).'The court ruled that it is unreasonable to hold a company responsible for document-submission delays caused by external factors beyond its control, to reduce drug prices. This is interpreted as a court warning against the government's drug price reductions driven by administrative convenience.Will 'Second Medica' Cases Follow Amid Concerns of Recurring ‘Administrative Bottlenecks’?This ruling is expected to have a greater ripple effect, as it coincides with the government's last month's drug-pricing reform plan. Under the reform, the basic calculation rate for generic drug prices will be reduced from 53.55% to 45%. Concurrently, the reduction rate for failing to meet standard requirements will be raised from 15% to 20%.Under the existing system, if one standard requirement was not met, the generic drug price was applied at 45.52% (53.55 x 0.85); if two were not met, at 38.69% (45.52 x 0.85). Under the new system, it will drop significantly to 36.00% (45.00 x 0.8) for one failure and 28.8% (36.00 x 0.8) for two failures.Upcoming drug-pricing reform plan. Under the reform, the basic calculation rate for generic drug prices will be reduced from 53.55% to 45%. Concurrently, the reduction rate for failing to meet standard requirements will be raised from 15% to 20%.These standards also apply to already-listed generics. Industry concerns are that the chaos of 2023 will repeat itself. In September 2023, the government simultaneously lowered the prices of 7,355 items. This was a measure that applied the drug price system, reformed in 2020, to existing items en masse. However, during the large-scale price reduction process, delays in data submission and review bottlenecks occurred, leading to continuous confusion and administrative conflicts regarding the interpretation of standards.The Medica Korea lawsuit is also analyzed to have occurred against this backdrop. Analysts believe that, in the process of evaluating and disposing of numerous items in a short period, the government failed to adequately review individual cases, leading to 'formalistic judgments' taking precedence.There is a possibility that even more listed items will be subject to price reductions in this reform. In this case, the administrative burden on the government will inevitably increase. It is noted that this process could create a vicious cycle of administrative errors, leading to more lawsuits.Reduction Rate Increased from 15% to 20%... Potential for Mass Recurrence of ‘Defensive Bioequivalence’ TestsThe measures taken by the pharmaceutical industry for 'price defense' are also factors fueling market confusion. Specifically, there is a high possibility that so-called 'defensive bioequivalence' tests to meet standard requirements will flood the market again.After the 2020 system reform, pharmaceutical companies rushed to conduct bioequivalence tests to defend prices. Companies developed generics themselves through internal formulation research and then conducted bioequivalence tests. Based on the equivalence results, they adopted a strategy of shifting from outsourced to in-house manufacturing to meet the 'conducting bioequivalence tests' requirement and maintain drug prices. In fact, the annual number of bioequivalence test approvals, which was 178 in 2018, surged to 323 in 2020 and 505 in 2021.The number of bioequivalence test approvals by month (unit: case, source: MFDS)The cost per bioequivalence test is estimated at KRW 300-500 million. Criticisms have been raised that spending hundreds of millions of won on bioequivalence tests to maintain drug prices, when the drugs are already being sold without issue after the government has recognized their safety and efficacy, is a waste of resources. Nevertheless, because the scale of price reductions has increased, the structure forces companies to increase additional bioequivalence tests to prevent losses."Litigation is Profitable"... The 'Learning Effect' Presented by the Medica Korea PrecedentConcerns are rising in the pharmaceutical industry that the litigation wars that followed the simultaneous reduction of 7,300 items in September 2023 will be repeated.With the Supreme Court's ruling now established, pharmaceutical companies' response is expected to become more aggressive. From a company's perspective, rather than accepting a 20% reduction, it is a rational choice to file a lawsuit to cancel the price reduction and seek a stay of execution under the Medica Korea precedent. Voices are high that unnecessary litigation will proliferate socially.Consequently, the government has a significant administrative burden during the large-scale drug price adjustment process. Following this Supreme Court ruling, the government's mechanical administrative convenience will find it difficult to gain legal legitimacy. Moving forward, the government faces the task of establishing flexible administrative guidelines that take into account realistic factors, such as the MFDS's review status, rather than insisting solely on the 'formal completeness of documents' during the price adjustment process for listed generics.A pharmaceutical industry official stated, "This ruling clearly established that substantial efforts by companies should not be ignored for administrative convenience. This case is expected to serve as an important legal reference for pharmaceutical companies to respond to the government's administration in the upcoming large-scale drug price reductions."
- Policy
- Government to prevent drug supply disruptions amid Middle East tensions
- by Jung, Heung-Jun Apr 07, 2026 07:22am
- Concerned that geopolitical risks in the Middle East could escalate into instability in the drug supply chain, the government is simultaneously pursuing regulatory improvements and conducting a survey of the current supply situation.This is because logistical disruptions involving raw materials and packaging materials could affect the domestic drug supply. In particular, there are concerns that shortages of petrochemical raw materials, such as naphtha, could exacerbate packaging supply issues.On the 3rd, the Pharmaceutical Supply Management Division of the Health Insurance Review and Assessment Service (HIRA) launched a survey on pharmaceutical supply status through the Korea Pharmaceutical and Bio-Pharma Manufacturers Association.The aim is to identify which drugs are being affected by import delays and supply disruptions due to risks in the Middle East. HIRA plans to use this information to proactively prepare countermeasures.HIRA is monitoring drug distribution inventory levels through the Korea Pharmaceutical Information Center. However, there is a limitation in that, while it has data on domestically distributed drugs, it is difficult to predict supply disruptions caused by import and logistics delays.HIRA is expected to compile information from pharmaceutical companies, including product names, packaging materials, and inventory levels, by next week and use this as a basis for formulating strategies such as future drug price management and securing alternative medications.If disruptions in the logistics networks for raw materials and packaging materials persist, the impact on domestic pharmaceutical companies’ production costs and supply stability could increase even further. Consequently, the government appears to be taking preemptive action before supply instability becomes a reality.The Ministry of Food and Drug Safety also discussed countermeasures last week with three companies supplying basic IV fluids and introduced unprecedented regulatory easing measures, including a fast-track system for approval changes.The measures were announced on the 3rd during a joint meeting of the Emergency Economic Measures Headquarters Meeting and Ministerial Meeting on Economic Affairs. The government announced regulatory easing measures. The MFDS lowered regulatory barriers to enable pharmaceutical and medical device manufacturers to diversify their supply chains for raw materials and packaging materials, such as IV solutions and syringe needles.First, in cases where changes to product approval are required due to shortages of petrochemical raw materials such as naphtha, a 'fast-track system' has been newly established to prioritize review over other items.Additionally, for medical devices, the agency allowed manufacturers to make changes to packaging materials to undergo document reviews instead of on-site GMP inspections.This is intended to reduce the one to two months it typically takes for pharmaceutical companies to complete product license amendment reviews. The measures to shorten review periods will be implemented immediately as part of the government’s proactive administration initiative.
- Policy
- Silymarin to undergo reimbursement reevaluations this year
- by Jung, Heung-Jun Apr 07, 2026 07:22am
- The ingredient 'silymarin (milk thistle extract),' which was the subject of a lawsuit after the company contested the results of the 2021 reimbursement reevaluation, is finally being put to the test once again. It is scheduled to be included in this year’s list of items subject to re-evaluation, alongside ginkgo biloba and dobesilate, which were previously on the list.According to industry sources on the 6th, the Health Insurance Review and Assessment Service (HIRA) Drug Reimbursement Evaluation Committee recently discussed a proposal to add silymarin to the list of items subject to reevaluation.In the 2021 reimbursement reevaluation, which also included dried bilberry extract and Avocado-soya unsaponifiables, silymarin was deemed inappropriate for reimbursement. In November of that year, the Ministry of Health and Welfare announced its decision to delist.Pharmaceutical companies filed injunction requests and administrative lawsuits. While the first trial in November 2023 upheld the reimbursement withdrawal, the appellate court overturned the decision in December last year, ruling in favor of the companies. The ruling became final after the Ministry of Health and Welfare chose not to appeal.Based on a review of the appellate court’s ruling, it appears that the direction has been set to conduct a re-evaluation of reimbursement appropriateness rather than delisting.This is interpreted as the court having pointed out procedural flaws in the reevaluation process rather than having judged the clinical utility of the drugs.Seven ingredients, including ginkgo biloba extract and calcium dobesilate, had already been discussed for reevaluation this year. It is reported that there have been changes to some of the other items. Although the agenda for items subject to reimbursement reevaluation was submitted to the Drug Reimbursement Evaluation Committee last January, the Health Insurance Policy Deliberation Committee has not yet reached a decision.Generally, items for reimbursement reevaluation are decided by the Health Insurance Policy Deliberation Committee immediately after being submitted to the Drug Reimbursement Evaluation Committee, but the process has been delayed due to the drug pricing reform, which includes changes to the reimbursement reevaluation criteria.Since the drug pricing reform plan was finalized at the March Health Insurance Policy Deliberation Committee meeting, the items are expected to be submitted to the committee this month.Furthermore, the items to be reevaluated next year remain unclear. Because the drug pricing reform has changed the annual reimbursement reevaluation to be conducted on an as-needed basis, the decision on items for 2027 will require further observation.
- Company
- Vadanem launches in Korea…draws attention as oral option
- by Son, Hyung Min Apr 07, 2026 07:22am
- The treatment paradigm for renal anemia may shift from a traditional ESA-centered approach to a multi-layered structure that includes oral treatment options. Amid this trend, Tanabe Pharma Korea and HK inno.N announced the domestic launch of the renal anemia treatment ‘Vadanem (vadadustat),’ signaling potential changes in treatment strategy.The two companies recently held a launch symposium titled ‘New Paradigm VADANEM Symposium’ at the Lotte Hotel Busan. The event featured a wide range of discussions on the mechanism of action and clinical data of HIF-PHI class therapies, as well as strategies for their application in real-world clinical practice.A view of the ‘Vadanem’ launch symposium.Renal anemia is a common complication in patients with chronic kidney disease (CKD), primarily caused by reduced erythropoietin (EPO) production due to impaired kidney function. Consequently, current treatment primarily relies on recombinant erythropoiesis-stimulating agents (ESAs) administered via injection.However, since ESAs are administered subcutaneously or intravenously, limitations have been pointed out, including treatment inconvenience, adverse reactions such as increased blood pressure and vomiting, as well as storage constraints. Although long-acting formulations with improved half-lives have emerged, the inconvenience of injection-based administration remains unresolved.Against this backdrop, oral HIF-prolyl hydroxylase inhibitors (HIF-PHIs) are emerging as a new alternative. This class of drugs works by inhibiting the enzymes that degrade hypoxia-inducible factors (HIF), thereby stimulating endogenous EPO production while simultaneously regulating iron absorption and utilization. They also offer advantages in administration convenience and storage compared to injectables.Vadanem is an oral HIF-PHI that regulates the HIF pathway. It induces endogenous erythropoietin production and improves iron utilization efficiency through a mechanism distinct from that of conventional ESAs.The symposium reflected this shift, highlighting the potential transition from ESA-centered treatment to a multi-layered approach that includes oral therapies.The first day’s session focused intensively on the mechanisms of HIF-PHI-class therapies and the clinical evidence for Vadanem. Chaired by Professor Jong-soo Lee of Ulsan University College of Medicine, presentations were delivered by Professor Bong Soo Park of Inje University College of Medicine and Professor Eun-sil Koh of The Catholic University of Korea College of Medicine.Professor Bong Soo Park of Inje University College of Medicine explained, “While ESAs supplement exogenous EPO, HIF-PHIs activate the hypoxia response pathway to induce endogenous EPO production. This represents a more physiological treatment strategy, as it also regulates iron metabolism.”Professor Eun-sil Koh of the Catholic University of Korea College of Medicine introduced the clinical results of Vadanem, stating, “In the INNO2VATE 1 and 2 clinical trials involving dialysis patients, Vadanem demonstrated non-inferiority in terms of hemoglobin (Hb) improvement compared to the injectable drug darbepoetin alfa (brand name Nesp).”In fact, during the primary efficacy evaluation period (weeks 24–36), the change in hemoglobin (Hb) was 10.36 g/dL for Vadanem and 10.61 g/dL for darbepoetin alfa, and in INNO2VATE 2, these values were 10.36 g/dL and 10.53 g/dL, respectively. Vadanem met the predefined non-inferiority criteria in both studies. Hb levels remained stable and showed similar trends during the long-term evaluation from weeks 40 to 52.It also demonstrated non-inferiority compared to darbepoetin alfa in terms of the risk of major adverse cardiovascular events (MACE). In the overall population, the hazard ratio (HR) for MACE was 0.96, meeting the predefined non-inferiority criteria (FDA 1.25, EMA 1.3).Professor Koh explained, “Consistent results were observed for individual cardiovascular events such as death, myocardial infarction, and stroke. We have established clinical evidence regarding both efficacy and safety.”VADANEM launch symposiumDuring the second day’s session, titled ‘VADANEM in Practice and Beyond,’ discussions focused on how to apply the mechanisms and clinical evidence presented the previous day to actual clinical practice.In particular, given the confirmed clinical efficacy and safety data for Vadanem, attention centered on which patient groups should be prioritized for treatment.Professor Sungjin Chung of the Catholic University of Korea College of Medicine stated, “In patients with CKD-related anemia, various factors such as ESA hyporesponsiveness, iron deficiency, and inflammation interact in a complex manner. For this patient population, HIF-PHI agents could serve as a new treatment alternative.”He added, “In patients with reduced ESA responsiveness, Hb control is often difficult with existing treatments. HIF-based approaches provide a clinically meaningful option.”He further noted, “Depending on the patient’s condition, we can adopt a more flexible treatment strategy, such as switching from ESA or considering oral therapy from the outset. Given the nature of the disease, which requires long-term treatment, oral formulations are also significant in terms of adherence. Their scope of application is expected to gradually expand in practice.”With the launch of Vadanem, attention is focused on whether HIF-PHI therapies will establish themselves as a mainstream option in Korea. The convenience of oral administration and regulation of iron metabolism are considered key factors in future changes to CKD anemia treatment strategies.Professor Sehoon Park of Seoul National University College of Medicine predicted, “We are entering an era that requires patient-tailored approaches based on multiple options rather than a single treatment strategy. The role of HIF-PHI class therapies will expand within this trend.”
- Company
- ‘Padcev + Keytruda’ reimbursement imminent in KOR
- by Son, Hyung Min Apr 07, 2026 07:22am
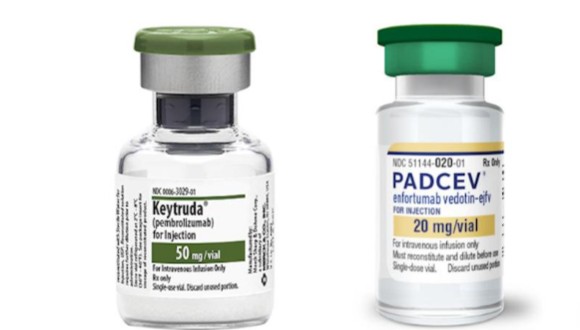
- Immunotherapy ‘Keytruda’ and ADC ‘PadcevWith combination therapy using antibody-drug conjugates (ADCs) and immuno-oncology drugs on the verge of being reimbursed in Korea, the treatment landscape for bladder cancer (urothelial carcinoma) is increasingly likely to undergo a structural shift.According to industry sources, the Health Insurance Review and Assessment Service (HIRA)’s Drug Reimbursement Evaluation Committee recognized the appropriateness of reimbursement for the combination therapy of Padcev and Keytruda as a first-line treatment for adults with locally advanced or metastatic urothelial carcinoma on April 2. Padcev monotherapy, however, did not receive reimbursement approval.This decision comes approximately 6 months after the combination regimen passed the Cancer Drug Deliberation Committee last October. If price negotiations with the National Health Insurance Service (NHIS) are concluded successfully, Padcev + Keytruda will be listed for reimbursement.Padcev is an ADC that targets Nectin-4, comprised of a fully human anti-Nectin-4 immunoglobulin G1 kappa monoclonal antibody conjugated to the small molecule microtubule-disrupting agent monomethyl auristatin E (MMAE), via a protease-cleavable maleimidocaproyl valine-cituline (vc) linker. Its mechanism of action involves selectively binding to tumor cells, internalization, and the release of MMAE via proteolytic cleavage, which subsequently induces cell death.Its key feature is the expected synergistic effect when used in combination with PD-1 inhibitors. This mechanism maximizes antitumor efficacy by simultaneously inducing direct cytotoxicity via MMAE and immune activation.These mechanistic strengths have also been confirmed in clinical trials. In the EV-302/KEYNOTE-A39 Phase 3 study, the combination therapy of Padcept and Keytruda achieved a median overall survival (OS) of 31.5 months in treatment-naïve urothelial carcinoma patients. This figure is approximately double that of the chemotherapy group, which recorded 16.1 months.Based on these results, the National Comprehensive Cancer Network (NCCN) recommends Padcev + Keytruda as a Category 1 preferred first-line regimen, positioning it as an option capable of replacing existing immuno-oncology drug + chemotherapy focused treatment strategies.ADC + Immuno-oncology drugs take center stage… shifts maintenance therapy-centric structureIf the Padcev + Keytruda combination regimen is actually reimbursed, there is a high likelihood that the combination could shift the treatment axis in urothelial carcinoma.Currently, various options coexist in the first-line treatment setting for urothelial carcinoma, including the combination of ‘Opdivo (nivolumab)’ and GemCis (gemcitabine + cisplatin) and the ADC + immuno-oncology drug combination.In addition, a sequencing strategy, which involves maintenance therapy with Merck’s ‘Bavencio (avelumab)’ after chemotherapy, has also established itself as a major pillar. Among the therapies, Bavencio is currently the only reimbursed option.Merck has emphasized adopting a sequencing strategy in which Bavencio maintenance therapy is administered after chemotherapy, followed by Padcev upon disease progression.In fact, real-world data (RWD) from multinational studies such as Japan’s JAVEMACS, the U.S.’s PATRIOT-II, and France’s AVENANCE showed that the median overall survival (OS) with Bavencio maintenance therapy exceeded 30 months, with some analyses reporting survival extended to over 40 months.Furthermore, in strategies where ADC is used following Bavencio maintenance therapy, OS exceeded 41 months, supporting long-term survival through sequential treatment.Ultimately, the future treatment landscape is likely to evolve into competition between potent combination therapy in the first-line setting and maintenance-based sequencing strategies.Whether or not reimbursement is approved is expected to serve as a key factor that goes beyond the simple addition of a treatment option. It is likely to reshape the very paradigm of bladder cancer treatment.
- Company
- Medtronic, 2nd generation Micra landing shifts the system
- by Hwang, byoung woo Apr 06, 2026 03:51pm
- Leadless pacemakers are shifting from a 'supplementary technology' to a variable that is fundamentally changing treatment structures in South Korea.The trend points to a convergence of technological advancements (improved battery life and procedural safety) and institutional changes, such as expanded insurance reimbursement. These factors are transforming access to treatment from a limited scope to a mainstream clinical reality.Medtronic Korea held a press conference on the 2nd for domestic launch of the 2nd generation Micra (Micra AV2), presenting these significant shifts.(From left: Ji Eun Song, Director at Medtronic Korea; Professor Hee Tae Yu, Cardiology, Severance Cardiovascular Hospital; Kangho Park, Marketing Manager at Medtronic Korea)Battery·Algorithm Improvements…The 2nd Generation EvolutionThe presentation explained the new product not merely as a new model, but as a turning point where leadless pacemaker technology, having been clinically validated, moves to its next stage.Since its introduction in 2015, Micra has been used to treat over 400,000 patients worldwide, accumulating data from 50,000 patients and over 450 studies. A 5-year follow-up study showed a major complication rate of approximately 4.5%, with no reported cases of device removal due to infection.Ji Eun Song, Senior Marketing Director of Cath Lab at Medtronic KoreaJi Eun Song, Senior Marketing Director of Cath Lab at Medtronic Korea, stated, "We are no longer at the stage of discussing whether the technology is possible. We are now at the stage of considering how far its application can be extended."The advancements in Micra AV2 can be summarized in three areas: battery, algorithms, and the delivery system.The most significant change is the battery life. The Micra AV2 lasts approximately 15.6 years and the VR2 approximately 16.7 years, representing improvements of 44% and 36%, respectively.Song emphasized. "Considering that we mostly have elderly patients, the reported figure indicates 80% of patients can maintain their treatment with a one-time treatment," adding, " This is not just a performance improvement; it is a change that impacts the treatment strategy itself."We have also improved algorithm. Atrial mechanical sensing has been refined, allowing for stable atrioventricular (AV) synchrony even at high heart rates, with the maximum tracking rate expanded to 135 bpm.Furthermore, the delivery system was upgraded with a rounded catheter tip, reducing pressure on the heart wall by up to 66%. Simulation-based analysis also suggested a potential reduction in perforation risk.Song stated, "As the heart-mechanical signaling monitoring function is improved, the device can now stably relay signals in a wider range of heart rates," adding, "Previously, device selection depended on patient conditions. Now, the latest improvement widened the range that a sing device can cover."Impact of expanded reimbursement…changes brought by clinical introductionClinical experts have also offered positive evaluations regarding the expanding role of leadless pacemakers.Professor Hee Tae YuProfessor Hee Tae Yu of Cardiology at Severance Cardiovascular Hospital stated, "Leadless pacemakers have opened up treatment possibilities for patients for whom conventional transvenous pacemakers were difficult. They are effectively an essential option for patients at high risk of infection or those with difficult venous access."Yu added, "The extended battery life and improved algorithms increase the consistency and predictability of treatment outcomes," and explained, "It is meaningful for long-term strategies."The domestic launch of Micra AV2 is particularly noteworthy as it coincides with the reform of the insurance coverage criteria for leadless pacemakers.As of December 1 last year, the Ministry of Health and Welfare limited the patient co-payment rate to 5% for cases where transvenous electrode insertion is impossible or has failed (e.g., venous stenosis, occlusion, or congenital malformations) and for patients with a current or past history of Cardiac Implantable Electronic Device (CIED) infection.Professor Yu noted, "With reimbursement currently applied to high-risk groups, the range of choices for leadless pacemakers in clinical settings has clearly widened. As more clinical data accumulates, there is a possibility that the target population will gradually expand."Future scope of application…coexistence with transvenous systemsDespite the system's expansion, reimbursement limitations remain a key issue. During the Q&A session, the scope of application emerged as a more central topic than the technology itself.Photos of Medtronic's implantable cardiac devicesProfessor Yu stated, "From a purely medical judgment perspective, it would be ideal to have no reimbursement restrictions. There are cases where a leadless pacemaker is more suitable, yet criteria limit the choice."In particular, Yu noted that elderly patients could be important candidates and emphasized the need for ongoing discussions on expanding coverage as clinical experience grows. However, the current application of essential coverage for high-risk groups was evaluated as a meaningful institutional starting point.Regarding traditional pacemakers, a period of coexistence is expected for leadless pacemakers and "At this stage, leadless pacemakers are not the primary choice for all patients," Professor Yu explained. "The role of transvenous pacemakers still exists." The transvenous method allows adjustment of electrode positions to maintain a more physiological conduction path, remaining a crucial option for younger patients or those who will be dependent on a pacemaker for a long time.In conclusion, Yu noted, "While leadless pacemakers are advancing rapidly, the current structure where they share purposes and coexist with transvenous pacemakers will be maintained for now. However, if leadless technology capable of physiological pacing is secured in the future, the scope of application could expand even further."
- Policy
- INN prescribing bill may be resubmitted to April subcommittee
- by Lee, Jeong-Hwan Apr 06, 2026 03:51pm
- 소병훈 보건복지위원장Attention is mounting within the healthcare and pharmaceutical sectors on whether a bill mandating limited international nonproprietary name (INN) prescribing for essential medicines or drugs with unstable supply will be reviewed by the National Assembly’s Health and Welfare Committee’s legislative subcommittee in April.The bill was included on the agenda of the Health and Welfare Committee’s legislative subcommittee last March, but did not get a chance to be reviewed as it was pushed back by other bills.On the 3rd, lawmakers from the Democratic Party of Korea have emphasized the need to convene the subcommittee in April to discuss bills under their purview that were not reviewed last month.As it is highly unlikely that the subcommittee will convene in May, just one month before the June 3 local elections, the Democratic Party of Korea members of the Welfare Committee saw a strong need to expedite the review of bills this month.Currently, the Health and Welfare Committee is led by Rep. Byung-hoon So (Gwangju-gap, Gyeonggi Province; third-term), who took over as the new chair following the resignation of former Chair Rep. Ju-min Park, who stepped down to run in the Democratic Party’s primary for the Seoul mayoral race.Accordingly, Chair Byung-hoon So, Democratic Party Executive Secretary Soo-jin Lee, and People Power Party Executive Secretary Mi-ae Kim are expected to begin discussions on the schedule for the April subcommittee meeting.Once the subcommittee meeting is confirmed, the bill mandating the limited use of INN prescribing, which was not reviewed last month, is highly likely to be placed on the agenda.Last month, on the day of the subcommittee meeting, the Korean Medical Association (KMA) held a “Rally to Block INN Prescriptions” on the steps in front of the National Assembly Main Building to pressure the Health and Welfare Committee.At that time, KMA President Taek-woo Kim made it clear that the association would take strong collective action if the bill were to be formally introduced.KMA President Taek-woo Kim led the rally to block the INN prescribing bill on the steps in front of the National Assembly Main Building on the 11th of last month.In particular, President Kim maintains a hardline stance that the bill must not be tabled at the April subcommittee meeting. The KMA is currently using the threat of a general doctors’ rally as leverage to block the review of the limited mandatory INN prescribing bill.However, the Democratic Party argues that the INN prescribing bill is part of President Lee’s campaign pledge and a national policy agenda adopted after his inauguration. They maintain that legislation is necessary to improve public access to medicines.A committee official stated, “The Democratic Party is calling for the need to convene the April subcommittee, but whether it will actually take place has not yet been finalized. It will be determined soon following consultations between the ruling and opposition party floor leaders, taking into account the schedule for the June 3 local elections.”There are three bills related to limited INN prescribing currently pending in the National Assembly: an amendment to the Pharmaceutical Affairs Act proposed by Rep. Yoon Kim of the Democratic Party of Korea, and amendments to the Medical Service Act and Pharmaceutical Affairs Act proposed by Rep. Jong-tae Jang of the same party.
- Opinion
- [Desk View] An odd policy ensuring high-priced biosimilars
- by Lee, Tak-Sun Apr 06, 2026 03:51pm
- If the government's recent decision to cut generic drug prices is aimed at reducing the National Health Insurance (NHI) financial burden, excluding biosimilars from this reform would be contradictory.As high-priced original biologics place a significant strain on NHI finances, promoting the use of lower-priced biosimilars could yield substantial financial savings. Patients could also significantly reduce their financial burden through affordable biosimilars.Major countries are implementing policies to increase biosimilar prescribing rates and dramatically reduce medical expenses. Japan has set a biosimilar market share target of 80% and provides financial rewards for prescriptions.France also encourages biosimilars to account for 70% of outpatient prescriptions and pays physicians a portion of the savings as an incentive.In contrast, South Korea's biosimilar prescription rate is merely 21% as of 2021.Unlike other developed nations, Korea has neither specific targets for prescription rates nor supporting policies. Ironically, the prescription rate remains low, despite the presence of two companies, Celltrion and Samsung Bioepis, that are globally competitive in the biosimilar field.The government attributes the low domestic biosimilar prescription rate to a preference for original drugs. While this is partially correct, it is also partially flawed.Another reason is that the government initially set biosimilar prices high to increase export competitiveness, resulting in a lack of price competitiveness with originals in the domestic market.When a biosimilar is listed for reimbursement, its price is set at up to 80% of the original drug's maximum price. After one year, both the original and the biosimilar are lowered to 70% of the maximum price. This means that the identical pricing structure is also applied to biologics.Consequently, biosimilars sometimes voluntarily lower their prices below the original to gain market competitiveness. However, in a market as small as Korea, the margin for voluntary price reductions by biosimilar manufacturers is limited.For this reason, biosimilar prices, which are 40% to 50% of the original price in global markets, remain at approximately 90% of the original drug price in Korea.This situation reinforces the preference for original drugs due to the negligible price difference and creates reverse discrimination, where only domestic patients bear the burden of high-priced biosimilars.To increase the biosimilar prescription rate, it is necessary to lower the price ratio relative to the original. Under the drug pricing reform, generic drugs will be set at approximately 45% of the original drug's maximum price. However, biosimilars are expected to maintain a guaranteed 70%. It is unrealistic to guarantee a 70% price point while hoping to drive up prescription rates through "low-cost biosimilars" at 40% to 50% of the reference price, as seen in other countries.Because biosimilar prices are kept above a certain level, the margin for price reductions on original drugs is also limited. This places a heavy burden on NHI finances. Even if the prices of cheap generics are cut, the contribution to fiscal savings will be low if the prices of expensive biologics remain unchanged.Despite these issues, the government conversely raised the price weighting from 70% to 80% in 2016 to support the competitiveness of the biosimilar industry. However, it must be recognized that the consumption volume of biologics in the domestic market has changed significantly since 2016. Biologics have now taken over major therapeutic markets, led by products like Prolia, which dominates the osteoporosis market thanks to its efficacy and convenience, and by various immune-oncology agents that have revolutionized cancer treatment.The problem is that these biologics are high-priced compared to synthetic drugs. Despite market growth, competition among biosimilars is also intensifying, and the domestic pricing structure limits the potential for cost savings.The government should first consider abolishing the identical pricing policy and lowering the price weighting.Incentive policies for biosimilar prescriptions, like those in other developed nations, may be necessary. In fact, this is needed not only for biosimilars but also for generic drugs. Significant fiscal savings result from replacing high-priced original drugs.Fundamentally, the government should favor prescribing low-cost generics or biosimilars to encourage companies to lower their prices voluntarily.However, it is unclear why the government continues to push for maintaining the original-generic (biosimilar) identical pricing mechanism while favoring a collective generic price reduction policy. In particular, the rationale for the government's push for a collective reduction in generic prices while maintaining a high-price guarantee policy for biosimilars remains unclear.