- LOGIN
- MemberShip
- 2026-05-04 00:25:50
- Company
- Novo Nordisk and Lilly post strong performance
- by Son, Hyung-Min May 08, 2024 05:48am
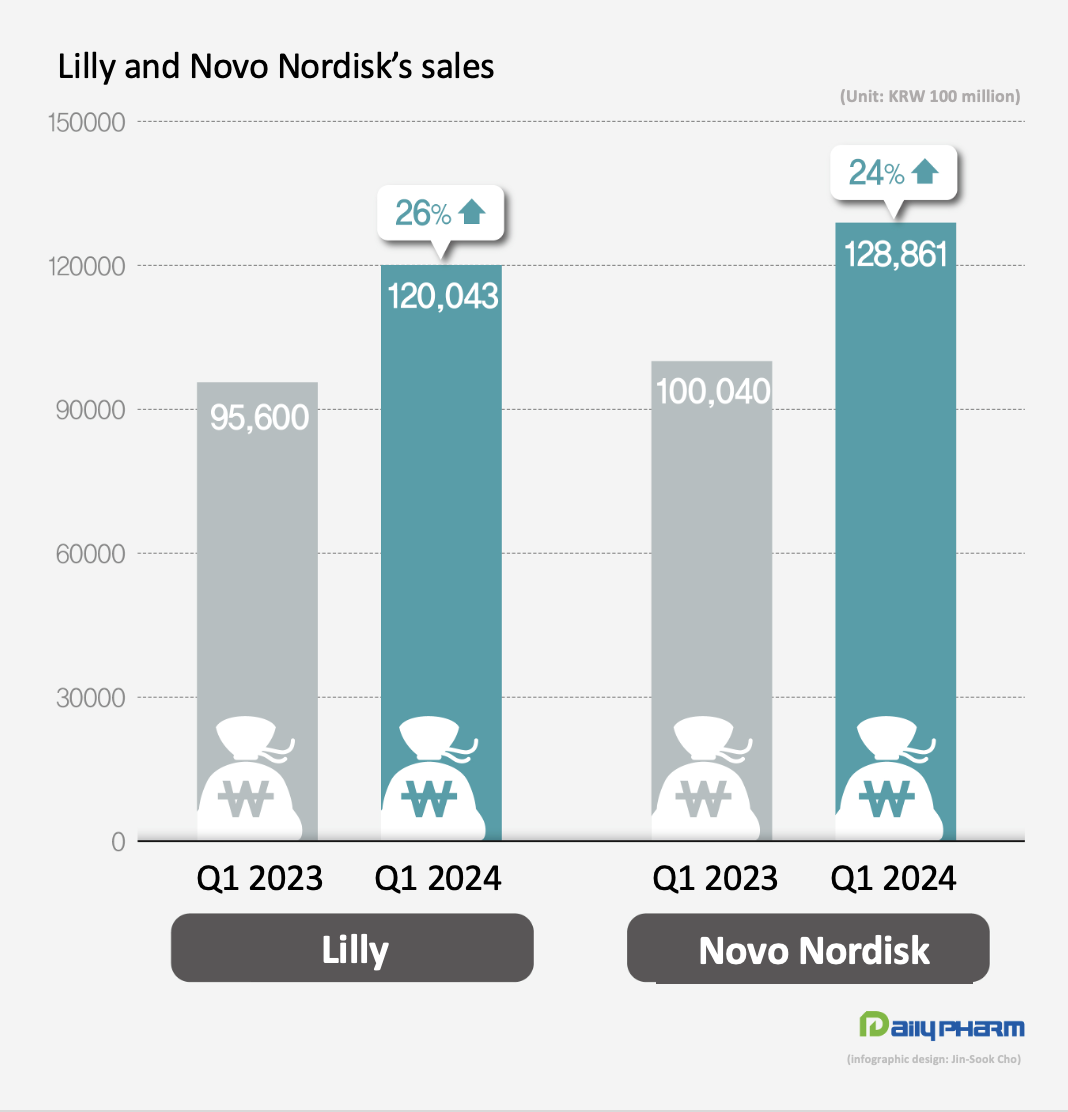
- The performance of Novo Nordisk and Eli Lilly, which released blockbuster diabetes and obesity drugs, have improved greatly in Q1 this year. Novo Nordisk's GLP-1 class diabetes drugs together generated KRW 10 trillion in quarterly sales. Lilly's obesity drug Zepbound posted sales of KRW 700 billion in Q1 this year, reaching nearly 1 trillion won in only half a year since its launch. According to KoreaBio data on the 3rd, Novo Nordisk's first-quarter sales rose 24% YoY to KRW 12.886 trillion (DKK 65.349 billion). The exchange rate was based on the basic rate of exchange as of May 2. Novo Nordisk's diabetes medicines generated sales of KRW 9.8456 trillion, up 24% YoY. In particular, sales of GLP-1 diabetes medicines surged 32% YoY to KRW 6.8981 trillion. Novo Nordisk's GLP-1 class diabetes drugs include Ozempic, Rybelsus, and Victoza, which are semaglutide and liraglutide drugs. Sales of obesity treatments totaled at KRW 2.1759 trillion, up 42% from Q1 2022. Specifically, Wegovy’s sales rose 107% to KRW 1.849 trillion. As of February 2024, the global market share of Novo Nordisk's diabetes treatments was 34%, including 35% in North America, 30% in Europe and 32% in China. Its global share of obesity medicines amounts to 85%. Lilly sees strong sales of diabetes and obesity drugs Lilly also reported first-quarter sales of KRW 12.43 trillion (USD 8.77 billion), up 26% YoY, driven by new diabetes and obesity drugs. The increase was driven by the company’s new products. Sales of its new products launched in 2022 and thereafter jumped 495%, bringing in KRW 3.27 trillion in Q1, up from KRW 550 billion in Q1 last year. Mounjaro’s revenue increased 218% from KRW 780 billion in Q1 last year to KRW 2.48 trillion in Q1 this year, recording a revenue of KRW 2.08 trillion in the U.S. alone. Mounjaro is a type 2 diabetes treatment developed by Eli Lilly that has a dual effect on glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP). By acting on GLP-1 and GIP, Mounjaro provides further blood glucose control. Mounjaro has also been shown to have dramatic weight loss benefits. Last year, Lilly also launched Zepbound, an obesity drug that contains the same substance as Mounjaro, after confirming its weight-loss benefits in clinical trials. The drug has become a global blockbuster only half a year after its launch, posting sales of KRW 71 billion in Q1. Demand for GLP-1 class drugs surge...company will address supply issue Novo Nordisk and Lilly are working to ensure smooth production of their GLP-1s, which are experiencing supply shortages. Currently, GLP-1 medicines are experiencing global stock-outs due to a surge in demand. Novo Nordisk plans to accelerate production by acquiring Catalent’s plant from Novo Holdings. Since Novo Holdings acquired Catalent last year, it has handed over 3 plants to its subsidiary, Novo Nordisk. Lilly has recently signed contract development and manufacturing organizations (CDMOs) with National Resilience in the U.S. and BSP Pharmaceuticals in Italy to increase its production capacity. To further increase its production facility in the mid-to long-term, Lilly recently acquired Nexus Pharmacutical's manufacturing facility in the U.S. and broke ground on a parenteral (injectable) manufacturing plant in Germany, both of which are expected to be operational by the end of 2025 and 2027, respectively.
- Policy
- MSD’s Cancidas will retain premium pricing for up to 5 yrs
- by Lee, Tak-Sun May 08, 2024 05:48am
- MSD's antifungal injection Cancidas’s premium pricing will be maintained for 5 years after generic entry. Originally, the price should have been adjusted to 53.55% of the highest price, but for various reasons, its price has remained at the level of 70% of the highest price. According to the industry sources on the 6th, Cancidas’s drug pricing premium was supposed to end on the 1st of this month, but the pricing premium was extended for another year according to the opinion of the Drug Reimbursement Evaluation Committee. As a result, the price of Cancidas 50mg will remain at KRW 215,977 and Cancidas 70mg at KRW 275,989. Sam Chung Dang Pharm’s Casfun Inj, the only generic version of Cancidas, also maintained its markup, and its price ceiling will remain at KRW 188,198 for Casfun Inj 50mg and at KRW 238,253 for Casfun Inj 70mg for another year. In principle, after the entry of generics, the price of the original drug drops to 70% of the highest price through ex officio adjustment, and after 1 year, it becomes the same price as its generic, set at 53.55% of the highest price. However, the price of Cancidas remains at the 70% level for 5 years. In the meantime, the principle of equal pricing for generic drugs has been broken. In June 2020, the price of Cancidas was adjusted to its current price following generic entry. The adjustment was temporary and set to last until May 2021. However, a year later, the number of generic companies remained below three, so the markup was maintained for 2 more years. Then, in April of last year, the 3-year premium pricing period passed, but the company wanted to extend the period for reasons such as ensuring a stable supply of the product, and DREC accepted the request and decided to maintain the premium pricing for one more year. This year, despite the expiration of the premium pricing period (3+1year), the premium pricing period was extended another year until May 2025 on the basis that if a drug manufacturer, contract manufacturer, distributor, or importer wants to extend the premium pricing period for reasons such as ensuring a stable supply of products, the period can be extended following DREC opinion. In January 2021, the Ministry of Health and Welfare reorganized the premium pricing system to allow up to 5 years of premium pricing through 1+2+2, including 1 year of markup upon initial registration, up to 2 years of premium pricing maintenance for drugs with 3 or fewer manufacturers, and 2 years of additional premium pricing granted after DREC deliberation when the pharmaceutical company wishes to extend the premium pricing. Cancidas’s premium pricing is being maintained for up to 5 years through the new system. Cancidas’s sales in Korea had been KRW 8 billion in 2022 (IQVIA). The drug is used for ▲ Empirical therapy for presumed fungal infections in febrile, neutropenic patients; ▲treatment of Candidemia and Other Candida Infections; ▲ treatment of esophageal candidiasis; and ▲ treatment of invasive aspergillosis. Sam Chung Dang Pharm was the only Korean pharmaceutical company to launch a generic version of Cancidas in May 2020. Since then, Sam Chung Dang Pharm ‘Casfun Inj ‘ has been the only generic version that entered the market.
- Company
- Prescriptions for cephalosporin antibiotics double in 3yrs
- by Chon, Seung-Hyun May 08, 2024 05:48am
- The popularity of antibiotics in the outpatient prescription market continues. The prescription market for cephalosporin-class antibiotics has nearly doubled in the past 3 years. This ‘heyday’ in the cephalosporin prescription market is continuing, fueled by the steady increase in flu and cold cases since the end of the pandemic. According to the market research institution UBIST, the outpatient prescription market for cephalosporin antibiotics was KRW 80.4 billion in Q1 last year, up 11.3% year-on-year. Compared to the KRW 64.1 billion it posted in Q1 2022, the market has expanded 24.4% in 2 years. Cephalosporin antibiotics, which are also called ‘Cepha antibiotics,’ are antibiotics used to manage a wide range of conditions including pneumonia, sore throat, tonsillitis, and bronchitis. The prescription market for cephalosporin antibiotics has undergone significant changes during the pandemic. The prescription market for cephalosporin antibiotics shrank by 29.3% from KRW 60.2 billion in Q1 2020 to KRW 42.6 billion in Q1 2021. In the early days of the COVID-19 pandemic, the prescription market for cephalosporin antibiotics shrank significantly, with the number of patients with infectious diseases such as flu and colds plummeting due to increased personal hygiene measures such as hand washing and mask-wearing. However, the demand for cephalosporin antibiotics surged with the explosive rise in the number of COVID-19 cases in late 2021. In Q1 2022, the prescription value of cephalosporin antibiotics began to rebound, reaching KRW 64.1 billion, up 50.6% YoY. Even after the end of the pandemic last year, the demand for cephalosporin antibiotics increased due to a steady number of confirmed daily COVID-19 cases and the rising number of flu and cold cases that arose after the lifted mask mandate. In Q1, the prescription market for cephalosporin antibiotics soared 88.8% in 3 years compared to Q1 2021. Cefaclor, the leading cephalosporin antibiotic, has recently grown significantly after the prescription market contracted in the early days of the COVID-19 outbreak. The outpatient prescription market for Cefaclor shrank by 23.2% from KRW 31.8 billion in Q1 2020 to KRW 24.4 billion in Q1 2021. However, from the end of 2021, the prescription market expanded at a rapid pace. In Q1, Cefaclor’s prescription size was KRW 40.6 billion, which is a 66.4% rise in 3 years from Q1 2021. Daewoong Bio was the dominant player in the Cefaclor market. Prescriptions of Daewoong Bio's Ceclor in Q1 was KRW 3.4 billion, up 20.1% YoY. Prescriptions of Ceclor have nearly doubled in 3 years from 1.8 billion won in Q1 2021. Prescription sales of Withus Pharamceutical’s Withus Cefaclor have increased sixfold from KRW 500 million in Q1 last year to KRW 2.8 billion in a single year. Other companies in the cephalosporin market, such as HLB Pharma, Mothers Pharmaceutical, Celltrion Pharm, Samsung Pharm, and Theragen Etex, generated over KRW 1 billion in prescriptions in Q1. Cephalosporin antibiotics have recently emerged as a new cash cow for pharmaceutical companies due to such a significant increase in demand. Many pharmaceutical companies had been considering withdrawing from the cephalosporin antibiotics business due to the declining market rising raw material costs and low drug prices. However, with the recent increase in demand, pharmaceutical companies are rather facing an urgent need to secure more supply. Daewoong Bios, which has been leading the market for cephalosporin antibiotics, announced last year that it would invest KRW 50 billion to build a new plant dedicated to the production of cephalosporin antibiotics. The current cephalosporin antibiotics plant in Seongnam, South Korea, will cease operation after this year due to outdated facilities. Once the new plant is completed, the company plans to further expand its antibiotic business. Separation of factories has become mandatory for the production of cephalosporin antibiotics since 2011. Since separate manufacturing facilities are required for its production, not many companies own dedicated facilities. One pharmaceutical company official said, "Cephalosporin antibiotics are a representative drug supplied through active consignment agreement. With the recent surge in demand, we have been struggling to secure sufficient supplies from our consignees.”
- Policy
- Will oral anemia drugs for dialysis patients be reimbursed?
- by Lee, Tak-Sun May 07, 2024 05:50am
- AstraZeneca recently withdrew Evrenzo, an oral treatment for anemia in chronic kidney disease, from the Korean market Industry interest in rising on whether oral treatments used to treat anemia in dialysis patients will be covered by health insurance in Korea. The drugs have long been approved in Korea since 2020, but one of the products recently withdrew its license. The other two have yet to be reviewed for reimbursement, raising interest. According to industry sources on the 3rd, AstraZeneca dropped the license for its Evrenzo Tab (Roxadustat, AstraZeneca), which is used to treat symptomatic anemia in patients with chronic kidney disease, on April 30. The market withdrawal comes more than 3 years after its approval in July 2021. The drug was praised for improving the convenience of anemia treatment for patients with kidney disease who previously had to depend on injections by switching to oral medication. Historically, patients with chronic kidney disease have been given injections to stimulate red blood cell production called erythropoietin (EPO) or erythropoiesis-stimulating agents (ESA) to treat anemia, a common complication of chronic kidney disease. However, Evrenzo was developed as an oral formulation that works by activating hypoxia-inducible factor (HIF), a gene involved in erythropoiesis that regulates gene expression and raised expectations on improving the convenience of treatment for the patients. After Evrenzo, JW Pharmaceuticals received approval for Enaroy in November 2022, and Mitsubishi Tanabe Pharma Korea received approval for Vadanem in March last year. Both are reportedly working to list their respective drugs for reimbursement. Under these circumstances, Evrenzo's market withdrawal has raised concerns that the authorities may have a negative stance toward the reimbursement of oral anemia drugs for chronic kidney disease. The reimbursement of these drugs also rose as an issue at the National Assembly audit held in October last year. At the time, Democratic Party lawmaker Sun-woo Kang questioned the denial of reimbursement, to which the HIRA responded that the drugs had not been reviewed for reimbursement in key reference countries and lacked clinical evidence. In a written QA, the HIRA said, "Although the drugs are oral formulations unlike existing ESA preparations that are injectables, additional advantages such as the convenience of dosing in hemodialysis patients, which is the target patient group for approval, are unclear. Although it may be potentially useful in some patient groups such as cancer patients for whom ESA administration increases the risk of tumor progression and recurrence and patients with adverse reactions or poor response to high-dose ESA therapy, it lacks direct clinical evidence of effectiveness and safety in these patient groups.” HIRA added that it would review any additional evidence of their therapeutic benefit in future reapplications or supplemental data submitted, as well as the results of overseas assessments, but was not deliberated by the Drug Reimbursement Evaluation Committee on reimbursement adequacy thereafter. However, as Vadanem received US FDA approval in March and reapplied for reimbursement, it remains of interest whether HIRA will start a reimbursement review for the drug soon.
- Company
- Another petition for reimb listing of TNBC drug 'Trodelvy'
- by Eo, Yun-Ho May 07, 2024 05:50am
- Gilead Science Korea’s Trodelvy (Sacituzumab govitecan). There is now yet another petition requesting reimbursement listing of the new breast cancer drug 'Trodelvy'. There was already a previous posting with 50,000 votes in January of last year. It appears that another petition was posted because it has been three months without any updates. A petitioner, who introduced themselves on the national petition platform on May 2nd as a stage 4 triple-negative breast cancer (TNBC) patient, pleaded for support in need of Trodelvy reimbursement, stating, "The tumor is growing too fast. I earnestly request the community to participate to extend the treatment option to me as a stage 4 patient." There has not been any updates regarding Gilead Science Korea’s Trodelvy (Sacituzumab govitecan), a treatment of triple-negative breast cancer (TNBC), being considered for the Drug Reimbursement Evaluation Committee (DREC) after the clearance of the Cancer Disease Review Committee of the Health Insurance Review and Assessment Service (HIRA) in November of last year. Trodelvy is the first Antibody-Drug Conjugate (ADC) composed of a monoclonal antibody that binds to the cell surface antigen Trop-2 and a DNA TOP1 inhibitor payload called 'SN-38,' which destroys cancer cells. It received approval as a treatment for adult patients with unresectable locally advanced or metastatic triple-negative breast cancer (mTNBC) who have received two or more prior systemic therapies, including at least one for metastatic disease, from the Ministry of Food and Drug Safety (MFDS) in May last year. Although Trodelvy is the only drug to have demonstrated improvements in overall survival period among those used for second-line treatment or more of metastatic TNBC, it is stalled at getting the reimbursement listing due to cost-effectiveness evaluation. One factor that can anticipate reimbursement coverage is recognition for innovativeness, as seen in the case of Enhertu (trastuzumab deruxtecan), which was listed in April and received a benefit from the government based on its ICER value. Whether Trodelvy will be considered for the upcoming DREC review is to be watched. Meanwhile, Trodelvy demonstrated its clinical effectiveness through the Phase 3 ASCENT clinical study. It has shown a 49% reduction in the risk of death and a 57% improvement in progression-free survival (PFS) in adult patients with unresectable locally advanced or metastatic triple-negative breast cancer (mTNBC) who have received two or more prior systemic therapies, including at least one for metastatic disease, compared to patients who received single-agent chemotherapy (TPC, Treatment of Physician’s Choice). These effects were observed regardless of the presence of brain metastasis.
- Company
- Hyperparathyroidism drug Orkedia may be reimb in Q3
- by Eo, Yun-Ho May 07, 2024 05:50am
- ‘Orkedia,’ a drug for secondary hyperparathyroidism, has entered its final gateway to insurance reimbursement in Korea. According to industry sources, Kyowa Kirin Korea recently entered into pricing negotiations with the National Health Insurance Service for Orkedia (evocalcet), a new drug for secondary hyperparathyroidism that can develop in patients with chronic kidney disease on dialysis. If the company and the authorities reach an agreement within the 60-day negotiation deadline, the drug could be launched with reimbursement in Q3 this year. The drug passed the Health Insurance Review and Assessment Service's Drug Reimbursement Evaluation Committee last month after receiving domestic approval in November last year. Orkedia is a calcimimetic agent and acts on calcium receptors on the surface of parathyroid cells to inhibit excessive parathyroid hormone (PTH) secretion, thereby reducing serum parathyroid hormone levels Secondary hyperparathyroidism is a condition in which excessive secretion of parathyroid hormone persists due to hypocalcemia caused by decreased kidney function, leading to complications such as bone disease. Orkedia is expected to help expand treatment options for patients who are taking existing medications for secondary hyperparathyroidism. Meanwhile, Kyowa Kirin acquired the rights to cooperative research, develop, market, and manufacture Orkedia in Japan and some parts of Asia with Mitsubishi Tanabe in March 2008 and has since been developing the drug.
- InterView
- 1 year after Lynparza approved for early-stage breast cancer
- by Son, Hyung-Min May 07, 2024 05:50am
- Professor Min Hwan Kim, Department of Oncology at Severance Yonsei Cancer Hospital. It’s been over a year since Lynparza was approved for the treatment of early-stage breast cancer. Previously, Lynparza was mainly used for treating metastatic breast cancer, but it expanded its usage following the approval last year for the early-stage treatment. As Lynparza has been confirmed to have a superior drug tolerance in the real-world, experts are advocating its use at early stages to prevent cancer recurrences. During a meeting with Daily Pharm, Professor Min Hwan Kim, Department of Oncology at Severance Yonsei Cancer Hospital, shared an opinion that Lynparza should be used more in early-stage treatments. Recently, targeted cancer therapies have proven their treatment effects at early stages in the field of solid cancer, including lung cancer, breast cancer, and gastric cancer. Lynparza is one of them. Lynparza is a PARP inhibitor-class therapy developed by AstraZeneca. It was approved in 2019 as a treatment for patients with metastatic HER2-negative breast cancer who carry germline BRCA (gBRCA). The PARP1 protein has been known to be overexpressed in female cancers, such as breast cancer and ovarian cancer. Lynparza’s underlying mechanism of action is preventing PARP1 from DNA binding, thereby inhibiting further cancer progression. Previously, patients with metastatic HER2-negative breast cancer and gBRCA mutation had unmet needs in targeted therapy options. Then, PARP inhibitor, which has shown effects in gBRCA metastatic ovarian cancer, emerged as a new treatment option as it demonstrated effects in breast cancer. Furthermore, in February of last year, Lynparza expanded efficacy in treating high-risk patients with metastatic HER2-negative breast cancer and gBRCA mutation. Kim emphasized the use of Lynparza at an early stage to prevent recurrence and for breast cancer patients to return to daily life. Lynparza demonstrated effects in early-stage breast cancer patients gBRCA mutations has been pointed out as the key risk factor for breast cancer. Mutation in gBRCA complicates the DNA damage repairs. In this case, genetic changes in a normal cell can lead to cancer occurrence. Mutations in gBRCA are found in around 5-10% of the total breast cancer. Whereas the average age of diagnosis for breast cancer is 63, the average age of diagnosis is relatively early when there is a BRCA1 mutation, at an average of 44.1, and a BRCA2 mutation, at 45.1. Breast cancer patients with gBRCA mutations confer poor prognosis, and as for HER2-negative breast cancer, there is no targeted receptor, which puts patients in limited treatment circumstances. But a relief for such individuals suffering from this condition is that PARP inhibitors, which have been found effective in treating breast cancer with gBRCA mutations, are now available. Lynparza, in particular, is expanding its presence after having demonstrated its effectiveness in the Phase 3 OlmpiA clinical trial, which involved HER2-negative breast cancer patients at early stages who carry gBRCA1/2 mutations. The clinical trial involved 1,836 patients who have completed adjuvant chemotherapy either prior to or after the surgery. During the follow-up period of 3.5 years (median value), post-surgical Lynparza adjuvant therapy reduced breast cancer recurrence or risk of death by 42% compared to placebo. Lynparza group’s invasive disease-free survival (IDFS) at 4 years was 82.7%, which was 75.4% longer than the placebo, and their distant disease-free survival (DDFS) was 86.5%, showing a significant improvement compared to 79.1% in the placebo group. For this reason, Kim strongly voiced his opinion towards the use of anti-cancer agents, such as Lynparza, at early stages of cancer. When cancer relapses, complete recovery cannot be anticipated, and improvements in survival rate are rarely found. Kim said, “When cancer relapses, even if Lynparza is used, complete recovery cannot be expected, and improvements in overall survival rate have not been demonstrated. Therefore, the benefit of using PARP inhibitors at early stages is enormous. Lynparza demonstrated overall survival rate improvements at early stages of HER2-negative breast cancer, increased complete recovery rate, and has solid clinical evidence.” He also emphasized that the “Lynparza group’s distant disease-free survival (DDFS) at four years was 86.5%, which practically lowered the recurrence rate to one-third. The clinical trial involved patients with triple-negative breast cancer, in which case cancer recurrence carries a higher risk of death. Reducing the cancer recurrence for these patients means a lot since it provides life-extension.” Non-reimbursed gBRCA screening…breast cancer patients face greater burden After receiving approval for expanded indications in early-stage breast cancer last year, Lynparza prescriptions are now available for patients. The basis for approval was superior drug tolerance and low side effects in early-stage breast cancer. Kim said, “To date, there have been no patients with cancer recurrence after Lynparza use. We are experiencing that Lynparza proved superior drug tolerance in treatment settings. We initially had concerns about the potential blood diseases, such as leukemia, considering the PARP inhibitor’s characteristics, but the side effects have been generally favorable when prescribed. Additionally, there weren’t many cases of anemia and tiredness.” Until now, the majority of targeted cancer therapies have been administered as non-reimbursed despite being approved for early-stage treatment options in various cancer types. Lynparza is non-reimbursed for use as post-surgical adjuvant therapy. Therefore, Kim emphasizes that early-stage cancers should be treated with targeted therapies more. “Considering the overall medical costs, early-stage treatment is more beneficial. The initial treatment costs about KRW 20 million to 30 million per year. Such treatment lasts about two years, and costs continue to grow when treating beyond the period,” Kim said. “Therefore, in terms of the society, it is important to prevent recurrence and save costs afterward through early-stage treatments,” he added. Kim also emphasized the importance of setting reimbursement criteria for the cost of gBRCA gene screening. Currently, breast cancer patients carrying gBRCA mutations bear a greater burden due to non-reimbursed administration and the cost of gene screening. The current reimbursement criteria for gBRCA screening include △At least one family member or relative (up to third-degree relative) with breast cancer, ovarian cancer, male breast cancer, metastatic prostate cancer, or pancreatic cancer △Been diagnosed with breast cancer at age 40 or younger △Been diagnosed with triple-negative breast cancer, bilateral breast cancer, or breast cancer with concurrent ovarian or pancreatic cancer at age 60 or younger △Male breast cancer and ovarian cancer patients. Kim said, “gBRCA gene screening costs about KRW 20 million when reimbursed, which burdens patients to have it tested without reimbursement coverage. Screening is advised in the United States for those with triple-negative breast cancer, regardless of age. However, Korea’s reimbursement coverage is narrow, leading to missed cases of diagnosing patients with gene mutations.” And added, “Since mutations in gBRCA are found about 10% in patients with hormone-positive breast cancer, we have a higher possibility of missing the detection because they are excluded from the reimbursement coverage for screening.” “Because the breast cancer occurrence rate is high in Korea, and it can be higher, appropriate treatment is critical. In particular, patients’ access to innovative new drugs should be improved,” Kim commented. “In Korea, there are cases of providing patient accessibility by granting selective reimbursement when new cancer drugs are not reimbursed, but almost half of the patients give up on the treatment because of the costs. Therefore, we need a more flexible system,” Kim emphasized.
- Company
- Fate of Retevmo’s reimb in Korea receives attention
- by Eo, Yun-Ho May 03, 2024 06:00am
- No news has been heard of ever since its drug pricing negotiations broke down in August last year. However, RET inhibitors are a hard-to-forego treatment option for a small number of lung cancer patients. There are only 2 RET-targeted therapies – ‘Gavreto (pralsetinib),’ which Roche Korea introduced from Blueprint Medicines, and ‘Retevmo (selpercatinib’ by Lilly Korea – currently approved in Korea. Both drugs have attempted insurance reimbursement in Korea but were denied reimbursement last year. Adding Roche's market withdrawal for Gavreto, it would be hard for Gavreto to be listed for reimbursement in Korea. The case is not much better for Retevmo either. Retevmo, which was approved in Korea in March 2022, failed to pass the Health Insurance Review and Assessment Service Cancer Disease Review Committee (CDDC) review in May of the same year, but then passed the CDDC review in November and finally passed the Drug Reimbursement Evaluation Committee in May last year. After passing the DREC review, the company entered into drug price negotiations with the National Health Insurance Service in June, raising expectations on Retevmo’s reimbursement. However, the two ultimately failed to reach an agreement. In fact, it was the only news of a drug pricing negotiation failure reported in the past year. As a result, it has become unclear whether or not anticancer drugs targeting RET mutations will ever be covered in Korea. However, there has been one glimmer of hope - Phase III results of Retevmo that were released in October last year. Results from Phase III trials on Retevmo - LIBRETTO-431 and LIBRETTO-531 - were presented at the European Society for Medical Oncology Annual Congress (ESMO 2023) last year. The results were published in the internationally recognized New England Journal of Medicine (NEJM) along with the congress presentation. The LIBRETTO-431 trial presented at the meeting compared Retevmo with platinum-based chemotherapy±pembrolizumab as a first-line treatment in patients with advanced or metastatic RET fusion-positive NSCLC. Key findings in the trial showed that in the ITT-pembrolizumab population, the median progression-free survival (PFS) by an independent centralized review committee (BICR) was 24.8 months in the Retevmo arm, and 11.2 months in the control arm, with a hazard ratio of 0.465. The overall response rate (ORR) by BICR was 83.7% in the Retevmo arm, which was statistically significantly higher than the 65.1% in the control arm. Retevmo was granted conditional authorization for conducting a Phase III trial and had trouble during the registration process as the authorities requested the company for data equivalent to a Phase III trial due to its lack of a Phase III trial. This led to criticism about the evaluation criteria for conditionally approved drugs that were granted fast-track review at the time. Retevmo, which applied for fast-track status under the accelerated review system, had been in reimbursement discussions for about a year and a half to no avail. This time, however, the company has secured solid Phase III trial results. Now it remains to be seen whether Lilly will be willing to try again and whether the government will be willing to reimburse the RET inhibitor. In 2020, Retevmo was approved as the first treatment option for cancer patients with RET alternations in the US after the FDA reviewed the drug through the Accelerated Approval and Priority Review pathway and granted the Breakthrough Therapy & Orphan Drug Designation.
- Policy
- Handok’s imported PNH drug Empaveli is approved in Korea
- by Lee, Hye-Kyung May 03, 2024 05:53am
- The Ministry of Food and Drug Safety (MFDS) announced on the 29th that it has approved Handok's imported new drug Empaveli Inj (pegcetacoplan). Empaveli binds to complement proteins C3a and C3b and inhibits the complement chain reaction, inhibiting intravascular and extravascular hemolysis. The drug is expected to help expand treatment options for adult patients with paroxysmal nocturnal hemoglobinuria**. The complement system is a part of the body’s innate immune system and helps the body fight off pathogens such as bacteria and viruses. It comprises a large number of different proteins (comprised of C1 through C9) that work together to promote immunity and inflammatory responses. PNH is caused by a somatic mutation in the X-chromosome that makes red blood cells sensitive to the complement response, leading to intravascular and extravascular hemolysis extravasation. Clinically, it manifests as aplastic anemia with decreased hematopoietic stem cells. Symptoms include fatigue, jaundice due to chronic hemolysis, hepatosplenomegaly, hemolytic anemia, hematopoietic deficiency, and venous thrombosis. The MFDS said, "We will continue to make our best efforts to ensure that treatments with sufficiently verified safety and efficacy are promptly supplied based on regulatory science so that patients can gain access to expanded treatment opportunities.”
- Policy
- AZ wins nod for new breast cancer drug 'Tiroo Cap Tab'
- by Lee, Hye-Kyung May 03, 2024 05:53am
- The Ministry of Food and Drug Safety. The Ministry of Food and Drug Safety (MFDS; Minister, Yu-Kyoung Oh) stated that it has granted AstraZeneca Korea’s new breast cancer drug 'Tiroo Cap Tab (capivasertib)' on April 29th. Capivasertib inhibits the activation of AKT protein, a serine·threonine kinase. Thus, it blocks the intracellular signaling pathway, preventing the survival and proliferation of tumor cells. This drug can be used in combination with fulvestrant in adult patients with hormone receptor (HR)-positive, HER2-negative, locally advanced, or metastatic breast cancer who have one or more mutations in PIK3CA/AKT1/PTEN genes during an endocrine therapy or when the disease progresses after completion, or when relapse occurs within 12 months after adjuvant therapy. The MFDS anticipates that this drug will provide a new treatment opportunity for patients with HR-positive, HER2-negative, advanced breast cancer who cannot be treated with existing treatments. The MFDS stated that with their specialty in regulatory science, they are committed to ensuring that treatments with proven safety and effectiveness are promptly distributed to expand patients’ treatment opportunities.