- LOGIN
- MemberShip
- 2026-05-03 21:03:15
- Policy
- "Chickenpox vaccine 'Sky Varicella Inj' is safe…"
- by Lee, Jeong-Hwan Jun 13, 2024 05:48am
- SK Chemical’s varicella virus vaccine, Sky Varicella Inj. The Korea Disease Control and Prevention Agency (KDCA) reported on June 12th that experts and related agencies have conducted an investigation and analysis in response to an increased number of adverse reactions reported following vaccination with 'Sky Varicella Inj,' a varicella virus vaccine, and they confirmed that there are no safety concerns related to the vaccine. According to the KDCA, cases of shingles have been recently reported following vaccination with Sky Varicella Inj. From 2018 until May this year, 1,888,631 varicella virus vaccinations were given, and 29 cases of shingles were reported after the vaccination (reported rate: 0.0015%). The reported rate of shingles after vaccination with SK Chemical’s varicella virus vaccine, Sky Varicella Inj, was 0.003%. Consequently, the KDCA formed a public-private working group on April 26th following the decision by the Korea Expert Committee on Immunization Practices (KECIP). The group conducted a comprehensive review, including the safety of the varicella virus vaccine and shingles cases after vaccination, and concluded that there are no safety concerns related to Sky Varicella Inj. The public-private working group consisted of three pediatric infection experts, one virus experts, pharmacoepidemiology expert, and officials from the National Health Insurance Service (NHIS), KDCA, and the Ministry of Food and Drug Safety (MFDS). The MFDS stated it had conducted a comprehensive evaluation of documents related to quality and non-clinical·clinical trials submitted during the approval of the varicella virus vaccine, reports of national lot release at every manufacturing stage, and cases of adverse reactions reported in South Korea and oversees. The findings indicated no safety concerns related to the vaccine itself. After investigating 29 cases of reported shingles following varicella vaccination, it was found that all 29 individuals experienced symptom improvement without any complications. Additionally, analysis of NHIS big data showed no significant differences in severity, including hospitalization duration after shingles occurrence, following vaccination. The KDCA explained, "The varicella vaccine is a live vaccine that uses weakened strains of bacteria or viruses. It is known that the symptoms of shingles after vaccination are generally milder than when shingles occur in individuals who have not been vaccinated against chickenpox." During the investigation, there had been one case of reported death suspected to be related to the varicella vaccine. However, the expert committee, including a blood cancer specialist, concluded that there is no causal relationship between the varicella vaccine and the reported death. Consequently, based on these results, the KECIP decided to continue using Sky Varicella Inj in national immunization. However, considering that the incidence of shingles after vaccination with Sky Varicella Inj is higher than with other vaccines, precautions will be advised for high-risk groups, such as prohibiting the administration of the vaccine to severe immune-compromised patients and pregnant women. The KDCA strongly advocated for vaccination, stating the significant preventive effect of the varicella vaccine, citing that the incidence of chickenpox among the unvaccinated group, based on those born in 2022, is nearly ten times higher than that of the vaccinated group. They also emphasized that Sky Varicella Inj’s preventative effect against smallpox is 78.9%, which is higher than that of other varicella vaccines. The KCDC said, "We urged the medical community to actively report cases of adverse events, such as shingles, after receiving the varicella vaccine." They added, "Enhanced surveillance of the safety of the varicella vaccine will be implemented, including conducting additional diagnostic tests when reporting adverse events." If any adverse reactions, such as high fever, rash, and shingles, occur after the vaccination in young children, report to the NIP internet website (https://nip.kdca.go.kr) or the monitoring system for vaccines (https://is.kdca.go.kr). For other inquiries, including the report process, contact the call center ☎1339 or the nearest public health center.
- Policy
- CPAC ‘Scemblix’s orphan drug designation is valid’
- by Lee, Hye-Kyung Jun 13, 2024 05:48am
- Pic of Scemblix The next-generation chronic myeloid leukemia drug ‘Scemblix (asciminib)’ is expected to be available for adult patients with chronic myeloid leukemia (CML) with the T315I mutation or Philadelphia chromosome-positive acute lymphocytic leukemia (Ph+ ALL) with the T315I mutation. According to the minutes of the Central Pharmaceutical Affairs Council that were disclosed by the Ministry of Food and Drug Safety on the 11th, the CPAC had discussed Scemblix’s orphan drug designation agenda at its last meeting. In Korea, Scemblix is currently only approved as a treatment for adult patients with Philadelphia chromosome-positive chronic myeloid leukemia (Ph+ CML) in the chronic phase previously treated with two or more tyrosine kinase inhibitors (TKIs). Iclusig(ponatinib) is currently the only treatment option available for the "patients with T315I-positive CML," for which the CPAC has been discussing Scemblix’s orphan drug designation. Iclusig was designated as an orphan drug for “patients with T315I-positive CML” and “adult patients with chronic, accelerated, or acute phase chronic myeloid leukemia (CML) or Philadelphia chromosome-positive acute lymphocytic leukemia (Ph+ ALL) that is resistant or intolerant to other tyrosine kinase inhibitors (TKIs). Regarding the designation decision, a CPAC member stated, "Scemblixworks in patients who are not sufficiently responding to treatment with other alternatives and in patients for whom alternative medicines are not available. Therefore, it is the only available alternative that offers improvement for difficult-to-treat patients.” According to data submitted by Novartis, Scemblix is a valid and viable alternative treatment option for CML patients with the T315I mutation, regardless of their Iclusig use. Also, the reported adverse events were manageable with dose adjustment, discontinuation, combination medications or supportive care, and a favorable safety profile compared to alternatives. The CPAC member said, "When considering the number of patients, prevalence, and safety and efficacy assessments, the results justify the drug’s orphan drug designation.” Another CPAC member said, “Given that the indication is limited to chronic myeloid leukemia and the submitted study is a Phase I study, its efficacy cannot be directly compared with Iclusig. However, in the submitted Phase I study, 38.5% of patients who have been previously treated with Iclusig achieved major molecular response (MMR). Given that Iclusig is the only treatment option for patients with T315I-mutant Ph+ CML, we believe that an orphan drug designation can provide patients and their physicians with more options.” Some noted that the definition of “significant” in the orphan drug designation criteria typically implies a statistically significant difference and that it would be unreasonable to conclude that a drug has significantly improved safety or efficacy based on the results of a Phase I trial. One member noted, "Given the limited number of CML patients with the T315I mutation, it will be some time before a direct comparison study is published.” However, the majority of committee members agreed that Scemblix is a viable treatment option for patients with leukemia that has become resistant to other therapies and that its orphan drug designation is valid.
- Company
- A growing trend of SC injections heats up competition
- by Son, Hyung-Min Jun 13, 2024 05:48am
- Pharmaceutical and biotech companies in Korea and worldwide focus on developing formulation modifications for anticancer agents. Following 'Tecentriq (atezolizumab)' SC (subcutaneous injection obtaining marketing authorization from the European Medicines Agency (EMA) in January, the R&D of 'Opdivo (nivolumab)' and 'Rybrevant (amivantamab)' is nearing the end. The industry attributes the recent booming development of SC formulations to their advantages over IV (intravenous) formulations, such as shortened administration time, improved convenience of administration, and reduced injection-related side-effects. According to the industry sources on June 11th, Bristol Myers Squibb (BMS)·ONO Pharmaceutical and Janssen disclosed the research outcomes of their SC formulations products, Opdivo and Rybrevant, respectively. Opdivo, an immunotherapy for cancerOpdivo, developed by BMS and ONO Pharmaceutical, is a PD-1-targeting immunotherapy for cancer. BMS conducted a clinical trial involving patients with renal cell carcinoma to change the Opdivo IV formulation to an SC formulation, and they obtained successful outcomes. The Phase 3 CheckMate-67T trial enrolled 495 patients with advanced or metastatic clear cell renal cell carcinoma (ccRCC) who have received prior therapy. For safety profile, the percentage of patients with topical adverse reactions of all grades in the Opdivo SC group was 8.1%, and in the IV group, it was 2.0%. Among the patients who were anti-drug antibodies (ADA)-positive, 15.2% of the patients in the SC group experienced mild topical adverse reactions of Grade 1-2, which resolved without the need of treatment. SC formulation of Rybrevant, a targeted therapy for cancer, has also shown effects in a clinical trial. Rybrevant, developed by Janssen, is a treatment for patients with non-small cell lung cancer (NSCLC) with EGFR exon 20 insertion mutations. A recently disclosed Phase 3 PALOMA-3 study demonstrated the non-inferiority of SC formulation Leclaza plus Rybrevant therapy to IV formulation Leclaza plus Rybrevant therapy. At a median follow-up of 7 months, SC formulation of Leclaza plus Rybrevant therapy was non-inferior to IV formulation Leclaza plus Rybrevant therapy. Yuhan SC formulation of Leclaza plus Rybrevant therapy had an ORR of 30.1% compared to 32.5% in IV formulation Leclaza plus Rybrevant therapy, meeting the standard for non-inferiority. For injection-related reactions (IRR), SC formulation of Leclaza plus Rybrevant therapy showed 13% IRR, which was significantly lower than 66% in IV formulation Leclaza plus Rybrevant therapy. The analysis suggests that improving Rybrevant’s administration will lead to greater synergy when combined with Leclaza. One of the concerns about combining oral Leclaza with IV formulation Rybrevant is that it may be less convenient due to the increased number of hospital visits. Since oral formulations for targeted therapy for lung cancer, such as Tagrisso (osimertinib) and Giotrif (afatinib), have been approved, Rybrevenat’s injectable formulation poses a weakness. Therefore, whether SC formulation of Rybrevant would be commercialized is attracting attention. Latecomers have started developing SC formulations Latecomers to developing anticancer agents are working to change formulations to reduce the administration time. Roche has succeeded in developing SC formulation of Tecentriq, an immunotherapy for cancer, and MSD is conducting a phase 3 clinical trial of SC formulation of Keytruda. Alteogen, which has a SC formulation modification technology, plans to develop technology for ADC SC platform. Alteogen expects the SC formulation of ADC to reduce adverse reactions. The company aims to launch the SC formulation of ADC into the market by 2028. The Korean pharmaceutical biotech industry is working on developing potential SC formulations of anticancer candidates. GI Innovation is developing a SC formulation of GI-102, a candidate immunotherapy for cancer. According to GI Innovation, the SC formulation of GI-102 has a bioavailability (BA) of up to 60% compared to an IV formulation. A clinical trial for the SC formulation of GI-102 will be conducted by confirming an appropriate dose in patients with various solid cancers. Once a proper dose of the SC formulation of GI-102 is determined, GI Innovation plans to conduct a clinical trial for an incremental dose in patients with solid cancer who have failed systemic therapies. Additionally, several companies are working on a new formulation modification other than IV to SC. Daehwa Pharmaceutical is developing an oral paclitaxel formulation, Liporaxel Sol. In a phase 3 clinical trial conducted by Daehwa Pharmaceutical’s partnering company in China, Haihe Biopharma, the efficacy and safety of Liporaxel have been confirmed to be non-inferior to paclitaxel injection.
- Policy
- 9th meeting held for external reference pricing reevals
- by Lee, Tak-Sun Jun 13, 2024 05:48am
- The government and the pharmaceutical industry held the 9th meeting on external reference pricing reevaluations but reportedly decided to continue discussions. Initially, the 9th meeting was supposed to be the last in the opinion-gathering process, but further meetings were deemed inevitable. According to industry sources, the government and the pharmaceutical industry held the 9th round of talks on the external reference pricing reevaluations at the Kukje Electronic Center in Seocho-gu on the 12th. This is the 9th round of talks since it began in November last year. As the government’s proposal for the method of comparison came out at the 8th meeting, the 9th meeting was expected to be the time to refine the final draft based on industry opinions. The industry also needed time to review the proposal, which was why the 9th meeting was pushed back to June instead of May after the 8th was held at the end of April. At the 9th meeting, the pharmaceutical industry made various demands. Although there was disagreement on the government’s method of comparing the A8 average price, which excludes the highest and lowest prices, the method is expected to be maintained as is. However, the parties reached a consensus that further discussion is needed on which drugs should be excluded from revaluations, the method of searching for foreign drug prices, and on whether to put a lower limit on the rate of drug price cuts. The 10th meeting is expected to be held after July to discuss the specifics. An industry official who attended the meeting said, "The industry made a lot of suggestions and decided to continue on the discussions. However, there seems to be no room for change in the comparison method proposed by the government."
- Company
- ‘Verify safety when using botulinum toxin for hair loss'
- by Nho, Byung Chul Jun 12, 2024 05:45am
- Dr. Jae-Hong Kim, Director of Planning and Policy at the Association of Korean Dermatologists (Chief Director, Yonsei Joeun Dermatology Clinic Gwangmyeong Branch)The market for hair loss treatment is growing day by day as hair loss, once considered a typical condition of middle-aged men, has become a general condition across all genders and ages. In particular, the market is being segmented across a wide age range and various lifestyles, and new treatments that complement the limitations of existing treatments are being actively developed. Dr. Jae-Hong Kim, Director of Planning and Policy at the Association of Korean Dermatologists, said, "Androgenetic alopecia (AGA), the most common type of hair loss, is generally treated with oral medications, but if the patient has inadequate drug response, the treatment’s effect decreases after a certain period of time. In recent years, procedures with different mechanisms of action, such as botulinum toxin, have emerged as a new alternative to treat hair loss." Botulinum toxin is a neurotoxin that inhibits the release of acetylcholine, a neurotransmitter that prevents muscles from contracting. It causes a temporary relaxation and shrinkage response in the muscle and is commonly used to treat wrinkles such as crow's feet and frown lines or to shrink overdeveloped muscles such as trapezius and calves. Kin explained, "When injected into the dermis, botulinum toxin has been shown to reduce the activity of TGF-ß1, which is responsible for hair loss. It is known to improve hair loss by increasing blood circulation by relaxing of the muscles around the scalp when injected intramuscularly." Research and publications on the effectiveness of botulinum toxin in treating hair loss are actively being conducted and published in the field. "There was a case of a man in his 30s and 40s who had advanced hair loss with thinning hair in the crown area along with scalp heat. He did not see any significant effect from oral medications, but experienced symptom improvement after receiving botulinum toxin injections in the balding areas.” However, as hair loss can have a significant impact on a patient's social and interpersonal life, it is important to carefully check the safety of the administered products. The safety and product history can be checked through the product’s FDA approval status and proven titer in the global market. In Korea’s botulinum toxin market, products such as Botulax have been approved by the FDA and have entered big markets such as Europe and China, and have been recognized for both its efficacy and stability. Accurate diagnosis and proper treatment by a medical professional are also important to achieve the best results. He added, "Patients tend to rely on arbitrary treatments or folk remedies, fearing side effects of oral medications or painful injections, which can cause them to miss the right timing to receive treatment. As various treatment methods are now available, patients should consult with a medical team to develop a treatment plan that takes into account each patient’s individual characteristics and the mechanism of action of the drug."
- Company
- Autotelic Bio signs licensing agreement with Chinoin
- by Nho, Byung Chul Jun 12, 2024 05:45am
- (From the left) Fernando Torres Navarrete, BD Director at Chinoin Productos Farmaceuticos in Mexico , Tae-Hun Kim, CEO of Autotelic Bio Autotelic Bio announced on the 7th that it has signed an exclusive license and supply agreement with Chinoin Productos Farmaceuticos in Mexico to distribute ATB-101, a novel combination drug for the treatment of hypertension and diabetes. ATB-101 is a fixed-dose combination product comprising of the hypertension drug ‘olmesartan’ and the oral diabetes drug ‘dapagliflozin.’ It is the world's first combination drug that treats both hypertension and Type 2 diabetes, making it easier for patients with both chronic diseases to take their medication. The company has received Phase III IND approval from the Ministry of Food and Drug Safety for ATB-101 and is currently conducting Phase III clinical trials in patients with essential hypertension and type 2 diabetes at more than 35 major hospitals in Korea, including Seoul National University Bundang Hospital. Autotelic Bio is planning to launch the product globally after proving safety and efficacy through the ongoing Phase 3 clinical trial. For this, the company has registered composition patents in the U.S., Japan, Russia, Mexico, and Brazil, in addition to Korea, and is expanding its patent to other countries such as China. The exclusive license and supply agreement it signed in Mexico is to supply more than 30 million ATB-101 tablets over 5 years. The agreement demonstrates the company's potential to expand into neighboring Latin American countries through Chinosa and is expected to serve as a bridgehead for future global expansion. In addition to the upfront payment, Autotelic Bio will receive additional payments based on development, licensing, and commercialization milestones. Mexico's hypertension and diabetes market is the second largest in Latin America after Brazil and has significant potential. Autotelic Bio plans to grow sales in the Mexican market and reinvest the proceeds in the continued development of innovative new medicines. Chinoin Productos Farmaceuticos is a Mexican pharmaceutical company founded in 1924. It owns a pharmaceutical R&D, manufacturing, licensing, sales, and marketing division, and is regarded to have excellent sales and marketing capabilities, ranking among the top 10 pharmaceutical sellers in Mexico. Autotelic Bio recently completed a pre-IND meeting with the U.S. Food and Drug Administration (FDA) to advance ATB-101 into the United States. During the meeting, the company received a positive response from the FDA regarding the ongoing Phase III clinical trial, and that an additional local Phase I clinical trial will be sufficient for approval in the U.S. based on the results of the domestic Phase III trial. Based on the results of the pre-IND meeting, the company will be meeting with more than 10 pharmaceutical companies at Bio USA to discuss global rights agreements for ATB-101, including in the US. This year, Autotelic Bio has joined the Boston C&D Incubation Office, a blockbuster global expansion program organized by the Korea Health Industry Development Institute (KHIDI), to strengthen its network for ATB-101’s clinical development and licensing-out activities and create results in the U.S. market. In addition to the incrementally modified drug, Autotelic Bio is developing two other RNA-based anti-cancer drugs, ATB-320 (a dual-mechanism of action anti-cancer RNA drug that works on the TME and inhibits angiogenesis) and ATB-350 (a next-generation KRAS mutation-targeting anti-cancer RNA drug that targets specific tissue). Also, its ATB-610 (ALK5 inhibitor), an inhaler in the company’s anti-fibrosis drug pipeline, has been selected as a project of the National New Drug Development Project in Korea, adding momentum to the company’s development of new drugs.
- Company
- Failed reimb negotiations for Lorviqua, was it for the best?
- by Eo, Yun-Ho Jun 12, 2024 05:45am
- After a long wait, the result was still a ‘no go.’ A solution does exist, but hesitation seems to be holding them back. The insurance reimbursement expansion for the 3rd-generation ALK anticancer drug Lorviqua to first-line therapy has become unclear again. Negotiations between Pfizer Korea and the National Health Insurance Service on the drug price of the ALK-positive NSCLC treatment Lorviqua (lorlatinib), which passed the Health Insurance Review and Assessment Service’s Drug Reimbursement Evaluation Committee review in January and began in March, recently broke down. This is the first time negotiations have broken down for a drug seeking reimbursement expansion risk-sharing agreement (RSA) scheme. The reason for the breakdown is believed to be related to the ‘expenditure cap amount’ rather than 'drug price'. Lorviqua was granted pharmacoeconomic evaluation exemptions when it was first listed. Such PE exemption drugs are required to be reimbursed through the RSA Expenditure Cap Type scheme. As such, a new cap amount would have been derived to account for the increased usage due to the expanded reimbursement during negotiations, and it is likely that Pfizer was unable to accept it. Pfizer's unacceptance may be seen as greed on the pharmaceutical company’s part. However, negotiations are always conducted within a set framework. Pfizer did conduct a pharmacoeconomic evaluation as part of the reimbursement expansion process. So the solution would be to eliminate the disputed expenditure cap requirement and convert Lorviqua to a drug listed through the general process. The other ALK anticancer drugs available in the market - the 1st generation drug ‘Xalkori (crizotinib),’ 2nd generation drug ‘Alecensa (alectinib),’ ‘Zykadia (ceritinib)’ – were all listed through the general track. In fact, Pfizer offered to switch Lorviqua’s reimbursement path to general listing during negotiations, but the government turned it down as it was "unprecedented," and that hesitation led to the breakdown of negotiations. However, patients are left to suffer the damage. It's important to make things work. If necessary, there's no reason not to take the road less traveled. Moving RSA drugs to the general track will also ensure additional price transparency. Pfizer quickly announced plans to reapply for reimbursement expansions. A company spokesperson said: "We are disappointed that final negotiations were unsuccessful. We plan to reapply for first-line reimbursement as soon as possible to ensure patient access to the treatment and we will do our best to engage in effective discussions with the government and facilitate a forward-looking review.” As such, its progress upon reapplication will also be interesting to watch. This was the e first time RSA negotiations have failed. After the unprecedented event, starting the process all over again would be a lengthy process. Regardless of whether reimbursement is expanded or not, the government would need to be flexible in its administration to achieve a quick result. Lorviqua was specifically designed and developed by Pfizer to penetrate the blood-brain barrier (BBB). The drug’s high clinical value as a first-line treatment was recognized in the 5-year long-term follow-up results of the CROWN study that was presented at ASCO. Results showed that Lorviqua reduced the risk of disease progression or death by 81% compared to crizotinib, with 60% of patients surviving without disease progression at 5 years. The risk of brain metastasis progression was reduced in 94% of patients, with only 4 of 114 Lorviqua-treated patients without brain metastases developing brain metastases.
- Policy
- Price ceiling for 'atosiban' set to rise under agreements
- by Lee, Tak-Sun Jun 12, 2024 05:45am
- Hanlim Pharm’s The insurance drug price ceiling for atosiban injection, used to delay pre-term birth in pregnant adult women, will increase. Currently, three products of atosiban for injection are available. With the drug price ceiling adjustment, better supply is expected following negotiations related to expanding the volume of distribution. According to the industry on June 11, the drug price ceiling of three products containing atosiban acetate will rise. Three items include Ferring Korea’s 'Tractocile Inj,' Hanlim Pharm’s 'Trecsiban Inj,' and Dong Kook’s 'Asiban Inj.' These products are used to delay pre-term birth in pregnant adult women with ▲regular uterine contractions of at least 30 seconds duration at a rate of more than 4 per 30 minutes ▲a cervical dilation of 1 to 3 cm (0-3 for nulliparas) and effacement of greater than 50% ▲18 years and older ▲pregnancy 24-33 weeks, and ▲a normal fetal heart rate. It is an inhibitor of oxytocin and selectively acts on uterine muscle, potentially preventing uterine contractions. The drug is currently reimbursed when used as the second-line treatment following the use of a ritodrine-containing agent. It is not covered with reimbursement from week 3 and results in a burden of over KRW 500,000 per 1 cycle. Therefore, the medical community has been advocating for expanding reimbursement coverage for first-line treatment and making it reimbursable after week 3. Current adjustment negotiations have reached an agreement on an increased drug price ceiling based on the volume of contract manufacturing (imports). It appears that this measure is intended to stabilize the supply. The drug price ceiling for a 6.75 mg product will be increased from KRW 13,000-14,000 to KRW 15,000, and for a 37.5 mg product, it will be increased from KRW 43,000 to 47,000. As the government focuses on policies related to raising birth rates and supporting pregnant women, raising the drug price of pre-term birth treatment likely happened quickly. Starting this month, five products for morning sickness are also reimbursable.
- Company
- Boryung wins the Pomalyst patent challenge for the 2nd time
- by Kim, Jin-Gu Jun 11, 2024 03:25pm
- Boryung has once again challenged the Pomalyst patent and won. Boryung won the second attempt to avoid the substance patent of ‘Pomalyst (pomalidomide),‘ a treatment for multiple myeloma. Despite winning the infringement trial for the same patent in 2021, Boryung had not released generic versions. It seems that Boryung changed the method of generic development and rechallenged the patent. The analysis suggests that Boryung is on a countdown to releasing Pomalyst generic following the second-time success of the patent infringement challenge. It has been confirmed that Boryung has already applied for marketing approval for four doses of pomalidomide. According to pharmaceutical industry sources on June 10th, Boryung received the decision in its favor regarding the claims to confirm the scope of a right for the Pomalyst substance patent. Interestingly, Boryung has already won the previous challenge for the same patent. In July 2020, Boyung filed claims to confirm the scope of a right for the Pomalyst substance patent and won the claim in February. At that time, Kwang Dong Pharmaceutical also challenged the patent and won. However, Kwang Dong Pharmaceutical and Boryung have not released the generic version. Although the patent holder did not appeal the loss of the first trial, neither company released the generics. In three years, Boryung filed a claim with the Intellectual Property Trial and Appeal Board (IPTAB) again. The target for claiming a trial and the type of claim were the same as before. Regarding this, the pharmaceutical industry suggested that both companies attempted to develop Pomalyst generics using a method approved by the IPTAB but faced challenges. Boryung might have developed a generic using a different method. Developing a generic with a new method may have required a new trial decision to confirm whether it does not fall under the scope of the rights of the Pomalyst patent. Consequently, the company may have rechallenged the same patent and won. It has been confirmed that Boryung has already applied for marketing approval for its four doses of generics. The pharmaceutical industry anticipates that Boryung will secure a right to priority of sale for Pomalyst generic exclusively. Celgene’s Pomalyst was approved in 2014 for the treatment of multiple myeloma. According to a pharmaceutical market research firm IQVIA, Pomalyst’s sales reached KRW 22.8 billion last year, up 17% from KRW 19.5 billion in 2022.
- Product
- Selection dilemma rises in IBD mkt due to increased options
- by Moon, sung-ho Jun 11, 2024 05:48am
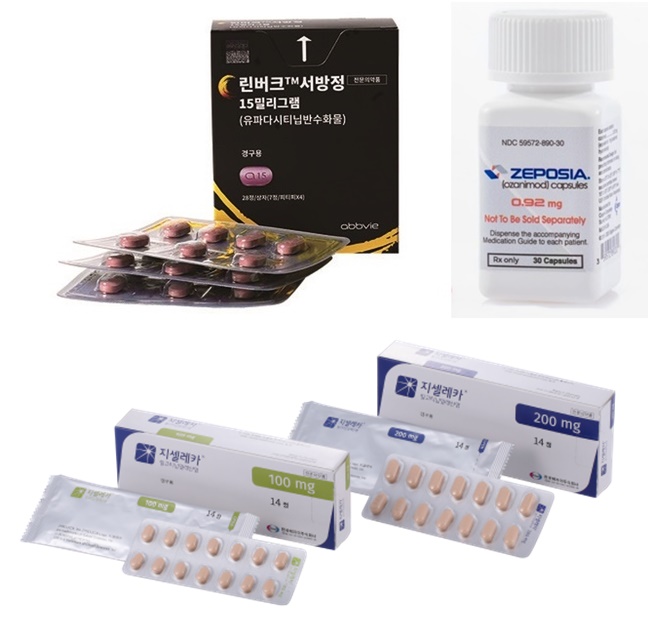
- With the recent surge in treatment options for inflammatory bowel disease (IBD), which is represented by ulcerative colitis and Crohn's disease, developing an appropriate treatment strategy for IBD is emerging as a rising topic in clinical practice. This is due to the recent health insurance reimbursement extensions granted for treatments by multinational pharmaceutical companies, which have lowered the burden on site. #Amid intensifying sales and marketing competition within the industry, the medical community is expected to revise its guidelines on selecting appropriate treatments. Until now, tumor necrosis factor (TNF) blockers Humira (adalimumab) and Remicade (infliximab) have dominated the field of IBD treatment in Korea. According to the pharmaceutical industry and medical community on the 8th, the IBD treatment market has been rapidly reshaping with the competitive entry of global pharmaceutical companies’ treatments this year. First, in the first half of this year, Lilly Korea received approval for its interleukin-23 (IL-23) inhibitor ‘Omvo (mirikizumab) from the Ministry of Food and Drug Safety. This added another IL inhibitor option to ‘Stelara (ustekinumab),’ the only anti-interleukin drug that had been available in the market until then. As a result, the anti-integrin agent ‘Kynteles (vedolizumab, Takeda),’ and anti-interleukin agent ‘Stelara,’ ‘Omvo,’ and the Janus kinase (JAK) inhibitors ‘Xeljanz (tofacitinib, Pfizer),’ ‘Rinvoq (upadacitinib, AbbVie),’ ‘Jyseleca (filgotinib, Eisai) can now be prescribed for IBD in Korea. Also, in addition to the JAK inhibitors, which were the only oral treatment options for severe IBD until the first half of this year, the launch and reimbursement approval of ‘Zeposia (ozanimod, BMS),’ a sphingosine-1-phosphate (S1P) receptor modulator broadened the options available on site. This means that the doctors have more options to use on patients who have failed initial treatment. In other words, the next treatment they choose can change the direction of each patient’s care. As such, the choice of IBD therapies, typified by ulcerative colitis (UC), has risen as a hot topic in clinical practice. While clinical research has made it possible to customize treatment for each patient, it has also increased competition between pharmaceutical companies. A professor of gastroenterology at A University Hospital in Busan said, "Previously, there were no options for IBD other than anti-TNF inhibitors. But many more options have become available in recent years, making the situation more complicated for prescribing clinicians.” The pharmaceutical industry is also scrambling to prioritize the lines of their treatment amid the various options becoming available. One representative example is BMS's Zeposia, which entered into a co-marketing agreement with Yuhan Corp, which owns strong domestic sales and marketing capabilities. An industry official said, "In fact, Yuhan Corp’s co-marketing agreement with BMS for Zeposia was considered quite unusual in the field. The collaboration seems to fall in line with the current situation, as the IBD market has recently become more competitive with an increasing number of treatment options and Yuhan had a need to increase its drug lineup." Also, with the increasing number of therapies available from global pharmaceutical companies, "sequencing" between existing and new drugs has become a hot topic in clinical practice. In other words, the increase in treatment options to use after initial treatment failure has created a "dilemma" as patients are allowed to switch between drugs, but not immediately. Another professor of gastroenterology at a university hospital said, "Recently, JAK inhibitors and small molecule drugs have been approved for ulcerative colitis and are being used in practice. However, the issue of side effects needs to be considered as well as benefits. Because complications such as herpes zoster and blood clots can occur when using these drugs, the new drugs are more commonly used on patients that have received shingles vaccinations and relatively young patients." He added, “In the JAK inhibitor class, Jyseleca is the only JAK inhibitor that can be prescribed directly after azathioprine. In clinical studies, RInvoq has shown promise in ulcerative colitis and Crohn's disease. However, the use of other JAK inhibitors requires azathioprine to be first removed, which is problematic for physicians because they have to remove azathioprine, which they consider effective for the patients.” In other words, while prioritizing the use of the right treatment for each patient, the sequencing of the treatments is currently being determined at the doctors’ discretion based on clinical research. As a result, therapies that are deemed to be the most effective based on the clinical studies that support their approval and reimbursement are being placed in the "last line of defense" and used as a last resort in practice. However, there is an opinion that this approach is not optimal and that prescriptions should be based on a comprehensive analysis of the patient's disease severity and socioeconomic status. There are also those who believe that they should wait and refer to the revisions made to the guidelines published by the Korean Association for the Study of Intestinal Diseases, which specializes in the disease. Professor Byong Duk Ye, Professor at the University of Ulsan College and Treasurer of KASID, said, "This is always a problem because there is no right answer. Especially, in the case of Rinvoq, there are opinions that its use should be delayed as much as possible because it is superior in clinical or endoscopic aspects compared to other agents. The drug should be used in combination with the patient's personal disease status and socioeconomic status." Ye added, "It is not necessarily a good treatment strategy to postpone the use of Rinvoq because it becomes less effective when used in later stages of the disease. It may be better to use it earlier to control inflammation. The final decision should be made in consultation with the patient, and we plan to publish revised KASID guidelines regarding the increased number of IBD treatment options available.”