- LOGIN
- MemberShip
- 2026-05-08 13:04:42
- Company
- 3 new asthma drugs resumed discussion on reimbursement
- by Eo, Yun-Ho Jul 10, 2023 05:21am
- Three new asthma drugs, which had been uninsured for at least three years, started the insurance benefit listing process, but only one drug made progress. According to related industries, Handokteva's eosinophilic asthma treatment Cinqair passed the HIRA Pharmaceutical Reimbursement Evaluation Committee. However, GSK Korea's Nucala and Korea AstraZeneca's Fasenra were not considered. These drugs are interleukin (IL)-5 antagonists and have a mechanism of reducing the level of eosinophils, a type of leukocyte involved in the induction of asthma. It received attention at the time of approval as a valid treatment option that did not exist before but was not included in the reimbursement list due to drug price issues. Drugs with the same mechanism started the listing process again at the same time, but the reason for the different results is believed to be that only Cinqair followed the general listing track. For the remaining drugs, companies are known to want to apply a risk-sharing agreement. It remains to be seen whether the two unlisted drugs of this evaluation committee can find a compromise with the government and continue the listing process. There are no registered drugs for severe asthma since Novartis Korea's Xolair entered insurance coverage in 2020. The disease area of 'asthma' looks the same, but three drugs and Xolair are prescribed for allergic asthma. There is a difference in the details of the indications. However, by the government's standards, Xolair became the target of comparison, and the drug's price was unbearable for three new biologics, so the reimbursement listing process was suspended.
- Policy
- Gov’s halts price cut discussions on generics
- by Lee, Jeong-Hwan Jul 10, 2023 05:21am
- Pharmaceutical companies in Korea are carefully monitoring the government's direction in improving the pricing system of generic drugs, including the government's insurance ceiling price policy. The Ministry of Health and Welfare was known to be contemplating a system with the health insurance authorities to further reduce the price of generic drugs after 3 years through a stepped pricing system. However, with no specific movement being observed in that direction for several months, there have been speculations that the government has temporarily halted the pursuit of additional price cuts on generic drugs. On the 7th, the pharmaceutical industry began to assess the atmosphere surrounding MoHW’s drug pricing policy on generics. Previously, MOHW, centering around the 2nd Vice-Minister of Health and Welfare Park Min-Soo, started exploring improvement measures to prevent the mushrooming of generics in the market. One measure mentioned was to further the price reduction imposed on generic drugs. As MOHW’s drug pricing policy aimed to expand accessibility for patients with severe and rare diseases who require high-cost drugs and rationalize the prices of generic drugs that lead to excessive competition in distribution, there was speculation that the upper price limit of 53.55% that was set for generic drugs could be adjusted or the number of differential price reductions for listed drugs with the same ingredients be reduced. However, no progress in the area has been made for several months since the internal meeting was conducted between the MOHW, the Health Insurance Review and Assessment Service, and the National Health Insurance Service regarding the drug pricing policy on generics in April. Therefore, the speculation is that the MOHW is controlling the speed of price reduction of generic drugs. MOHW may have felt it burdensome to create additional measures for the price reduction of generic drugs ahead of the reevaluation of the ceiling price (criteria) that will be held for listed generic drugs. This speculation has been supported by the fact that the scheduled TFT meeting between the MOHW, HIRA, and NHIS for drug pricing policies of generics in June was postponed. However, MOHW has not proclaimed a specific stance regarding the pricing system of generics. This means that it is difficult to hastily judge whether the government has halted its pursuit to impose price cuts on generic drugs. Given the situation, pharmaceutical companies are focusing on the actions of MOHW to formulate countermeasures in line with the administrative direction. An official from a pharmaceutical company stated, “For now, MOHW has halted the scheduled meetings on drug pricing policy on generics with HIRA and NHIS. With the reevaluation of the standards for listed drugs scheduled in the second half of the year, there are speculations that the MOHW may have slowed down its pace in pursuing additional revisions in drug pricing policies on generics. However, some expect partial differential price cuts may be imposed on generic drugs, even if the ceiling price is not adjusted" An official in charge of drug pricing from another pharmaceutical company said, "For the pharmaceutical industry, the news that MOHW has halted additional drug price reductions is a significant development. However, we cannot be at ease until the MOHW presents specific policy directions regarding drug price cuts. Many pharmaceutical companies are preparing various arguments and evidence against drug price cuts." In addition, with the upcoming announcement of the final version of the Second Comprehensive Plan of National Health Insurance this year, pharmaceutical companies are demanding a clearer policy direction from MOHW so that they can increase predictability in order to respond to government policies. A representative from another pharmaceutical company said, “In addition to the drug pricing policies on generics, MOHW has not yet released the final version of its policy on preferential pricing for breakthrough therapies after their discussions with private-public consultative bodies in the first half of the year. As this coincides with the formulation of the Second Comprehensive Plan of the National Health Insurance, pharmaceutical companies are contemplating on how to strategize their management policies accordingly. It would be desirable for the government to gather a wide range of opinions and take actions to prioritize predictability for companies and provide support for future management decisions, rather than being solely driven by political considerations.”
- Company
- New AML drug Vyxeos can be prescribed at general hospitals
- by Eo, Yun-Ho Jul 10, 2023 05:21am
- The new drug ‘Vyxeos’ that was introduced to Korea by Handok Pharmaceuticals may now be prescribed at general hospitals in Korea, According to industry sources, Vyxeos (daunorubicin+ cytarabine), a treatment for adults with newly diagnosed, therapy-related acute myeloid leukemia (t-AML) or AML with myelodysplasia-related changes (AML-MRC), has passed the drug committees (DCs) meetings of several medical institutions in Korea including the National Cancer Center, Samsung Medical Center, Seoul National University Hospital, and Asan Medical Center, and Sinchon Severance Hospital. However, Vyxeos is yet to be reimbursed in Korea. Its reimbursement agenda had been deliberated by the National Health Insurance Service’s Cancer Disease Deliberation Committee last month, but the committee was unable to set the reimbursement standards. Vyxeos was developed by a global pharmaceutical company Jazz Pharmaceuticals headquartered in Ireland, and Handok owns the exclusive rights to its sales in Korea. The overall prognosis of adults with therapy-related acute myeloid leukemia (t-AML) or AML with myelodysplasia-related changes (AML-MRC) is poor, and t-AML or AML-MRC patients have demonstrated low remission rates and shorter overall survival (OS) after intensive chemotherapy compared to other AML patients. Intensive chemotherapy, the 7+3 regimen of cytarabine and daunorubicin, had remained the standard therapy for over 50 years since its introduction in the 1970s. This is why an unmet need existed in the field for some time. Vyxeos is a liposomal formulation of a fixed combination of daunorubicin and cytarabine in a 1:5 molar ratio. Vyxeos liposomes accumulate and persist at a higher concentration in the bone marrow, where they are preferentially taken up intact by leukemia cells, maximizing synergistic antitumor activity. In a Phase III trial that demonstrated the efficacy of Vyxeos, the median overall survival of patients with t-AML or AMLM-MRC that were treated with Vyxeos was 9.6 months, which was longer compared with the 6 months in patients that received the 7+3 arm. Also, 48% of the Vyxeos-treated patients achieved complete remission (CR) and complete remission with incomplete neutrophil or platelet recovery (CRi), which was higher than the 33% in the 7+3 arm. The safety profile in both arms was similar.
- Company
- Daiichi's sales rose & Astellas' sales fell
- by Jung, Sae-Im Jul 10, 2023 05:20am
- Among Japanese pharmaceutical companies that have entered the domestic market, 4 out of 7 subsidiaries with settlements in March expanded their sales. Daiichi Sankyo Korea's sales reached 253.2 billion won, ranking first among Japanese pharmaceutical companies. As a result of analyzing the performance for the 2022 business year (April 1, 2022, to March 31, 2023) of 7 pharmaceutical companies with settlements in March submitted to the Financial Supervisory Service on the 10th, the total sales amounted to KRW 1,115.4 billion, up from 11,557 in the previous year. decreased by 3% compared to the billion won. During the same period, operating profit fell 18% from 97.9 billion won to 80.2 billion won. 4 out of 7 companies succeeded in expanding their top line. Four companies saw an increase in operating profit. More than half improved performance, but the decline in performance at a particular company affected overall performance. Daiichi Sankyo Korea posted 253.2 billion won in sales last year, up 3% from the previous year. It surpassed Astellas Pharmaceuticals Korea and rose to No. 1 among Japanese pharmaceutical companies (including the December settlement). Operating profit fell 16% to 22.1 billion won. Lixiana·Sevikar sales made stable performance.. Since last year, it has been taking on a new challenge with the approval of the anti-cancer drug Enhertu. There were also changes in the members of the organization, such as increasing the number of experts in anticancer drugs. As a result, selling and administrative expenses increased and operating profit decreased. Enhertu is a next-generation antibody-drug conjugate (ADC) that has proven efficacy not only in HER2-positive but also in HER2-low-expressing breast cancer for which there was no treatment. In May, HER-2-positive breast cancer and stomach cancer passed the HIRA committee and benefits became possible. If the benefit is applied within the year, it is expected to have a great impact on Daiichi Sankyo Korea's sales. Takeda Pharmaceutical Korea and Astellas Korea Pharmaceutical, which cost about 200 billion won, obtained conflicting results last year. Takeda Pharmaceutical Korea saw an increase in sales and a decrease in operating profit, while Astellas Pharmaceutical Korea saw a decrease in sales and an increase in operating profit. Last year, Takeda Pharmaceutical Korea's sales were 249.6 billion won, up 8% from the previous year. Operating profit fell 6% to 7.6 billion won. Anticancer drugs such as Zejula, Alunbrig, and Ninlaro contributed to sales expansion with steady growth. However, the decrease in operating profit was mainly due to the increase in the cost of sales. Last year, Takeda Korea's cost of sales was 177 billion won, up 13 percent from 156.4 billion won the previous year. Astellas Pharmaceutical Korea recorded 232.2 billion won in sales last year, down 6% from the previous year. Representative products, such as Betmiga and Harnal, are continuously declining in sales. Instead, the company is pinning its hopes on Xospata, a leukemia drug that succeeded in applying for reimbursement last year. Saving on SG&A expenses, operating profit increased by 16% last year to KRW 17.6 billion. Eisai's sales decreased by 34% from 212.9 billion won in 2021 to 140.5 billion won last year. During the same period, operating profit also decreased by 77% to 5.2 billion won. Sales of existing products such as Lenvima have declined, while new drugs such as Jyseleca have not yet generated significant sales in the market. Eisai, which exceeded 200 billion won in annual sales for the first time in 2019, fell back to the 100 billion won level in three years. Lecanemab is a promising new drug that will bring Eisai back. Lecanemab, jointly developed by Biogen and Eisai, is a drug that can fundamentally treat Alzheimer's disease and is expected to exceed 1 trillion won in global sales by 2027. Lecanemab, which received conditional approval from the FDA last year, was recently approved as an official drug, raising expectations for commercialization. In particular, Eisai, not Biogen, is leading the commercialization of Lecanemab. Eisai submitted an application for domestic approval of Lecanemab last month. Santen Korea recorded 120.2 billion won and 16.9 billion won in sales and operating profit, up 10% and 6%, respectively. Mitsubishi Tanabe Korea had the same sales as the previous year, but its operating profit increased by 7%. Ono Pharma recorded sales of 50.1 billion won, up 23% last year thanks to the growth of the immuno-oncology drug Opdivo.
- Company
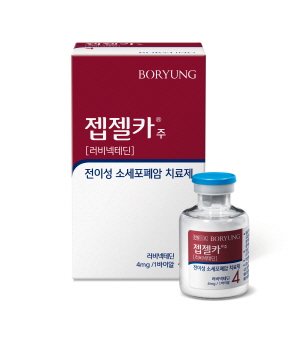
- Boryung’s new drug Zepzelca lands in Big 5 hospitals in KOR
- by Eo, Yun-Ho Jul 07, 2023 05:43am
- Zepzelca, a new drug introduced to Korea by Boryung, can now be prescribed in the Big 5 general hospitals in Korea. According to industry sources, the small cell lung cancer treatment Zepzelca (lurbinectedin) has passed the drug committees (DCs) of all the top 5 tertiary hospitals in Korea – Samsung Medical Center, Seoul National University Hospital, Seoul St. Mary’s Hospital, Seoul Asan Medical Center, and Sinchon Severance Hospital, and has been listed in 60% of all medical institutions nationwide that offer lung cancer treatment services. The only issue that remains is that Zepzelca is yet to be reimbursed. The company is preparing to submit an application for its reimbursement. The new anticancer drug was developed by Spanish pharmaceutical company PharmaMar S.A., and is indicate for the treatment of metastatic small-cell lung cancer that failed first-line platinum-based chemotherapy. Zepzelca is a novel drug with a mechanism of action that simultaneously ‘induces apoptosis by inhibiting DNA transcription,’ and ‘inhibits cancer cell proliferation, immune checkpoint activity, and angiogenesis through the inhibition of transcriptional activity in tumor-associated macrophages.’ The drug was approved by the Ministry of Food and Drug Safety in September last year and was released and prescribed in February this year. The drug was approved in July 2020 in the US. Zepzelca positioned itself as the leading second-line treatment for small-cell lung cancer in the US and posted sales of USD 5.35 million last year. Over 40% of small-cell lung cancer patients received Zepzelca as a second-line treatment. In Korea, Boryung owns the exclusive right to the sales and distribution of Zepzelca since 2017. Based on a study that became the basis of Zepzelca’s approval that was published in Lancet Oncology, patients treated with Zepzelca showed an overall response rate of 35%, with a mean duration of response of 5.3 months. Due to its convenience in administration of being administered once every 3 weeks and manageable side effects In addition to such clinical benefit, the drug has been evaluated to have a superior effect over other drugs that had been previously used in Korea. Zepzelca is also recommended in international guidelines including the the National Comprehensive Cancer Network and European Society for Medical Oncology.
- Company
- Release of triple-combo diabetes drugs imminent
- by Kim, Jin-Gu Jul 07, 2023 05:43am
- The release of the ‘triple combination therapies' appear to be in sight. However, unlike the 2-drug combos that are already in fierce competition even in the pre-release stage, industry interest in 3-drug combos is currently at best lukewarm. The pharmaceutical industry pointed to the relatively challenging development environment for triple combination drugs as well as the impurity issues that exist. Nevertheless, there are predictions that in the long term, the paradigm for antidiabetic combos will shift from dual therapy to triple therapy combinations. 96 companies own 100 2-drug combos vs. 2 companies own 7 3-drug combos According to industry sources on the 6th, Daewon Pharmaceutical and Hanmi Pharmaceutical recently applied for the reimbursement of their 'dapagliflozin, sitagliptin, and metformin’ triple combination therapy for diabetes. The drugs, Daewon Pharmaceutical's ‘Dapasita-M’ and Hanmi Pharm's ‘Sildapa M,' are expected to be released after September. This is because the patent for the original sitagliptin drug Januvia will expire on September 1st. Currently, the competition for antidiabetic combination drugs focuses on dual combinations. As of the 5th, 96 pharmaceutical companies have received marketing approval for 100 dual combination products that combine SGLT-2 inhibitors and DPP-4 inhibitors. This is in contrast to the fact that only 7 triple combination products from 2 companies have received marketing authorizations. In the case of dual combinations, the dapagliflozin and sitagliptin combination accounts for the absolute majority with 93 products from 92 companies. Many of these products are also expected to be released when the patent for Januvia expires. While the interest in dual combination therapies is highly heated despite the possibility that a large amount of the products will be released at the same time, the attention towards triple combination therapies is still lukewarm. Marketing approval state of SGLT2i + DPP4i combination therapy for diabetes Considering the expanded reimbursement scope for diabetes treatments that had been granted earlier this year, the phenomenon is somewhat puzzling. In May, the government limited the reimbursement scope for diabetes treatment to combinations of ▲SGLT-2 inhibitors, DPP-4 inhibitors, and Mmtformin, ▲SGLT-2 inhibitors, TZD, and metformin, ▲Some SGLT-2 inhibitors and sulfonylurea or in combination with insulin. The SGLT-2 inhibitor and DPP-4 inhibitor combination, which includes a majority of the dual combination therapies, was not included in the reimbursement scope. When prescribing to patients, doctors have to add metformin to the dual combination therapy drugs to receive reimbursement. "Difficult combine metformin due to its large dose… Impurity issues and concerns in development cost also exist" The analysis is that multiple factors have contributed to this phenomenon. The relatively complex product development is considered the primary reason among them. The dose of metformin, which is much larger compared to the other two drugs, posed an obstacle. The dose of dapagliflozin is set to 5mg and 10mg, while sitagliptin is set to 50mg and 100mg. However, the dose of metformin is set much higher at 500mg, 750mg, and 1000mg. Technically, combining the three ingredients is not difficult. However, due to the significant differences in dosages of each ingredient, the stability of the final product may be somewhat compromised. There are three main methods of combining the three ingredients: single-layered tablet, double-layered tablet, and coating Metformin with DPP-4 inhibitors and SGLT-2 inhibitors. Among these methods, dapagliflozin and sitagliptin can be combined relatively thinly in single- and double-layered tablets due to their small doses. As a result, there is a higher possibility that the two ingredients may not interact adequately. The method of coating metformin to the duo is not significantly different, but achieving a uniform thickness is difficult. This process poses certain challenges, such as the need for repeated bioequivalence tests to verify the uniform pharmacokinetic action of all ingredients. The impurity issue is also another factor that makes the development of triple combination therapy challenging. Among the three ingredients in the combination therapy, impurities have been detected in metformin and sitagliptin. As a result, when manufacturing pharmaceuticals with these ingredients, companies must validate whether or not impurities exist and submit one year’s worth of safety data to the Ministry of Food and Drug Safety. The so-called ‘1+3 joint bioequivalence’ system is also considered a factor that makes product development challenging. Under the Pharmaceutical Affairs Act that was implemented in 2021, the number of consignor pharmaceutical companies is limited to three per one consignee. This imposes a higher cost burden on small and medium-sized pharmaceutical companies in the development process compared to the past. An official from the pharmaceutical industry said, "Companies that started product development before the implementation of the regulation may be fine, but the potential burden for companies considering new development after that is substantial." They further explained, "In the past when 10 to 20 companies could share the cost, each company had a smaller burden. However, we can now only recruit up to four companies, which imposes a larger cost burden for each company." Another official stated, “The guideline set by the Ministry of Food and Drug Safety for the bioequivalence testing of combination therapies have become more stringent, requiring more extensive clinical trials than before. If the total cost for developing a combination therapy is around KRW 6 to 8 billion, each company should now bear approximately KRW 2 billion. This is not an easy decision for small and medium-sized pharmaceutical companies to make." "In the long term, triple combination therapies will increase… Numerous companies have already started development” However, the predominant forecast is that the number of companies venturing into the development of triple combination therapies will increase in the long term. This analysis is based on the fact that triple combination therapy is considered more advantageous than dual combination therapies in terms of convenience in taking the medicine and applicability for reimbursement. An industry official said, “While it is considered more challenging compared to dual combination therapies, the development and manufacturing of triple combination therapies is not inherently difficult. The market will move in the direction of reimbursement, to triple combination therapies.” Another industry official added, "As dual combination therapies are not eligible for reimbursement and require additional intake of metformin, the demand for triple combination therapies is expected to steadily increase in the future. Apart from Daewon Pharmaceutical and Hanmi Pharmaceutical, several other companies have already started or are considering the development of triple combination therapies."
- Policy
- Taiwanese new drug receives reimb in only 1 yr since release
- by Lee, Tak-Sun Jul 07, 2023 05:43am
- The Nephoxil Cap (ferric citrate hydrate) that was granted reimbursement at KRW 377 per capsule from the 1st of this month is actually a Taiwanese new drug. The drug, which is being imported and sold by the Japanese pharmaceutical company Kyowa Kirin’s Korean subsidiary in Korea, was developed by a Taiwanese pharmaceutical company. In other words, Nephoxil marks a rare case where a new drug developed in Taiwan was imported and reimbursed in Korea. Although the drug has not been listed in any of Korea’s A7 reference countries, it only took 14 months for the company to complete the listing process from approval to reimbursement, at a lower price than its substitute. In 2017, Kyowa Kirin Korea signed a domestic licensing agreement for Nephoxil with the Taiwanese pharmaceutical company, Panion & BF Biotech. Nephoxil was developed by Panion & BF Biotech in 2015. The agreement drew attention at the time as the Korean subsidiary of Kyowa Kirin had independently promoted and signed the agreement, not its Japanese headquarters. Nephoxil is used to improve hyperphosphatemia in patients with chronic renal disease on hemodialysis. As an iron-based phosphate binder, the drug has been assessed to reduce the risk of adverse events that commonly arise in calcium-based phosphate binders such as hypercalcemia and vascular calcification. Non-calcium class drugs currently available in Korea are Sanofi’s Renvela Tab, SK Chemical’s Invela, JW Pharmaceutical’s Fosrenol, among others. Also, same-ingredient generics versions of Renvela have recently joined in on the competition in Korea’s market. In Korea, Kyowa Kirin Korea has been positioning itself as a company that sells treatments for chronic renal disease patients. The company had achieved high sales performance n the field with its anemia treatment 'Nesp' and 'Regpara', a treatment for secondary hyperparathyroidism in patients with chronic renal disease. The company had once excelled in the hyperphosphatemia treatment market as well. Its product, Renagel Tab, which contains the same ingredient as Lenvela, has once led the market, however, its supply was discontinued in 2015 due to a contract with its developer. The company had lacked a product for hyperphosphatemia ever since. In this context, Nephoxil was a relief to the company. Regarding the use of Nepoxil, the Korean Society of Nephrology recommended restricting the administration of calcium-based phosphorus binders to avoid hypercalcemia and favorably recommended ferric citrate as it is useful and has an additional effect on correcting anemia as it contains iron compared to general phosphorus binders. However, the Health Insurance Review and Assessment Service’s Drug Reimbursement Evaluation Committee reviewed that it is difficult to determine whether Nephoxil has a different effect over existing non-calcium-based binders. Moreover, none of the A7 countries (USA, Germany, Switzerland, UK, Italy, Japan, France) have listed the same product. Only different strengths of ferric citrate were available in the United States and Japan. Despite such criticism, the company overcame the barriers with its low price. Kyowa Kirin Korea accepted the drug’s price of KRW 377, which is 90% of the weighted average price of its alteratives, and was able to skip the drug price negotiation process. Nephoxil received approval from the Ministry of Food and Drug Safety on May 9 last year. After passing DREC review in only one year of its approval in April this year, it was swiftly applied reimbursement in July. The industry analysis is that the company’s low price strategy also had some influence on Nephoxil’s speedy reimbursement.
- Company
- Baxter and Fresenius Medical benefited the most
- by Nho, Byung Chul Jul 07, 2023 05:43am
- As the Ministry of Health and Welfare's pilot project for home management of peritoneal dialysis patients began in earnest, the sales of Baxter and Fresenius Medical, which supply related products, are also expected to grow exponentially. As of 2022, total domestic hemodialysis patient medical expenses amounted to 2,634 billion won, of which peritoneal dialysis accounted for 4-5%. According to the hemodialysis adequacy evaluation data in 2018, the number of hemodialysis patients in that year was 90,901, and it is showing an increasing trend of 10,000 each year, which is difficult to find worldwide. The annual cost of hemodialysis per patient who visits the hospital's artificial kidney room for treatment is about 30 million won, and peritoneal dialysis, which can be treated at home, is observed to be 20-30% cheaper. Therefore, the health authorities plan to reduce the proportion of hemodialysis, which costs astronomical costs, and induce peritoneal dialysis to induce financial soundness, considering the health insurance financial deficit and reduction in reserves. According to what is known, health authorities are planning various policies/systems to raise the rate of peritoneal dialysis from less than 5% to a maximum of 10-20% through this pilot project. The health insurance benefit subsidy for cassettes, hemo-vacs, and catheter tip occluders, which are consumables required when using an automatic peritoneal dialysis machine, is 14.2 million won per day. Previously, the subsidy (5,640 won per day) was not enough to purchase only a cassette, but the burden of patients was reduced by expanding the benefits for Hemo-vac. Automated peritoneal dialysis is when a patient connects an automatic peritoneal dialysis machine, dialysis solution, and body catheter before going to bed, and dialysis is automatically performed while sleeping. For this reason, while there are few restrictions on work, school life, and social activities, there is a risk of accidents such as secondary infection as the patient handles all processes directly. This is a part that can be sufficiently prevented with proper education. Hemodialysis requires direct visits to the artificial kidney room three times a week for dialysis for 3 to 4 hours a day, and emergency response can be swift. Still, it has the disadvantage of being restricted in daily life. The pilot project for home management of peritoneal dialysis patients was adopted by order of the Ministry of Health and Welfare in December 2019, and the second pilot project (May 2022-2025) is currently underway. The purpose of the project is to continuously manage at-home patients and provide feedback to reduce unnecessary medical expenses due to hospitalization and worsening of diseases and to improve the quality of life of patients. The target is a chronic kidney disease stage 5 patient who needs renal replacement therapy and has agreed to participate in the pilot project for home management of peritoneal dialysis patients.
- Policy
- Evaluation different after Kymriah·Zolgensma benefits?
- by Lee, Tak-Sun Jul 07, 2023 05:43am
- The ultra-expensive treatments Zolgensma and Kymriah are supposed to go through a performance evaluation, but whether or not they are disclosed is different. As a pre-approved drug, Zolgensma, which is subject to review by an expert review committee, has performance evaluation results disclosed to the public, whereas Kymriah does not. Therefore, unlike Zolgensma, Kymriah, which received a benefit earlier than Zolgensma, does not disclose performance evaluation results. According to the industry on the 5th, The HIRA recently disclosed the first performance evaluation of Zolgensma on its website. Zolgensma requires clinical evaluation before administration and every 6 months after administration for up to 5 years, and objective data such as medical records for clinical evaluation must be submitted. In addition, ▲ permanent respiratory use or death, ▲ CHOP-INTEND score not improved by 4 points or more compared to the baseline before drug administration, ▲ even if the previous items were improved, CHOP-INTEND 4 points or more in two consecutive times in the subsequent response evaluation Or, if it falls under any of the cases of a decrease of 3 points or more on the HFMSE, it is defined as drug administration failure. Reflecting this, as a result of the first performance evaluation, clinically meaningful improvement was confirmed in 5 out of 6 cases and marked as successful. The remaining case was judged to be a failure because a patient with respiratory problems due to SMA died of suspected acute respiratory failure. 5 out of 6 were successful reviews. Then, how was Kymriah, which was listed for benefit in April last year, 4 months ahead of Zolgensma, evaluated? Zolgensma is an ultra-expensive new drug worth 2 billion won and Kymriah is about 360 million won, and the Ministry of Health and Welfare is managing the performance of both. However, Kymriah cannot know the results of the evaluation. Because there are no disclosure rules. An official from the HIRA said, "Zolgensma is a pre-approved drug that goes through an expert review committee, so the review results are disclosed according to regulations, but Kymriah has no disclosure regulations." “At this time, we are not considering making it public,” he explained. Kymriah was not subject to the prior approval system because the patient's condition could deteriorate due to medication delay. For this reason, performance evaluations are not made public. Regarding this, an industry insider pointed out, "It is appropriate to disclose the results of the performance evaluation to the outside in order to enhance transparency and reliability in the context of the decision to evaluate the performance as part of the management of super-expensive drugs." The HIRA went through a professional review committee and disclosed two cases of the recognition of Kymriah's benefits in May, but both cases were rejected because they did not meet the standards. If the reimbursement is rejected, the patient has no choice but to pay 360 million won for non-reimbursement drugs. If benefits are applied, the drug price will be reduced to 6 million won. For this reason, some are suggesting that a plan to reduce the burden on patients should be prepared in the event of a post-reimbursement issue by reflecting the characteristics of an ultra-expensive new drug. Regarding this, Novartis said, "The reduction in benefit is a problem that occurs between the nursing institution and the patient and has nothing to do with the manufacturer. There is no separate patient support program."
- Policy
- Pres. Yoon urges swift legislation for remote treatment
- by Kang, Shin-Kook Jul 06, 2023 05:39am
- President Yoon Suk-yeol has instructed the Ministry of Health and Welfare to make every effort to pass the amendment of the Medical Service Act for the introduction of non-face-to-face treatment, which is currently under discussion in the National Assembly, raising hopes for its rapid legislation. President Yoon made these remarks on the 4th while leading the 18th Emergency Meeting on Economic Affairs on the direction of economic policies for the second half of 2023 at the Yeongbingwan in Cheong Wa Dae. President Yoon stated, "Many bills aimed at improving the economic constitution and ensuring stable public welfare - such as the National Finance Act for the introduction of fiscal rules, the Housing Act for easing residency obligations, and the Medical Service Act for establishing the basis for non-face-to-face treatments - are being impeded by the National Assembly, disappointing many citizens." To this, President Yoon urged, "Ministers of each department should focus solely on the people and make every effort to ensure the swift passage of essential economic and public welfare bills." As President Yoon personally directed the amendment of the Medical Service Act, it is anticipated that the government will expedite the legislation for the non-face-to-face treatment system. Currently, the amendment of the Medical Service Act related to non-face-to-face treatment is pending in the Legislative Review Subcommittee of the NA’s Health and Welfare Committee. The direction of the legislation has taken shape to closely align with the current pilot project for non-face-to-face treatment. The legislative direction being discussed and promoted by the government in cooperation with the National Assembly is as follows: Allowing non-face-to-face treatment only for follow-up visits, with initial consultations primarily in clinic-level medical institutions as exceptions. If patients are not eligible for home-delivered medication, the patient (or their representative) may obtain the prescribed medication directly from a pharmacy after receiving face-to-face medication counseling from a pharmacist. While the method of delivering medication is still an issue, the matter will not be a major point of contention during the National Assembly discussions, as the aspect falls under the amendment of the Pharmaceutical Affairs Act and not the Medical Service Act.