- LOGIN
- MemberShip
- 2026-05-07 14:21:27
- Policy
- 'Apply preferential pricing to non-inferior new drugs'
- by Lee, Tak-Sun Aug 11, 2023 05:35am
- With the government planning to release a drug price reform plan that includes a fair value compensation plan for innovative new drugs as early as next month, attention is focused on whether the reform will include a preferential measure for new drugs that demonstrate non-inferiority. This is because most of the new drugs that domestic pharmaceutical companies have successfully developed are new drugs that have demonstrated non-inferiority to existing drugs. Until now, non-inferior new drugs have been listed at a price below the weighted average of its alternatives. Therefore, the industry has been criticizing how the prices do not properly reflect the innovativeness of the developed new drugs. In addition, industry officials have pointed out that the low drug prices set in Korea render it difficult for companies to release their drugs overseas. To address this, domestic pharmaceutical companies have requested the government to provide additional scores for non-inferior new drugs as compensation while discussing the fair value of innovative new drugs. The government's policy on providing preferred measures for non-inferior new drugs was partially revealed on the 9th at the 'Policy Discussion for the Industry’s Leap to Become a Global Pharma & Bio Center (sub: Applying an Appropriate Value to New Drugs and Measures to Revitalize the API Industry)' that was co-hosted by Rep. Choi Jae-Hyung of the People Power Party and the Korea Pharmaceutical and Bio-Pharma Manufacturers Association. Director Chang-Hyun Oh from MOHW is discussing measures to compensate for the innovativeness of new drugs at a NA policy debate At the debate, Chang-Hyun Oh, Director of the Pharmaceutical Benefits Division of the Bureau of Health Insurance Policy at MOHW introduced, ▲clinical superiority, ▲innovative company designation status ▲expedited review subject status, and ▲domestic trial status as categories that the MOHW recognizes as innovative. Although Oh did not specify whether the clinical superiority of non-inferior drugs will be accepted, industry officials believe that this is highly likely. However, while explaining the point of Korea's positive listing system, Director Oh said that the current system’s structure does not provide preferential treatment to non-inferior new drugs and that he will work to take into account the pharmaceutical companies’ opinions to the extent that it would not jeopardize health insurance’s finances. An industry official who attended the event said, “Oh’s remarks may mean that only drugs that show clinical superiority can receive preferential treatment under Korea’s positive listing system and that non-inferior drugs are not subject to such treatment. However, the government also said it will consider reflecting the concept of an innovative new drug that was discussed by the public-private consultative body, such as taking into account the company’s innovative company status, domestic clinical trial status, MFDS expedited approval track status, etc., In that case, the non-inferiority criteria may not be important." Oh also added that the announcement was delayed due to the financial impact simulations the government conducted to assess the impact of the innovative new drug value compensation plan, and the results are likely to be released next month. The value of compensating non-inferior drugs was also emphasized by Gwan-Woo Park, a lawyer at Kim & Chang, who gave a presentation that day. Park, who had worked at the Health Insurance Review and Assessment Service for 4 years after graduating from Sahmyook University College of Pharmacy, said that most new best-in-class drugs that treat chronic conditions are being listed at 90% of the weighted average price of alternative drugs. Park said, “When a new drug for a chronic disease is released, it is difficult to convert the drug’s benefit into life expectancy extension or health-related life indicators required for QALY (quality-adjusted life year) calculation even if the drug has demonstrated clinical superiority. Therefore, a very low ICER (Incremental Cost-Effective Ratio) threshold is applied to those drugs. In particular, for indications that have generics drugs released, it is difficult for new drugs to obtain a price higher than that of the generics." Park explained that this was why most of the new drugs for chronic diseases are listed at 90% of the weighted average price of alternative drugs that were already listed for reimbursement. New drugs that were recently developed by domestic pharmaceutical companies are non-inferior drugs that target chronic diseases and are often listed at the weighted average price level of alternative drugs. On this, the pharmaceutical industry believes that for non-inferior new drugs to be properly valued, compensation should be provided so that the patients can receive the highest price of its alternatives.
- Policy
- Health insurance finance approved by the government alone
- by Lee, Jeong-Hwan Aug 11, 2023 05:35am
- It was pointed out again that health insurance finance should be included in the national finance and operated as a fund. There are concerns that if the health insurance finances are managed without going through deliberation by the National Assembly as it is now, transparency will be reduced and it can lead to negligence. The current method of independently reviewing and approving health insurance finances by the Ministry of Health and Welfare has also been criticized for being excessively discretionary and reducing the authority of health insurance subscribers. On the 10th, the National Assembly Budget Office announced this through an analysis of the Ministry of Health and Welfare’s financial statements for fiscal year 2022. Currently, health insurance finance is being operated through the health insurance general account of the National Health Insurance Corporation. The national pension, public servants pension, military pension, teacher pension, employment insurance, industrial accident compensation insurance, and long-term care insurance for the elderly are included in the national finance and operated as a fund. The Ministry of Budget and Policy considered it a problem that decision-making on health insurance finances was made without external control by the Health Insurance Policy Deliberation Committee, which was established and operated under the Ministry of Health and Welfare, and the Ministry of Health and Welfare approved NHIS accounting, budget, and settlement. It is unreasonable that the Ministry of Health and Welfare, which is the main body of health insurance policy establishment, has the right to review the budget and settlement of health insurance projects at the same time. The Ministry of Budget and Policy said that it is necessary to strengthen the National Assembly's control over the health insurance finance managed outside of the national finance, and to strengthen the transparency and accountability of financial operations. As a basis for this, it was said that national insurance premiums, which are the main financial source of health insurance finances, are in fact a quasi-tax, and that the government subsidizes a total of 20% of the expected income from health insurance premiums for that year, which causes limitations in figuring out the national fiscal balance. It pointed out the problem that if the increase in health insurance fiscal expenditure is not properly controlled, subscribers and the general public who pay insurance premiums and taxes will cover the cost. In particular, the National Fiscal Management Plan includes only a portion of the health insurance budget, which underestimates the scale of health and welfare expenditures and limits the ability to accurately grasp the actual total national expenditure. In addition, it was criticized that the health insurance policyholders' voting rights were not sufficiently guaranteed as the Ministry of Health and Welfare could take the lead in making decisions on major agendas related to health insurance finance input through a separate advisory meeting without deliberation and resolution by the Health Policy Deliberation Committee. During the deliberation on the calculation of the amount of compensation for losses in the medical sector caused by the promotion of reimbursement for ultrasound and MRI examinations, there were also cases where the Ministry of Health and Welfare did not provide enough data necessary for deliberation, such as reporting to the Health Policy Deliberation Committee on reduced profits in the medical sector. In response, the Ministry of Budget and Policy ordered the establishment of a health insurance fund, reconsideration of transparency in financial operations such as health insurance expenditure and income, and concrete measures to strengthen democratic control of the National Assembly, taking into account the characteristics and conditions of health insurance finances and the lack of a control function. The Ministry of Budget and Policy explained, “If the health insurance finance is operated as a fund, it is possible to operate it flexibly compared to the budget so that it can respond appropriately to the characteristics of short-term insurance.” Next, the Office of Budget and Policy pointed out, "Political issues in the National Assembly basically conform to the principle of representative democracy. The current decision-making structure rather exaggerates the scope of the government's discretion." “Expanding health insurance coverage and securing financial soundness is the premise and goal of health insurance finance operation, and the criticism that the expansion of coverage is hindered when funded is insufficiently grounded in logic,” he said.
- Company
- Will Darzalex be reimb as 2nd-line treatment for MM?
- by Eo, Yun-Ho Aug 11, 2023 05:35am
- Whether progress will be made on the discussions on extending reimbursement of the multiple myeloma treatment ‘Darzalex’ as second-line treatment is gaining attention. According to industry sources, Janssen Korea is reattempting to apply for reimbursement of its 'Darzalex (daratumumab)' to be reviewed by the Health Insurance Review and Assessment Service's Cancer Disease Deliberation Committee. The company had succeeded in setting reimbursement standards for Dazarlex as first-line therapy for multiple myeloma in combination with Velcade® + thalidomide + dexamethasone (DVTd), and the agenda is awaiting deliberation by the Drug Reimbursement Review Committee (DREC) soon. However, the drug failed to receive reimbursement standards as second-line therapy at the DREC level in March for its DRd (daratumumab+lenalidomide+dexamethasone), DVd(daratumumab+bortezomib+dexamethasone), and DKd (daratumumab+carfilzomib+dexamethasone) indications. Therefore, whether the company will succeed in extending the much-needed Darzalex’s reimbursement to the second line this time remains a focus of attention. The NCCN and ESMO guidelines recommend Darzalex as part of standard first- and second-line combination therapy for multiple myeloma and as part of the first-line DVTd therapy in patients who are eligible for autologous stem cell transplant. Darzalex is a human monoclonal antibody that targets CD38, a cell surface protein that is overexpressed on multiple myeloma (MM) cells. The drug induces direct celluar apoptosis via ▲ complement-dependent cytotoxicity (CDC), ▲ antibody-dependent cell-mediated cytotoxicity (ADCC), ▲ and antibody-dependent cellular phagocytosis (ADCP) triggered complement-dependent cytotoxicity (CDC).
- Policy
- Out of stock of GLP-1 injections
- by Moon, sung-ho Aug 10, 2023 05:33am
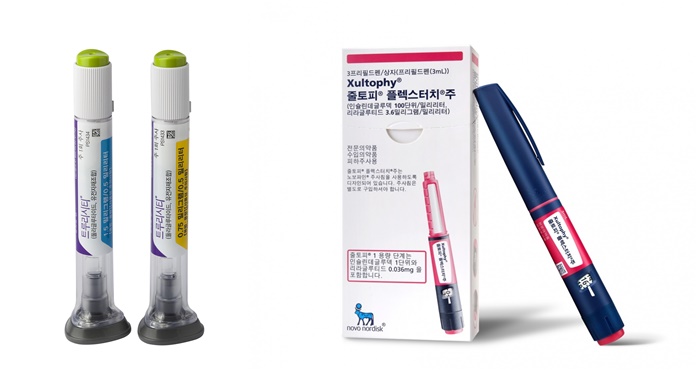
- As the news of GLP-1 (Glucagon-like peptide-1)-type diabetes treatments being used in clinical settings is reported one after another, concerns about this are growing. According to the medical community on the 4th, Novo Nordisk Pharmaceutical Korea is currently informing the clinical site of the out-of-stock news of Xultophy, a GLP-1 series diabetes treatment. Xultophy is a drug that controls blood sugar in adult type 2 diabetic patients and is a fixed ratio combination (FRC) of our company's basal insulin degludec and the GLP-1 analog liraglutide. After approval by the Ministry of Food and Drug Safety in Korea in 2019, it was applied as a benefit in May 2021 and is being used in clinical settings. However, due to the imbalance between demand and supply around the world, the aftermath also affected domestic clinical sites, resulting in out-of-stock products. The problem is that Lilly Trulicity, which was widely used as a GLP-1 diabetes treatment in domestic clinical settings prior to Xultophy, is also out of stock. In the clinical field, in the case of Trulicity out of stock, it is evaluated as the effect of concentration of production of Mounjaro, which is expected as a new drug for diabetes and obesity. A professor of endocrinology at general hospital A, who requested anonymity, said, "I heard that Xultophy may be out of stock soon after Trulicity. We inform patients in advance during treatment." The professor explained, "While checking the inventory status of the drugstore, some patients who were prescribed Trulicity are replacing it with DPP-4 inhibitor drugs." As a result, Soliqua is the only GLP-1 diabetes treatment that can be used as reimbursement in clinical settings. In the case of Xultophy, it can be replaced with Soliqua, but in the case of Trulicity, it is not easy to replace it with the corresponding treatment, the clinical field explains. Another professor of endocrinology at a tertiary general hospital who is an executive officer of the Korean Diabetes Association said, “There is no GLP-1 treatment that can be replaced with reimbursement for Trulicity, so the burden of non-reimbursement drugs will increase for patients. "For patients who are prescribed both insulin and Trulicity, Soliqua or Xultophy can be substituted, but there is no direct substitute for Trulicity," he pointed out. He said, “In this situation, as even Xultophy is out of stock, it seems that only Soliqua will be able to prescribe normally for the time being.” It is expected that the prescription of type 1 diabetes drugs will be disrupted." Meanwhile, current domestic and international diabetes treatment guidelines recommend preferentially considering GLP-1 injections, which have proven cardiovascular benefits, with SGLT-2 inhibitors in patients with atherosclerosis. Due to the high weight loss effect of GLP-1 injection, it is considered first in obese patients. Thanks to the guidelines, the domestic GLP-1 injection market, which is being applied as a benefit, is growing day by day. According to UBIST, a drug research institute, Trulicity recorded 54.7 billion won in sales last year, expanding its influence in the domestic clinical field. It recorded sales of 27.9 billion won in the first half of this year, continuing the upward trend of the previous year. Similarly, Xultophy recorded sales of 7.9 billion won in the first half of this year following the prescription record of 11.1 billion won last year. Soliqua is also showing sales growth, recording 6.3 billion won last year and 3.4 billion won in the first half of this year.
- Opinion
- [Reporter's view] Prompt benefit registration
- by Eo, Yun-Ho Aug 10, 2023 05:33am
- These days, the word 'expedited' appears frequently in the reform of the insurance benefit system. The plan is to speed up the listing of necessary new drugs by linking approval, and evaluation, and shortening the listing period at each stage. This is a good intention to quickly expand drug coverage for patients who are waiting. Shortening the insurance benefit registration period for pharmaceuticals has been discussed almost every year, and in fact, the regulatory period is getting shorter and shorter. Both the HIRA and the NHIS' evaluation and negotiation phases are similar. However, it is only a deadline for pharmaceutical companies to apply and review them. First of all, not a few pharmaceutical companies spend a considerable amount of time in the process of obtaining approval from the head office and requesting actual reimbursement. In other words, they are thoroughly flirting with an idea. If the registration process of drugs that have long passed the review period is traced back, there are many cases in which the Subcommittee on Drug Reimbursement Standards voluntarily withdraws after the decision to delay the review. However, there are many cases where this voluntary withdrawal is not 'voluntary'. In drug price negotiations between the NHIS and pharmaceutical companies, delayed decisions are made as if they were eating rice. The 60-day negotiation period is a promise. While announcing a proposal to shorten the deadline for domestically produced new drugs, is called a 'benefit'. However, there is no transparency in this whole process of the NHIS and the HIRA. Before simply promoting 'speed', concerns about transparency should be added. Just as the results of the Pharmaceutical Reimbursement Evaluation Committee and the Cancer Disease Review Committee were switched from non-disclosure to disclosure, discussions on the disclosure of information as much as possible in the new drug reimbursement process are now necessary. If drug price negotiations break down and additional disclosure of drugs that have been delayed after the application for reimbursement is made, the predictability of those waiting and watching will increase, which will lead to the establishment of effectiveness in shortening the evaluation period.
- Company
- Lotte Biologics advances CDMO Biz with Roche Diagnostics
- by Jung, Sae-Im Aug 10, 2023 05:33am
- On the 9th, Lotte Biologics announced that it had recently signed a Memorandum of Understanding (MOU) with Roche Diagnostics, the diagnostic division of the Roche Group, to advance the productivity and quality of its Contract Development and Manufacturing Organization (CDMO) business. The MOU, which was signed at Penzberg, where Roche Diagnostics Custom Biotech Center is located, aims to enhance the productivity and quality of Lotte Biologics’ pharmaceutical production. Won-jik Lee, CEO of Lotte Biologics, Rainer Mueller, Vice President of Roche Diagnostics Custom Biotech, and Kit Tang, General Manager of Roche Diagnostics Korea, attended the signing ceremony. Under the agreement, the two companies will collaborate in various areas, including the establishment of hardware and automation systems for the production process design of Lotte Biologics’ Mega Plant, as well as technical consulting and equipment support. The companies also plan to prepare a training program for the smooth operation of the ‘Bio-Venture Initiative’ that will be established in the Mega Plan Complex to support the preparation of a forum for technology development cooperation between bioventure companies. Won-jik Lee, CEO of Lotte Biologics, said, “Through the MOU, we plan to reinforce the production process capability of our company’s Mega Plant with Roche Diagnostics. Also, we hope that our collaboration with the global in-vitro leader Roche Diagnostics will create synergy and facilitate smooth operation of our Mega Plant, thereby improving the efficiency of our business while fulfilling customer needs."
- Company
- Generic drugs occupy over 70% of tamsulosin market
- by Kim, Jin-Gu Aug 10, 2023 05:33am
- The share of generic drugs in the market for prostatic hyperplasia treatments that contain tamsulosin exceeded 70%. This is interpreted as an effect of the rapid rise in generic sales while the prescription performance of original products slowed down. One variable in this market is impurities. At the end of June, impurities were detected in some products, initiating voluntary recalls. However, as only one product made the voluntary recall, its impact on the overall market is not significant yet. Prescription of tamsulosin generics rise 18% in one year... market share exceeds 70% According to the market research institute UBIST on the 9th, the outpatient prescription market for tamsulosin single-agent prostatic hyperplasia treatments in 1H recorded KRW 107.2 billion. The market increased by 10% from KRW 97 billion in 1H last year. The growth of generic products in the market led to the expansion of the overall market size. In 1H this year, the combined prescriptions for tamsulosin generics amounted to KRW 74.9 billion, an 18% increase from the past year. On the other hand, prescriptions of the original product Harnal-D decreased by 3% from KRW 33.4 billion in 1H last year to become KRW 32.3 billion in 1H this year. Prescription Performance of Tamsulosin Drugs for BPH While sales of the original drug slowed down, sales of generics rose rapidly. As a result, the share of generics in this market exceeded 70% for the first time. The quarterly share of generics exceeded 50% in Q3 2018 and then expanded further to exceed 60% in Q2 2021. Then, in the second quarter of this year, it exceeded 70%. The share of generics in the market reached 70.2% in Q2 this year. Sales of Hanmi Tams·Taminal·Bearosin rise over 10%…sales of combo drug Duodart rise rapidly Prescription performance of most of the major generic products increased by more than 10% during the past year. Hanmi Pharm’s 'Hanmi Tams' and 'Hanmi Tams OD’ recorded the highest prescription performance among generic tamsulosin drugs in 1H this year. The combined prescription of the two products in 1H this year recorded KRW 19.2 billion, up 11% from the KRW 17.3 billion the two drugs had made in 1H last year. In particular, prescriptions of Hanmi Tams OD rose from KRW 4.6 billion to KRW 6.2 billion in one year, driving the growth of the entire product line. Hanmi Tams OD is an orally disintegrating tablet version of Hanmi Tams, which is a capsule formulation. In addition, the prescription performance of all products with half-year prescriptions that exceed KRW 2 billion increased by more than 10%. Sales of Genuone Science's 'Taminal' increased by 11% from KRW 3.7 billion to KRW 4.1 billion, and Daewoong Bio's 'Bearosin' increased by 25% from KRW 2.8 billion to KRW 3.5 billion. Prescriptions of DongKoo Bio&Pharma’s ‘Uropa,’ Celltrion Pharm’s ‘Tamsol (30%↑)', Kyung Dong Pharma’s ' Uronal (14%↑)', Dongkook Pharmaceutical’s ' Tarunal (26%↑)', Huons’s ' Tamlusindi (19%↑)' had also increased relatively greatly. One product that stands out is GSK’s ‘Duodart.’ Duodart is a combination of tamsulosin and another prostatic hyperplasia drug dutasteride. Prescriptions of Duodart had only reached KRW 0.9 billion in 1H last year, but sales had risen by more than 7 times in one year to KRW 6.7 billion. GSK released the product in Q1 last year. The variable that remains in the market is impurities. Last June, Huons voluntarily recalled some lot numbers of its Tamlusindi. This was a voluntary recall made to address concerns related to the detection of excess N-nitroso tamsulosin impurities. However, the voluntary recall was limited to Huons. No cases of voluntary recall have been reported since then. In the current situation, the impact of the impurity issue is not expected to be significant. Specifically, how much the impurities will affect the overall tamsulosin market may be revealed at the end of this year.
- Company
- Patent dispute over Entresto's patents continue
- by Kim, Jin-Gu Aug 10, 2023 05:33am
- Pic of Entresto The patent dispute over ‘Entresto (sacubitril/valsartan),’ a chronic heart failure treatment with an annual prescription of more than KRW 40 billion, has been ongoing for over 2 years now. Novartis, the company that owns the original drug, is actively pursuing a defense strategy against generic companies' patent challenges. Novartis appealed after losing the 1st trial, and three cases are being tried in the second trial. Some of the results are expected to be pronounced next month. According to industry sources on the 8th, Novartis filed a trial revocation litigation against Hanmi Pharm and Elyson Pharm regarding Entresto’s salt·hydrate patent (10-1549318). After losing to generic companies in the Intellectual Property Trial and Appeal Board (1st trial), the company filed an appeal to the Patent Court of Korea against the ruling. Due to Novartis' appeal, the number of patent disputes in the second trial increased to 3. In addition to the salt and hydrate patents, Novartis and generic companies are in dispute in the Patent Court of Korea the crystalline form patent (10-1432821) and composition/use patent (10-0984939) of Entresto. Entresto is protected by 6 patents: ▲salt and hydrate patent that expires in November 2026, ▲use patent that expires in July 2027, ▲crystalline patent set to expire in September 2027, ▲composition patent set to expire in November 2028 (10-1700062), ▲another composition patent set to expire in January 2029 (10-1589317), and ▲a use patent set to expire in 2033 (10-2159601). Among the 6 patents, generic companies have succeeded in nullifying or avoiding 2 patents. The results of the two were finalized after the generic companies won the first trial and Novartis did not file an appeal. In the case of the use patent that expires in 2033, the patent was listed after generic companies applied for marketing authorization of their generics. The generic companies have also succeeded in winning against Novartis in the first trial for the other 3 patents as well. However, Novartis chose to appeal and proceed to the Patent Court of Korea for all 3 cases. The Patent Court of Korea announced that it will make a ruling on the crystalline patent on the 14th of next month. This means that the outline of the second trial rulings regarding the Entresto patent dispute will be revealed next month. After this ruling, the other 2 rulings are expected to be made until next year. If the party that loses the 2nd trial decides to go on to the Supreme Court, the Entresto patent dispute is likely to be prolonged to more than 4 years. Since 2021, generic companies have been filing trials against Entresto's patents. Starting with Elyson Pharm, about 10 companies including Hanmi Pharm, Chong Kun Dang, and Daewoong Pharmaceutical jumped into the dispute. Meanwhile, according to the market research institute UBIST, Entresto's outpatient prescriptions amounted to KRW 42.5 billion last year. Entresto has shown rapid growth in the market, increasing prescription sales by nearly KRW 10 billion every year. Its prescription performance, which recorded KRW 5.5 billion in 2018, increased to KRW 14.3 billion in 2019, KRW 22.4 billion in 2020, then to KRW 32.4 billion in 2021.
- Policy
- MOHW to expand ‘approval-assessment-negotiation’ project
- by Moon, sung-ho Aug 09, 2023 05:49am
- With the pilot project for the parallel operation of the ‘approval-assessment-negotiation linkage’ system that was implemented to shorten the drug reimbursement process in full swing, additional drugs are expected to be selected for the project in 2H this year. This is because the health authorities started a demand survey to select additional candidates for the pilot project in the second half of the year. Therefore, industry interest is rising on which items will additionally benefit. Pic. MOHW, HIRA, and NHIS have been operating the pilot project for the parallel operation of the ‘approval-assessment-negotiation linkage’ system this year According to industry sources on the 3rd, the Ministry of Health and Welfare, Health Insurance Review and Assessment Service, and National Health Insurance Service are planning to expand the operation of the ‘approval-assessment-negotiation linkage’ pilot project in 2H this year. The health authorities have been promoting a pilot project that included the parallel operation of the approval, benefit evaluation, and drug price negotiation system. The system was implemented to address the issue of how long and complicated the process for the reimbursement of high-priced rare diseases is. The authorities prepared a system that simultaneously operates the whole approval to reimbursement and drug price negotiation process. President Suk-Yeol Yoon had pledged to expedite the listing of ultra-high-priced drugs and expand reimbursement during his presidential campaign. Accordingly, the health authorities recently selected the neuroblastoma treatment Qarziba Inj (dinutuximab, Recordati) and the progressive familial intrahepatic cholestasis treatment advanced Bylvay (odevixibat, Ipsen) as priority candidates for its pilot project. Qarziba Inj, which is manufactured by the Italian pharmaceutical company Recordati, is being supplied by the Korea Orphan & Essential Drug Center in Korea. The drug is indicated for the treatment of high-risk neuroblastoma in patients aged 12 months and above. Bylvay is indicated for the treatment of pruritus in patients 3 months of age and older with progressive familial intrahepatic cholestasis. The drug received FDA approval in 2021. In Europe, the drug was approved to treat patients from the age of 6 months with progressive familial intrahepatic cholestasis. The French pharmaceutical company Ipsen had acquired Albiero which owns Bylvay earlier this year. The health authorities are now planning to select additional candidates for the project through a demand survey in 2H this year. The drug currently being discussed is 'Pluvicto (lutetium (177Lu) vipivotide tetraxetan), Novartis' prostate cancer drug. Also, Cablivi (caplacizumab), Sanofi's acquired thrombotic thrombocytopenic purpura (aTTP) treatment, is also being considered as a candidate. An industry official who requested anonymity, said, “The pilot project will be conducted in 2H 2023 to minimize the registration period for drugs that have proven superior treatment effects for patients with no appropriate treatment and a life expectancy of less than 1 year. The authorities will select candidates for the pilot project in 1H and carry out the project in 2H.” He added, “A demand survey may be conducted for Novartis’s ‘Pluvicto’ and Sanofi’s ‘Cablivi’ in 2H this year. The drugs subject to the project need to go through the MFDS’s Global Innovative products on Fast Track (GIFT), so the GIFT system is also being extended.”
- Policy
- Insurance price ceiling reeval negotiations to end on Aug 18
- by Lee, Tak-Sun Aug 09, 2023 05:49am
- The pricing negotiations for items subject to revaluations of their insurance price ceiling in Korea are taking place from the 4th to the 18th of this month. The negotiations are expected to be completed within the deadline as the National Health Insurance Service has been discussing the measures with pharmaceutical companies in advance. Therefore, the adjusted drug price will be announced on the 1st of next month after the results of the negotiations are reported to the Health Insurance Policy Deliberation Committee at the end of this month. According to the NHIS on the 8th, the Ministry of Health and Welfare issued a negotiation order on a total of 12,800 items by 206 companies that received insurance price ceiling reevaluations. Although 16,000 items were known to have received reevaluations, items that had already completed negotiations and were adjusted accordingly were excluded from the negotiations. The Generic Drug Division of the Pharmaceutical Benefits Department of NHIS plans to divide the companies subject to negotiation into 3 types and complete the negotiations by the 18th. HIRA had received data from pharmaceutical companies until last February and conducted a re-evaluation on the price ceiling of subject drugs. The first results were released in May after the results were reviewed by the Drug Reimbursement Evaluation Committee. After the results of the first evaluation were released, companies filed objections on 1,300 items, and the review results of the objections were finally deliberated by DREC on the 3rd. Afterward, HIRA transferred the results of the re-evaluation to NHIS. The NHIS had held discussions in advance with pharmaceutical companies before the main negotiations since last April and agreed on most of the terms of the negotiations. An NHIS corporation explained, "The pharmaceutical companies cooperated well with the NHIS during the preliminary discussion period and there seems to be no problem in completing the negotiations as scheduled." The reevaluation of the insurance price ceiling has been in progress to maintain or lower the upper limit set for insured drugs depending on whether or not the listed drugs meet the criteria for bioequivalence tests and DMF listing. Drugs that satisfy both requirements – DMF and self-bioequivalence tests – can maintain their price as is, and the price of those that only meet one of the requirements is adjusted to 85%, and those that meet none are adjusted to 72.25% of the previous price. Meanwhile, the 5,000 drugs subject to the second round of reevaluations by NHIS also submitted their data last month, and their review is expected to begin soon.