- LOGIN
- MemberShip
- 2026-04-26 03:48:13
- Opinion
- [Desk’s View] MFDS should clarify AAP safety message
- by Lee, Tak-Sun Sep 29, 2025 06:08am
- Unforeseen moves by U.S. President Donald Trump are having a considerable impact in Korea. After sudden tariff hikes rattled the Korean economy, an unexpected drug safety issue has now emerged. The domestic healthcare market, which is reliant on overseas drugs, is reeling from Trump-related risks. The controversy began on the 22nd when President Trump stated at a press conference that acetaminophen is not safe for pregnant women. He said, “Acetaminophen, widely known as Tylenol, may increase the risk of autism in children if taken during pregnancy. The U.S. Food and Drug Administration will notify doctors of this, and if necessary, recommend restricting Tylenol use during pregnancy.” Acetaminophen, widely known under the brand name Tylenol (Kenvue), is one of the most commonly used fever reducers and pain relievers in Korea. It is generally regarded as relatively safe for pregnant women and young children, which is why healthcare professionals frequently recommend it to such patients. Trump's remarks appear to be based on a recently published report by a research team at the Icahn School of Medicine at Mount Sinai in the United States. This report suggests a possible link between Tylenol use and autism. However, academic communities in Korea and abroad are pointing out that Trump's statement is premature, as scientific evidence linking acetaminophen to autism remains insufficient. The Korean Pharmaceutical Association stated, “Major global health authorities and academic organizations have made it clear that there is insufficient scientific evidence to support such claims at this time.” The Korean Medical Association also dismissed the claims, citing insufficient evidence. KMA spokesman Sung-keun Kim said in a regular briefing, “There is no scientifically established evidence to support the claim that taking Tylenol during pregnancy causes autism in the fetus.” The same sentiment is echoed overseas. WHO spokesman Tarik Jasarevic told reporters at a press briefing, “Evidence remains inconsistent.” The European Medicines Agency (EMA) also stated in a release, “Based on the evidence available to date, no association has been found between the use of paracetamol (the active ingredient name for acetaminophen in Europe) during pregnancy and autism.” However, confusion persists as the US Food and Drug Administration (FDA), the regulatory authority for Tylenol’s home country, has yet to issue an official statement. The stance of the Ministry of Food and Drug Safety (MFDS) is also ambiguous. While the MFDS stated it would receive relevant data from manufacturers and discuss the matter, it has not issued a clear message. It did note, however, that under current approval guidelines, if a pregnant woman experiences a persistent fever above 38°C in early pregnancy, it could affect fetal neural development. In such cases, acetaminophen-based fever reducers and pain relievers may be taken, but the dosage should not exceed 4,000 mg per day. It added that since individual medical situations may vary, pregnant women should consult a healthcare professional before taking any medication containing acetaminophen. This reflects a cautious stance regarding the link between acetaminophen use during pregnancy and autism. This is understood to be a comprehensive reflection of the lack of official statements from the U.S. President, a key ally, and the FDA. Nevertheless, compared to the WHO and EMA stating there is still no clear evidence, this stance appears overly passive. Furthermore, the title of the official press release, “Consult a healthcare professional and take as directed,” seems to shift the burden onto private experts rather than the government. Had the government clearly communicated that, at least for now, evidence is insufficient and that the drug should be taken according to current approved guidelines, it would have alleviated public anxiety. The Ministry of Food and Drug Safety (MFDS), despite being a regulatory body like the FDA or EMA, has faced significant criticism in the past for making decisions based on politics rather than scientific evidence. Of course, it is not entirely independent from government influence, and unlike the FDA or EMA, it lacks manpower and expertise; therefore, direct comparisons may not be fair. Nevertheless, if Korea is to be recognized as a member of the advanced nations and if MFDS truly seeks global recognition as a competent regulatory agency—as it often promotes—then in such controversies, it must deliver clearer, science-first messages. That would undoubtedly strengthen public trust in MFDS by showing that science is prioritized over politics.
- Policy
- MoHW and NHIS agree on need to expand expedited listing
- by Jung, Heung-Jun Sep 29, 2025 06:08am
- The Ministry of Health and Welfare (MoHW) expressed consensus on the need to expand fast-track reimbursement to improve access to treatments for rare and severe diseases. As the government agenda already includes system improvements to reflect the innovative value of new drugs, the ministry stated its intent to support these reforms. On the 26th, at a forum on improving the operation of the National Health Insurance finance hosted by Representatives Mi-hwa Seo and Jong-tae Jang, the government, industry, and academia all voiced the need to expand fast-track reimbursement for rare disease treatments. Yeon-sook Kim, Director-General of the Pharmaceutical Management Division at MOHWYeon-sook Kim, Director-General of the Pharmaceutical Management Division at MOHW, said, “Rare and severe diseases are difficult to diagnose, and the small patient population leads to insufficient data. We do regret how the listing process takes a long time, and communication regarding system improvements has been slow. We will gather opinions to develop the system rationally.” Kim added, “This is also included in the government's national agenda. We have decided that the drug pricing system will support the creation of an ecosystem for innovative new drug development by reflecting the innovative value of new drugs. This also includes alleviating the burden of rare and intractable diseases.” "Our goal is to ensure that more necessary drugs are covered quickly through expedited listing and to broaden coverage. Currently, we are also attempting to accelerate the process by concurrently handling approval and listing. The national agenda also comprehensively includes improvements to the drug pricing system. However, as it requires significant social consensus and careful consideration, we will need time to discuss improvement measures." The National Health Insurance Service (NHIS) emphasized the need for a roadmap to prioritize reimbursement and use resources more efficiently. Yoo-kyung Yoon, Director of Pharmaceutical Management at NHISYoo-kyung Yoon, Director of Pharmaceutical Management at NHIS, said, “There are limitations in terms of budget and review manpower, but I agree expansion is necessary. We recognize the importance of prioritization. We need to review reimbursed drugs, set reimbursement priorities, and establish a roadmap for efficient fiscal use.” “We must determine how to select drugs eligible for fast-track, identify issues as the system is implemented, and continuously improve it to ensure prompt reimbursement can be achieved. Adjusting the reimbursement scope requires social consensus, so we will thoroughly gather opinions from stakeholders.” Yoon also emphasized, “Improvements to the generic drug pricing system must also be considered alongside measures to foster a virtuous cycle in the industry. Rapid listing of rare and intractable disease drugs is included in national policy tasks, and we will strive to develop solutions.” The industry expressed that establishing a virtuous cycle structure is urgently needed to enable the development of innovative new drugs for rare and severe diseases. Jae-won Heo, Executive Director at Gilead Sciences Korea Jae-won Heo, Executive Director at Gilead Sciences Korea, noted, “Hepatitis C, which can progress to liver cancer, already has curative treatments. If patients are treated early, it can actually reduce the financial burden on the NHIS. Data also shows that 20% of cancer patients give up economic activity, devoting much of their time to caregiving. Supporting their return to society carries significant value.” Heo explained, “The number of patients is small, but development is extremely difficult, and companies inevitably face heavy burdens. Even after more than 10 years of research, it is not uncommon to see results showing no clinical effect. Despite failures, companies continue to develop treatments because patients exist. A virtuous cycle must be established so development is feasible,” urging expansion of new drug access. Professor Yong-jin Kwon of Seoul National University Hospital Criticism also emerged that the government should not show a passive attitude toward coverage for rare and severe diseases, and that Aative review of the generic drug pricing system is also necessary. Professor Yong-jin Kwon of Seoul National University Hospital's Public Healthcare Center pointed out, "New drugs are approved, but they aren't even used as non-reimbursed treatments, so they don't show up in the statistics. The coverage rate appears high, but that's because no treatment exists. In reality, the coverage rate for rare diseases isn't high. Furthermore, care costs are not factored in.“ Kwon further criticized, “NHIS does not examine how much value has been generated (so far) from the high prices paid for generics and the development of innovative R&D treatments. How much have domestic pharmaceutical companies advanced over the past 25 years? We need to evaluate the outcomes and discuss the development of the pharmaceutical industry.” stressing the need to reform the generic pricing system.
- Policy
- “Cut prices of generic drugs across the board”
- by Jung, Heung-Jun Sep 29, 2025 06:07am
- A proposal has been made to establish reimbursement priority for treatments targeting rare/serious diseases versus mild conditions, thereby expanding access to new drugs. There were also calls to reform the distorted pharmaceutical budget structure by cutting generic prices across the board and canceling approvals for products lacking bioequivalence data. At a National Assembly forum on improving the operation of health insurance finances for rare and severe diseases, hosted on the 26th by lawmakers Mi-hwa Seo and Jong-tae Jang, participants stressed the need to allocate limited insurance resources more effectively to improve access to new drugs. Prof. Yong-jin Kwon of Seoul National University Hospital’s Public Healthcare Center Professor Yong-jin Kwon of Seoul National University Hospital’s Public Healthcare Center said, “The National Health Insurance system has reached a structural contradiction. While pharmaceutical spending exceeds the OECD average, access to innovative drugs remains restricted, depriving patients of treatment opportunities. Coverage for rare and severe diseases should have expanded, but instead, it has regressed.” Professor Kwon called for ▲Reestablishing reimbursement priorities, ▲reforming the drug management system , and ▲expanding access to new drugs. He explained that a survey conducted last July of 1,000 citizens showed significant public agreement on prioritizing coverage for patients with rare and severe diseases. According to the results, 46.7% agreed with prioritizing severe disease patients, and 52.7% supported prioritizing rare disease patients. However, 76.9% responded that while premiums should be maintained at the current level, coverage should be differentiated. Prof. Kwon said, “This suggests there is sufficient basis to regard reprioritization as being highly feasible.” Professor Kwon proposed the following improvement measures ▲establishing a National Health Insurance Priority Committee with public participation ▲implementing blanket price reductions for generic drugs and fostering competition, and ▲introducing a fast-track system for rapid listing and flexible benefit determination. Prof. Kwon said, “The share of pharmaceutical expenditures is already high, but the portion spent on new drugs is low. The generic market is driving distortion. We should consider whether this is due to high prescription volumes or high generic prices,” stressing the need to shift reimbursement priorities from mild to severe conditions. He added, “Prioritization should consider disease severity and social costs, as well as risks of treatment delays and potential market failures.” He also argued that generic drug prices should be cut across the board, and generics lacking bioequivalence testing should have their approvals revoked. He stated, “It is unworthy of our national standing that drugs without bioequivalence certification are still circulating. Bioequivalence test results should be made public. Citizens must be convinced that the efficacy and composition are identical.” Furthermore, he called for expanding fast-track reimbursement and flexible decision-making for rare disease drugs. Suggestions included accelerating reviews, granting conditional approvals, and enhancing post-marketing management through fast-track pathways. He concluded, “We must streamline the health technology assessment process and implement conditional approvals. If MFDS approval represents the product, insurance reimbursement represents the technology. Even if not yet officially authorized, reimbursement should be possible based on technological appropriateness. For rare diseases, conditional approval and reimbursement must be adopted, and real-world evidence (RWE) should be leveraged for more sophisticated post-market management.” He added, “Flexible reimbursement frameworks must be expanded. Risk-sharing agreements (RSA) should be applied diversely, such as on a performance-based basis. Patients should also understand that the limited coverage can be gradually expanded over time.”
- Company
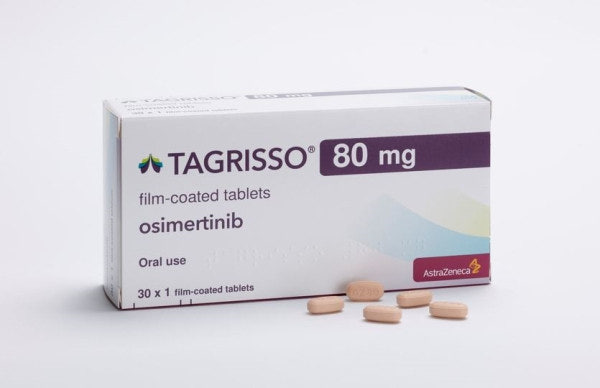
- CKD and Kwang Dong win Tagrisso formulation patent suit
- by Kim, Jin-Gu Sep 26, 2025 06:14am
- Generic drugmakers challenging AstraZeneca's patent for the non-small cell lung cancer treatment ‘Tagrisso (osimertinib)’ have won their case in the first instance. According to industry sources on the 25th, the Intellectual Property Trial and Appeal Board (IPTAB) on the 24th ruled in favor of Chong Kun Dang and Kwang Donng Pharmaceutical in their request for a negative right scope confirmation trial regarding Tagrisso’s formulation patent (No. 10-2336378). This significantly increases the possibility of an early launch of Tagrisso generics. The two companies have also met 2 key requirements for obtaining exclusive marketing rights (first generic exclusivity): ▲ being the first to file the trial request and ▲ winning the trial/litigation. Now, they only need to satisfy the condition of being the first to file for generic approval to obtain the first generic exclusivity right. CKD and Kwang Dong are the only companies to have challenged the Tagrisso formulation patent. If both secure the first approval for their generics and gain the first generic exclusivity rights, they will be able to sell their product exclusively for 9 months. The key variable is AstraZeneca’s appeal. If AstraZeneca files a lawsuit to overturn the IPTAB decision with the Patent Court, the dispute may be prolonged. AstraZeneca's decision on whether to appeal has not yet been made. Tagrisso is protected by three patents: substance patents expiring in November and December 2033, and a formulation patent expiring in January 2035. CKD and Kwang Dong have successfully avoided the formulation patent. With the formulation patent out of the way, both companies plan to launch their generics as soon as the substance patent expires in 2033. There is also speculation that they could aim for an even earlier launch by targeting the extended duration granted to the substance patent. Tagrisso is a targeted anticancer drug used for EGFR-mutated non-small cell lung cancer (NSCLC) that received domestic approval in 2016. It is used as a first-line treatment for patients with locally advanced or metastatic NSCLC harboring EGFR gene mutations. In Korea, it competes with Yuhan Corp’s Leclaza (Lazertinib). According to the market research institution IQVIA, Tagrisso’s sales in Korea reached KRW 111 billion in 2023. After surpassing KRW 100 billion in annual sales in 2022, growth has continued steadily. With reimbursement expanded last year to include first-line treatment for locally advanced and metastatic NSCLC patients with specific EGFR mutations, sales are estimated to have exceeded KRW 130 billion. Separately, CKD is developing its own new drug for non-small cell lung cancer. The candidate compound, named ‘CKD-702’, is a bispecific antibody targeting both cMET and EGFR. It is currently undergoing global Phase I clinical trial. CKD is seeking to strengthen its foothold in the NSCLC treatment market by developing both a new drug and a generic.
- Opinion
- [Reporter’s View] The gap between innovation and access
- by Son, Hyung Min Sep 26, 2025 06:12am
- Advances in medicine have created pivotal turning points in the course of human survival. Diseases once deemed incurable are gradually being reclassified as chronic conditions. From anticancer drugs to treatments for rare diseases and immunotherapies, innovative new drugs have not only prolonged patients’ lives but also increased the burden of responsibility borne by nations and societies. The problem lies in the fact that the ‘pace of innovation’ and the ‘pace of patient access’ are not on the same track. Korean patients are always left to wait. Even when news arrives that a new drug has been approved in the US or Europe, a gap of 1 to 3 years often exists before patients can actually receive a prescription domestically. This delay is not merely a procedural issue; it represents a lost opportunity for treatment. For a terminal cancer patient, 1 year can be their entire life. This is why it's not uncommon for patients to seek treatment abroad. At the center of this irony lies a uniquely Korean formula: price over innovation. The value of a new drug is first calculated by its burden on the national health insurance budget rather than by its clinical significance and impact on patient survival. While managing insurance finances is clearly a crucial task in national governance, the balance has tilted excessively toward fiscal restraint, depriving patients of the opportunity to timely benefit from innovations. This is also why pharmaceutical companies often push Korea down the priority list in their global launch strategies. The so-called ‘Korea passing’ concern is not an abstract warning but a real risk that delays actual patients' treatment opportunities. The global environment is not favorable either. President Trump’s MFN (Most Favored Nation) drug pricing policy has posed a threat to pricing systems worldwide. Under the pretense of protecting American patients, it targeted countries like Korea that maintain low drug price systems as risk factors. From the perspective of multinational pharmaceutical companies, the incentive to launch drugs in Korea has diminished because protecting prices in the US market has become more critical. In other words, Korea’s low drug prices translate directly into being deprioritized in global market strategies. This leads us to a fundamental question: what is a new drug to the patient? To the government, it may be a budget variable; to companies, a profit variable. But to patients, a new drug is a survival variable. Unless the perspective shifts from “how cheaply can we bring it in” to “how quickly and fairly can it reach patients,” the meaning of innovation becomes powerless in front of patients. Of course, the constraints of the national health insurance budget are an undeniable reality. Within limited resources, it's difficult to unconditionally recognize the value of new drugs and raise their prices. The government isn't sitting idle either. New attempts are being discussed, such as the approval-evaluation linkage pilot project, expansion of risk-sharing schemes, and recently, indication-based pricing. But the fundamental limitations remain. Within the current system, patient access to new drugs inevitably remains low. A radical policy shift is now needed. So what constitutes as ‘radical’? Suggestions include introducing value-based assessment that prioritizes clinical innovation and patient survival outcomes; implementing multi-layered risk-sharing schemes where government, pharmaceutical companies, and society share burdens; and establishing a national strategy vision that enhances international negotiation power and improves patient access. Furthermore, a paradigm shift is needed—one that recognizes healthcare not merely as a fiscal issue, but as a core national competitiveness factor. Medical innovation will not cease. The problem is that the speed at which this innovation reaches Korean patients remains sluggish. How long can we tolerate the paradox of patients lagging behind in this era of innovation? Now is the time for government, industry, and society to find answers together. A decisive policy action to align the speed of innovation with patients’ needs is urgently required—so that patients no longer have to waste their time waiting.
- Company
- Teva-Handok challenges mkt with LAI risperidon, Uzedy
- by Hwang, byoung woo Sep 26, 2025 06:12am
- As the schizophrenia treatment paradigm shifts toward managing medication adherence, Teva-Handok has introduced Uzedy (risperidone), a long-acting subcutaneous containing risperidone, to the Korean market. Uzedy is expected to become a new treatment option, enhancing patient convenience with its 1-month and 2-month dosing options and a design that eliminates the need for a loading dose. This drug has been shown to reduce the risk of relapse by up to 80% compared to placebo. Uzedy logoTeva-Handok recently announced that its long-acting subcutaneous injectable for adult schizophrenia, Uzedy (risperidone), received approval from the Ministry of Food and Drug Safety (MFDS) on September 5. It is assessed as a new treatment option that overcomes the medication adherence issues associated with existing oral therapies and provides convenience for both patients and medical professionals. Notably, it is expected to contribute to securing 'treatment persistence,' which is critical in schizophrenia management. Uzedy is an long-acting injectable that can be administered at 1-month and 2-month intervals, developed specifically to address poor medication adherence, cited as the primary cause of schizophrenia relapse. Schizophrenia is a chronic, progressive mental illness affecting thought, emotion, and behavior, with about 80% of patients experiencing multiple relapses within the first five years of treatment initiation. Since repeated relapses can diminish treatment effectiveness, impair daily functioning, and even cause structural changes in the brain, consistent medication is essential. Uzedy's differentiation lies in its proprietary technology that eliminates the need for a separate high-dose initiation or oral supplementation during the initial treatment phase. Previous long-acting injectables required a high-dose loading dose or co-administration of oral medication for a certain period to reach therapeutic concentration levels. However, Uzedy is designed to achieve an effective blood concentration rapidly within 24 hours of administration using a special polymer technology, allowing for a fast onset of therapeutic effect. Professor A of Neuropsychiatry at a tertiary general hospital in Seoul explained, "The long-acting formulation can resolve the medication adherence issue where patients, due to low insight into their illness, stop taking their medication," and added, "Compared to daily oral medications, it maintains stable drug concentration in the blood, which is beneficial for maximizing therapeutic effect and minimizing the occurrence of side effects." Professor A also said, "This drug alleviates the patient inconvenience of having to take pills daily and the social burden of having to expose one's illness to others, thereby assisting with social reintegration and job retention." Risperidone, Uzedy's active ingredient, is a second-generation antipsychotic developed in the 1990s, with long-proven efficacy and safety in clinical settings. With the introduction of Uzedy, the schizophrenia long-acting injectable (LAI) market in Korea is expected to become a four-way competition. Following existing LAIs based on haloperidol decanoate (1st-generation), paliperidone (2nd-generation), and aripiprazole (3rd-generation), the addition of risperidone-based Uzedy is expected to provide diverse treatment options for schizophrenia patients. Given that some existing treatments offer longer dosing intervals than Uzedy, Uzedy's market establishment and competition will be linked to the overall therapeutic standing of risperidone. However, reimbursement listing is essential for Uzedy to expand its influence in the domestic schizophrenia treatment market. Teva-Handok said, "We have a plan for Uzedy's reimbursement and will follow the standard procedure for securing reimbursement after approval." Additionally, improving the perception of the LAI formulation, which currently has a low prescription rate in Korea, will be a challenge for Teva-Handok. Professor A said, "Research indicates that some clinicians avoid prescribing LAIs due to concerns that it might strain the patient-physician relationship or lead to criticism over forced injections," and stressed, "To increase the prescription rate, we need to eliminate this perception and for physicians to provide treatments they believe are necessary with a sense of responsibility." Hee Kyung Ahn, CEO of Teva-Handok, added, "Uzedy is expected to contribute to improving the quality of life for patients who struggle with long-term treatment due to low medication adherence by offering flexible dosing options and a rapid therapeutic effect simultaneously."
- Policy
- HIRA, "Will enhance the monitoring of rare disease drugs"
- by Jung, Heung-Jun Sep 26, 2025 06:12am
- With the rapid increase in newly emerging treatments for rare and severe diseases, there have been suggestions for establishing sustainable systems, such as strengthening post-market management and creating a separate dedicated fund. It was explained that monitoring uncertain evidence resulting from expedited approvals and improving patient access through a separate fund, similar to overseas models, are necessary steps. On September 25, the Health Insurance Review & Assessment Service (HIRA) hosted a symposium at the St. Mary's Hospital Seong-ui Hall in Seoul on the future direction and social ethics of rare and severe disease treatment. Lee So-young, Director of HIRADuring the symposium Lee So-young, Director of HIRA's Pharmaceutical Performance Assessment Division, said that as rare disease treatments rapidly increase, not only Korea but also other countries are deliberating on management strategies. In the United States, 52% of new drug approvals are for rare disease treatments, and the FDA operates four expedited tracks to address unmet medical needs. However, Lee pointed out that problems are arising where expedited approval, often based on surrogate endpoints, does not ultimately improve patient access or where research finds the drug provides no actual benefit. Lee explained, "The FDA is also aware of the problem. Since the year before last, they have required that when approval is based on surrogate index, a confirmatory clinical trial must be initiated or clearly planned," and added, "They have also reinforced measures to allow for rapid withdrawal of approval if the requirements are not met or if the anticipated clinical benefit is not realized." Lee emphasized that it is time for Korea to move beyond viewing rare disease treatment as an exceptional case and start considering a sustainable system. Lee proposed three strategies: ▲Conditional reimbursement based on evidence generation ▲Establishing a separate dedicated fund ▲Improving reimbursement criteria and pre-and post-market management. Regarding conditional reimbursement, Lee said, "The legal basis is established, and the guidelines will be released in November this year. This is a structure where a drug is listed and covered on the condition that post-market evaluation is conducted, and the post-market management tracks the extent of evidence uncertainty and whether that uncertainty can be eliminated." Lee added, "The UK classifies drugs into those that should or should not be listed through the Cancer Drug Fund. They have also established an Innovative Medicines Fund. Taiwan and Australia operate similar funds," proposing the establishment of a separate fund in Korea. Lee concluded, "Currently, reimbursement management is conducted at the patient level. There is a need for monitoring at the drug and disease level, with performance management based on those results,"and added, "It's difficult for pharmaceutical companies alone to gather and compile all the data. The EU also operates its system through transnational cooperation," and stressed the importance of a cooperative framework for strengthening post-market management.
- Policy
- Legislation of restricted INN Prescriptions gain momentum
- by Lee, Jeong-Hwan Sep 26, 2025 06:11am
- With the ruling party accelerating legislation of “restricted international nonproprietary name (INN) prescriptions,” which was one of President Jae-myung Lee’s campaign pledges, the medical community is showing visible unease. Democratic Party of Korea lawmakers In-soon Nam, Young-seok Seo, Yoon Kim, and Jong-tae Jang, along with Rebuilding Korea Party lawmaker Sun-min Kim, announced that they will host a policy forum on September 30 at the National Assembly under the theme “Introducing a Korean Model for INN Prescriptions.” In response, doctors’ associations have directly talked with Rep. Joo-min Park, chair of the NA Health and Welfare Committee, and are planning a protest rally. On the 24th, the Seoul Medical Association said it would hold a “Seoul Medical Association Representatives’ Rally Against INN Prescriptions” on September 26 at 7:30 a.m. at its headquarters. Participants will include the members of its executive board, auditors, the council’s steering committee, and presidents and executives of local medical associations. The day before, the Seoul Medical Association President Kyu-Seok Hwang visited NA Health and Welfare Committee Chair Joo-min Park's office on the 23rd for a meeting and conveyed their position on how the INN-based prescription policy threatens the sustainability of primary care. Doctors argue that since generic substitution is already legally guaranteed, further mandating INN prescriptions would jeopardize patient safety and undermine the foundation of Korea’s doctor-pharmacist separation system. They also contended that trying to address drug supply shortages through INN prescriptions is not a fundamental solution, and that the clause stipulating penalties of up to 1 year imprisonment or fines up to KRW 10 million is excessive. Nonetheless, the ruling party maintains the position that legislation is inevitable to resolve the harm to patients caused by shortages of essential and unstable supply of medicines. The lawmakers co-hosting the INN prescription forum with the Korean Pharmaceutical Association and the Korea Institute for Pharmaceutical Policy Affairs include not only pharmacist-turned-lawmaker Young-Seok Seo but also physician-turned-lawmakers Yoon Kim and Sun-min Kim, indicating broad support on the need for its institutionalization. The ruling party lawmakers recognize that the bill on restricted INN prescribing (led by Representative Jong-tae Jang), which is currently pending in the National Assembly, is far removed from undermining the intent of the separation of medical and pharmaceutical practices or threatening patient safety. This is because the bill proposes establishing a ‘Supply Management Committee for Medicines with Unstable Supply’ under the Ministry of Health and Welfare, involving both pharmacists and doctors, to designate out-of-stock drugs and permit generic prescribing only for those designated drugs. Lawmakers argue that legislation on restricted INN prescriptions must focus on easing patient inconvenience and improving access to medicines, rather than fueling conflicts over professional boundaries between doctors and pharmacists. A ruling party official said, “The restricted INN prescription bill should prioritize the public over doctors and pharmacists. The bill establishes a new committee to designate medicines with supply shortages subject to INN prescribing, and institutionalizes a management system requiring pharmaceutical companies, wholesalers, pharmacies, and physicians to submit information on such shortages. The goal is to resolve the long-standing inconvenience faced by the public.”
- Policy
- PVA monitoring for high-priced drugs conducted in Q4
- by Jung, Heung-Jun Sep 25, 2025 06:12am
- High-priced anticancer drugs, including Keytruda and Opdivo, have been placed under monitoring for price-volume agreements (PVA, Type A·B) in the 4th quarter. On the 23rd, the National Health Insurance Service (NHIS) released ‘prior information on the Q4 monitoring list for drugs subject to PVA (Type A·B).’ A total of 111 items were listed, including many blockbuster products from multinational pharma companies such as ▲ Novartis Korea’s Zolgensma (onasemnogene abeparvovec), ▲ MSD Korea’s Keytruda (pembrolizumab), ▲ Ono Pharmaceutical Korea’s Opdivo (nivolumab) 20mg, 100mg, 240mg, ▲ Roche Korea’s Alecensa (alectinib HCl) 150mg, ▲ Sanofi-Aventis Korea’s Dupixent (dupilumab) 200mg, 300mg. Also, products from Korean pharmaceutical companies on the list include: ▲ Celltrion’s Donerion Patch (donepezil) 87.5mg, 175mg, ▲ GC Biopharma’s Denol (bismuth subcitrate potassium), ▲ Bukwang Pharma’s Agio Granule, ▲ Dongindang Pharma’s LecClean Solution (sodium phosphate) 133ml, 1000ml, ▲ Ildong Pharmaceutical’s Pirespa Tab (pirfenidone) 200mg, and ▲ Boryung Corp’s Kanarb (fimasartan potassium trihydrate) 30mg, 60mg, 120mg. The NHIS said, “Claims filed for the monitored drugs will be analyzed, and if they meet the negotiation criteria, they will be designated as subjects for price-volume agreement negotiations.”
- Company
- Twice-yearly 'lenacapavir' for HIV expected to land in KOR
- by Eo, Yun-Ho Sep 25, 2025 06:12am
- Product photo of lenacapavir 'Lenacapavir,' a HIV prevention drug taken twice a year, is expected to be marketed in Korea. According to industry sources, the Ministry of Food and Drug Safety (MFDS) is currently reviewing the approval of lenacapavir from Gilead Sciences Korea. The drug was designated as an orphan drug in January. Its specific indication is "a combination therapy with other antiretroviral agents for the treatment of multidrug-resistant HIV-1 infection in adults who are not being treated with their current antiretroviral therapy." This drug, marketed overseas under the brand name Sunlenca, is the first long-acting HIV-1 capsid inhibitor and is administered as a subcutaneous injection every six months. It was approved in countries like the United States and Europe in 2022 and is currently being prescribed. Current HIV treatment is maintained through daily oral administration of antiretroviral drugs. However, with the development of long-acting formulations, the administration frequency is advancing to once every two months or once every six months. Lenacapavir is also garnering more attention for its potential in HIV 'prevention,' not just treatment. In June, this drug received approval in the U.S., and more recently in Europe, for pre-exposure prophylaxis (PrEP) to reduce the risk of sexually acquired HIV-1 infection in at-risk adults and adolescents weighing at least 35 kg. The product name for lenacapavir used in prevention is 'Yeytuo.' The efficacy of lenacapavir for prevention was proven through the Phase 3 PURPOSE 1 and PURPOSE 2 studies. The PURPOSE 2 study results showed that lenacapavir reduced HIV infection by 96% compared to the background HIV incidence (bHIV). In the study, 2 cases occurred among 2,180 participants, meaning that 99.9% of the lenacapavir arm did not contract HIV. Last year, Gilead also prematurely unblinded its PURPOSE 1 trial, which evaluated lenacapavir as PrEP in cisgender women in Sub-Saharan Africa, after it met its primary efficacy endpoint. Meanwhile, the international science journal and news Science selected lenacapavir as its 'Science Innovation of the Year' last year based on these research results.