- LOGIN
- MemberShip
- 2026-04-26 12:10:49
- Policy
- Ofev will be reimbursed next month
- by Lee, Tak-Sun Apr 29, 2025 05:57am
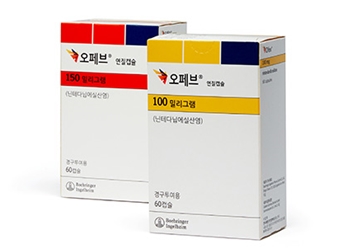
- Product photo of Ofev Ofev Soft Cap (nintedanib esylate, Boehringer Ingelheim Korea) , which was approved in South Korea in 2016, will be listed for reimbursement next month, creating an opportunity for follow-on drugs. It took a long time to secure reimbursement, and with its compound patent already expired, generic manufacturers have obtained marketing authorization and are now awaiting reimbursement. Generic manufacturers plan to apply for reimbursement immediately upon Ofev’s listing to receive the same reimbursement price and commence market sales soon. Some generic companies are even securing distribution channels by launching non-reimbursed versions before the reimbursement takes effect. According to industry sources on the 28th, Ofev soft cap will be reimbursed from next month at KRW 26,220 for the 150 mg and KRW 20,960 for 100 mg. After Ofev was approved in South Korea in October 2016, the drug applied for reimbursement in October 2020 but was deemed non-reimbursable, and the company re-applied for reimbursement in March of last year. Ofev has secured three indications. At the time of its domestic approval in October 2016, it was indicated for idiopathic pulmonary fibrosis (IPF), in February 2020, for systemic sclerosis-associated ILD, and in June 2020, for chronic fibrosing ILD with a progressive phenotype (PPF). The current reimbursement criteria cover only ILD with a PPF. The Health Insurance Review & Assessment Service (HIRA) determined that reimbursement for IPF was not appropriate, as the company did not submit separate cost-effectiveness evidence. In the case of IPF, Ildong Pharmaceutical's Pirespa Tab (pirfenidone) established a dominant position when they were reimbursed under a risk-sharing agreement (RSA) starting in October 2015. Subsequently, generic pirfenidone formulations entered the market, and Pirespa Tab's RSA ended in October 2017. Currently, pirfenidone formulations from Ildong Pharmaceutical, Yungjin Pharmaceutical, Kolon Pharma, and Korea United Pharm are listed for reimbursement. When Pirespa entered the RSA, it was difficult for follow-on products in the same indication to be included in the scheme, making reimbursement listing for Ofev challenging. After securing Ofev's three indications in 2020, the company was reportedly focused on obtaining reimbursement for PPF, a segment with no market competition. The Drug Reimbursement Evaluation Committee (DREC) recognized clinical utility, citing the significant improvement in the annual decline rate of forced vital capacity (FVC) compared with placebo and judging that the cost-effectiveness ratio fell within an acceptable range, deeming reimbursement appropriate. Reimbursement also includes patients with systemic sclerosis-associated interstitial lung disease who exhibited delayed lung function decline. It is estimated that approximately 329 patients will be eligible for Ofev reimbursement in Korea. With reimbursement, annual out-of-pocket drug costs are expected to amount to KRW 5.74 million, significantly reducing the financial burden. Under non-reimbursed status, costs amounted to approximately KRW 19.14 million. However, the imminent entry of generic versions poses a threat to Ofev. Ofev's compound patent expired on January 25 of this year. As a result, generic manufacturers have either already launched their products or are preparing to do so following approval. The currently approved generics are Daewoong Pharmaceutical's Opevia Tab, Yungjin Pharm's Nintebro Tab, and Ildong's Cuinnta Tab. With Ofev being listed as an innovator drug, these generics are now more likely to receive reimbursement within three months of their listing applications. If they apply for reimbursement in May, they could be covered as early as August. The fact that the compound patent has expired and that nintedanib is designated as an orphan drug allows it to receive the same top reimbursement price as the original, creating opportunities for the generics. In particular, companies that have already established a foothold in the pulmonary fibrosis market with pirfenidone formulations can expect synergies by maintaining their existing customer base while expanding their product line. Pirfenidone and nintedanib have different reimbursed indications. Last year, pirfenidone formulations posted sales of KRW 34 billion for Ildong's Pirespa (according to UBIST) and KRW 4.9 billion for Yungjin's Fybro. Yungjin began marketing immediately after the patent expired, while Ildong recently started non-reimbursed marketing. Ildong held a symposium on the launch of Cuinnta Tab on the 26th–27th at the Gravity Chosun Seoul Pangyo Hotel, attended by approximately 80 respiratory medicine specialists from across the country.
- Policy
- 13 items including Jakavi receive price cuts in May
- by Lee, Tak-Sun Apr 29, 2025 05:56am
- Starting May 1, the insurance price ceiling of 13 items on the drug reimbursement list will be reduced. Among them, five items are voluntary reductions requested by the manufacturers. According to industry sources on the 28th, the insurance ceiling prices of 13 items will be reduced in May, including the price of Jakavi Tab, which will be lowered based on the Price-Volume Agreement. Jakavi Tab (ruxolitinib phosphate, Novartis), a treatment for myelofibrosis, will have its price reduced under Type B Price-Volume Agreement negotiations. Type B negotiations are conducted if the maximum price was previously adjusted under Type A negotiations, or if the claims amount for the same product group has increased by more than 60% compared to the previous year's claims amount without Type A negotiations, or the increase is 10% or more and the increase amount exceeds KRW 50 billion. In such cases, the price is adjusted through price negotiations with the National Health Insurance Service. Accordingly, the price of Jakavi 5mg tablets will be reduced from KRW 25,962 to KRW 25,339, Jakavi 10mg tablets from KRW 38,943 to KRW 38,398, Jakavi 15mg tablets from KRW 52,199 to KRW 59,460, and Jakavi 20 mg tablets will be reduced from KRW 52,213 to KRW 50,960. Lorviqua, reimbursement for which has been expanded to cover the reimbursement of first-line treatment for anaplastic lymphoma kinase (ALK)-positive locally advanced or metastatic non-small cell lung cancer, underwent a procedure to adjust the maximum price in accordance with the expansion of the scope of use of risk-sharing agreement drugs. As a result, the price of Lorviqua Tab 25mg will be reduced from KRW 52,819 to KRW 51,234, and the price of Lorviqua Tab 100mg will be reduced from KRW 158,457 to KRW 153,703. Two migraine treatment drugs that contain naratriptan, will have their prices reduced due to the expiration of the pricing premium. This is because there are now four or more Naratan ODT 2.5mg products available. The health authorities terminate the premium pricing immediately when the number of companies with the same formulation registered after the expiration of the premium pricing period (one year) reaches four or more. As a result, the price of CMG Pharm’s Narafil ODF 2. 2.5mg will be reduced from KRW 2,437 to KRW 2,193, and Yuyu Pharmaceutical's Nagran ODT 2.5mg will be reduced from KRW 2,867 to KRW 2,193. These products were previously granted first-generic exclusivity last month, but the premium was terminated within a month due to the introduction of same-ingredient products. A total of 5 products will have their price ceiling reduced following voluntary price reduction requests from manufacturers. These include 3 products from Daewoong Bio (Serotapin Tab), one from Bukwang Pharm (Ariplus Tab), and one from Hyundai Pharm (DM Duo Tab). The price of Serotapin Tab 25mg will be reduced from KRW 274 to KRW 230, Serotapin Tab 100mg from KRW 688 to KRW 544, and Serotapin Tab 200mg from KRW 1,012 to KRW 927. The price of Ariplus Tab will be adjusted from KRW 3,879 to KRW 2,990, and DM Duo Tab will be adjusted from KRW 3,879 to KRW 3,658. Ariplus and DM Duo are donepezil + memantine combination drugs that were listed for reimbursement in March. Bukwang and Hyundai voluntarily lowered their drug prices just two months after their release.
- Policy
- Will Enhertu be reimb for HER2-low cancer in Korea?
- by Whang, byung-woo Apr 28, 2025 05:55am
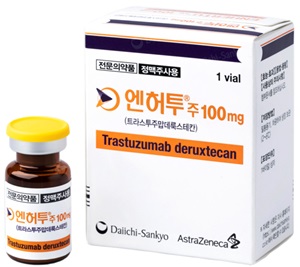
- Results of the deliberation on the reimbursement expansion of the new antibody-drug conjugate (ADC) Enhertu (trastuzumab deruxtecan) for HER2-low breast cancer and lung cancer are drawing attention. Pic of Enhertu According to industry sources, the Health Insurance Review and Assessment Service's Cancer Disease Deliberation Committee (CDDC) is scheduled to hold a meeting on the 30th to review 2 additional indications for Enhertu. The indications under review are ▲HER2-low metastatic breast cancer and ▲HER2-mutated non-small cell lung cancer (NSCLC). If the reimbursement expansion is approved, this is expected to expand treatment access for breast cancer and lung cancer in Korea. Both indications were approved by the Ministry of Food and Drug Safety in May last year based on the DESTINY-Breast04 and DESTINY-Lung02 clinical studies. Notably, the trials demonstrated the efficacy of Enhertu in HER2-low breast cancer, where treatment options were previously for HER2-negative status patients, and marks the emergence of the first and only targeted therapy for HER2-mutated lung cancer. Additionally, Enhertu has expanded its indication to include HER2 ultra-low expression in the United States by the FDA, suggesting its potential as a new standard treatment option for patients with metastatic breast cancer across the entire spectrum of HER2 expression, including HER2-positive, HER2-low, and HER2 ultra-low expression breast cancer. The main point of the CDDC review was also focused on how to evaluate Enhertu's efficacy in HER2-low expression breast cancer, where existing HER2-targeted therapies have shown limited efficacy, despite the significant improvement in treatment outcomes for HER2-positive breast cancer achieved by existing HER2-targeted therapies. Previously, HER2-positive breast cancer was defined as “HER2-positive if IHC 3+ or IHC 2+ and ISH-positive, and HER2-negative if IHC 0, IHC 1+, or IHC 2+ and ISH-negative.” Joohyuk Sohn. Professor of Medical Oncology at Yonsei Cancer Center, said, “With the domestic approval of Enhertu's indication for HER2-low metastatic breast cancer, patients previously classified as HER2-negative with limited treatment options now have a new treatment option. This is expected to further improve the treatment landscape for HER2-positive metastatic breast cancer in Korea.” Enhertu is the first anti-HER2 agent to demonstrate treatment benefits in HER2-low metastatic breast cancer, redefining the definition of HER2-low and presenting a new paradigm for metastatic breast cancer treatment. Another key point is that patients with HER2-low breast cancer account for nearly half - approximately 45% to 55% - of all breast cancer patients. Additionally, HER2-low breast cancer accounts for approximately 60% of HER2-negative breast cancer cases. Apart from the benefits of Enhertu, this means that the financial burden on health insurance due to the large number of patients would also likely need to be taken into consideration to a certain extent. If reimbursement is expanded to include indications such as HER2-low breast cancer and HER2-mutated non-small cell lung cancer, this is expected to increase Enhertu’s insurance claims amount significantly. This is why there are industry views that the reimbursement expansion will depend on the financial sharing plan proposed by the pharmaceutical company. However, when Enhertu was listed for reimbursement in Korea last April as a treatment for HER2-positive metastatic breast cancer and gastric cancer, the government had flexibly applied the ICER threshold to grant its reimbursement. In March, Daiichi Sankyo reportedly applied for and held a drug briefing session on Enhertu’s use in HER2-mutated non-small cell lung cancer. Drug information briefing sessions were introduced in 2010 to enhance the transparency and objectivity of evaluations by facilitating mutual sharing of information between pharmaceutical companies and reviewers regarding new drugs. Daiichi Sankyo also utilized this system during the initial approval of Enhertu. Enhertu was jointly developed and commercialized by Daiichi Sankyo and AstraZeneca. In South Korea, it is co-developed and promoted by Daiichi Sankyo Korea and AstraZeneca Korea, with distribution handled by Daiichi Sankyo Korea.
- Policy
- 'Social discussions needed for indication-based pricing'
- by Lee, Jeong-Hwan Apr 28, 2025 05:54am
- Won-Joon Cho, head of the Democratic Party There have been calls for caution regarding the introduction of an “indication-based drug pricing system,” to improve patient access to multi-target anticancer drugs that treat various types of cancer. The concern is that if the insurance drug price for a specific disease among the multiple indications of an anticancer drug increases, the insurance drug price for other diseases may decrease, thereby hindering patient access. Suggestions were also made that it is necessary to discuss whether the introduction of an indication-based drug pricing system is a good alternative, whether expanding the risk-sharing agreement (RSA) is a more realistic option in the short term, or whether other policy approaches are needed, and to go through a process of reaching social consensus. On the 25th, Won-Joon Cho, senior expert on health and welfare policy and head of the Democratic Party's presidential election pledge task force, made the following statement regarding the indication-based drug price system. Recently, a debate on “Eliminating inequality in access to innovative new drugs and improving regulations” was held at the National Assembly, hosted by Democratic Party lawmakers Mi-hwa Seo, Yoon Kim, and Jong-tae Jang and organized by the Korean Research-based Pharmaceutical Industry Association (KRPIA). At the debate, there was a wide argument on how the current single drug pricing system in Korea is limiting patients' access to high-cost anticancer drugs like Keytruda and Opdivo, despite their approval for various indications, and that an indication-based drug pricing system should be introduced to address this issue. Won-Joon Cho noted how certain lung cancer treatments have over 30 indications and that he understands why an indication-based drug pricing system is being proposed. However, he pointed out that it is important to consider the paradoxical issue that raising the price of the drug for a specific indication could reduce patient access to the drug itself or lower the likelihood of its health insurance reimbursement listing. Cho explained, “If the price for a specific indication becomes excessively high, it could paradoxically reduce patients' access to medications or lower the likelihood of insurance coverage. Theoretically, while drug prices may decrease for some indications, others will inevitably increase.” He added, “On a practical level, there are concerns about whether the Health Insurance Review & Assessment Service (HIRA) will be able to track and manage (drug price claims, etc.) for each indication and whether errors in entering indications and false claims can be controlled. The drug price negotiation process is also likely to become complicated and opaque.” Cho explained that this is why it is necessary to carefully examine whether introducing a system that differentiates drug prices by indication is the best alternative whether there are other policy alternatives, and the need to secure empirical evidence. He stated, “At this point, we need to discuss whether a differential drug pricing system based on indications is a significantly better alternative than the current drug pricing system, whether expanding the RSA is a more realistic alternative for now, or whether a different approach is necessary. Any discussion of institutional changes must be preceded by verification and evaluation, and there must be sufficient empirical evidence based on case studies.”
- Policy
- ‘Should apply blended pricing and reimbursement rates’
- by Lee, Jeong-Hwan Apr 25, 2025 05:59am
- With multiple drugs with multiple indications, such as multi-targeted immunotherapy drugs, being approved in Korea, there have been claims that the introduction of an “indication-based drug pricing system” is necessary to improve patient access to treatment and ensure equity. In particular, the argument was made that ‘blended pricing,’ which sets different prices for each indication, could reflect the value of each indication while maintaining a single price, thereby increasing social acceptability, and that it could be introduced without conflicting with the current drug pricing system in Korea, which is based on a single price structure. Ultimately, after taking the first step with “blended pricing,” the industry recommended that the government should introduce a “differentiated reimbursement rate system” based on real-world data accumulated for each indication in order to reflect the value of drugs for each disease and speed up reimbursement for patients. Jung-hoon Ahn, Professor of Health Convergence at Ewha Womans University Graduate School, will present these views at a policy discussion forum titled “Resolving Inequality in Innovative New Drugs and Regulatory Reform” co-hosted by the Democratic Party of Korea lawmakers Mihwa Seo, Byung-Hoon So, Yoon Kim, and Jong-Tae Jang on the 24th. The forum is organized by the Korean Research-based Pharmaceutical Industry Association (KRPIA). Professor Ahn will give a presentation on the reimbursement policy for drugs with multiple indications. Professor Ahn pointed out that there are an increasing number of cases in which drugs with multiple indications are being approved in the field of anticancer drugs. In fact, as of 2018, 75% of tumor treatment drugs in the United States were approved as drugs with multiple indications, and in South Korea, 32 anticancer drugs with multiple indications are eligible for reimbursement. In South Korea, drug prices are determined based on the active pharmaceutical ingredient contained in the drug, making it difficult to set and reflect separate prices for individual indications. This means that even drugs with multiple indications are assigned a single insurance reimbursement ceiling. Professor Ahn expressed concerns that the value of individual indications is not sufficiently reflected in drug prices, leading to issues such as access to treatment for patients that are covered with the expanded indications in South Korea. Taking the multi-indication immunotherapy drug Keytruda as an example, he pointed out that while it is reimbursed in Italy, Switzerland, France, Australia, Japan, and Belgium for both first-line treatment of head and neck squamous cell carcinoma and second-line treatment of endometrial cancer, it is not reimbursed for either in South Korea. In response, Professor Ahn suggested the need to introduce or improve a drug pricing system for multi-indication drugs. Specifically, Professor Ahn proposed that while methods such as “individual approval for each indication” or “differentiated reimbursement rates” could transparently reflect the value of each indication, they require legal amendments or raise concerns about equity in reimbursement amounts between patients that are applied different indications, as well as the need for preparation in the current system, including settlement mechanisms. He emphasized that the blended pricing method is highly feasible under the current reimbursement and drug price system. The logic is that applying blended pricing within the framework of risk-sharing agreements (RSAs), which are legal contracts, would allow the value of drugs to be reflected according to their indications while managing the financial risk of drugs with uncertain cost-effectiveness. Professor Ahn stated, “The country has established a value-based drug pricing system. However, while value is recognized primarily based on the primary indication, appropriate values for individual indications are not reflected. As a result, pharmaceutical companies are delaying or abandoning the launch of subsequent indications, leading to reduced access to new treatments for patients.” “I propose collecting and analyzing real-world data on claims made for each indication to establish actual value evidence for drugs, and building a system that applies differential reimbursement rates that reflect the clinical value differences by indication based on accumulated data,” said Ahn. “This is a strategic approach that complements the limitations of Korea's single drug pricing system while flexibly realizing the effects of indication-based drug price adjustments.” He added, “We can start with a practical approach, such as blended pricing (indication-weighted average price), and gradually evolve toward a differentiated reimbursement rate system that reflects indication-specific value. Blended pricing maintains a single price while reflecting the value of individual indications, making it more acceptable within the social framework.”
- Policy
- "Will consider proposal for Indication-based pricing system"
- by Lee, Jeong-Hwan Apr 25, 2025 05:58am
- Lee Joongkyu, Director of the National Health Policy at the Ministry of Health and Welfare (MOHW), at the National Assembly policy forum Regarding introducing an 'indication-based pricing system' aimed at improving patient access to medications, Lee Joongkyu, Director of the National Health Policy at the Ministry of Health and Welfare (MOHW), stated, "While it is still too early to announce when to implement the system, it is an opportune time to consider reviewing the proposal." During the 'Discussion Forum on Resolving Inequalities in Innovative New Drugs and Regulatory Reforms' at the National Assembly on April 24, Director Lee explained, "Recently, multiple indications are frequently approved for new drugs, thus presenting issues that cannot be solved in previous methods." Director Lee highlighted that the National Health Insurance's operational direction is to provide medications that citizens need in a timely manner. In other words, introducing an indication-based pricing system aimed at improving patient access to medications still requires further discussion within the Ministry of Health and Welfare (MOHW). Directior Lee said that since the Korean health insurance system operates as a sole supplier than a multiple insurance system, there will be challenges related to purchasing medications and receiving reimbursement. Despite such challenges, Director Lee agreed that solving the patient access issue by improving policy is necessary rather than simply regarding it as a financial issue. Dr Lee remarked, "We must consider whether issues related to reimbursement method of pharmaceutical have been resulted due to insufficient measures from the perspective of the system rather than a National Health Insurance expenditure issue," and added, "In my opinion, it is about time to review the indication-based pricing system." "We cannot provide an exact implemenation timeline, but the MOHW will review the measure. The MOHW is aware that if coverage under the National Health Insurance is not provided, individuals will need to purchase medications at non-reimbursed price," and Dr. Lee added, "If there are issues with the supply of quality drugs, we will certainly consider proposals."
- Policy
- MFDS to improve essential drug designation standard
- by Lee, Hye-Kyung Apr 25, 2025 05:58am
- The Ministry of Food and Drug Safety will conduct a study to improve the standards for designating essential medicines. When the national essential medicine system was first implemented in 2017, the designation focused on government stockpiles, but there have been continuous calls to expand the list to include items that require stable supply in the private medical setting. This was announced in the “Proposal Request for Research on Classification of National Essential Drugs and Measures for Stable Supply” announced by the Ministry of Food and Drug Safety on the 23rd. The MFDS designates and manages essential medicines that need a stable supply because they are necessary for medical use, such as disease control and radiation disaster prevention, Efforts have been made to ensure a stable supply of essential medicines, including improving the designation criteria, introducing a reevaluation system, providing administrative support for expedited approval, and revising laws. The study plans to review cases from other countries to develop measures to improve the current system. Following the recruitment of researchers, KRW 50 million will be invested over a period of 6 months to conduct the following: ▲survey and compare the operation and utilization of essential medicine systems in major countries; ▲analyze the current status of national essential medicine operations and explore directions for improvement; and ▲analyze the current status of utilization and explore directions for improvement to ensure the stable supply of national essential medicines. First, the study will examine the purpose of essential medicine management in other countries, classification methods (product characteristics, uses, etc.), selection criteria and procedures, and consultation processes. It will also investigate the current status of policy support and preferential measures for stable supply. In addition, the study will derive key considerations for designating national essential medicines based on the characteristics of each item and prepare proposals for improving the standards for designating national essential medicines. The study will also review the classification methods for national essential medicines by use, referencing the WHO Model List of Essential Medicines, to revise the list. The list will be revised based on a comprehensive review of the necessity of each item within the category when designating or reevaluating national essential medicines. In addition, the purpose of the national essential medicines system and the need to distinguish it from similar systems will be considered, and the scope of designation and exclusion of national essential medicines be reviewed. This study will also establish a reorganization and operational plan for the Stable Supply Council and Subcouncil to facilitate discussions on the designation and stable supply of national essential medicines. The study will identify government policy tools and collaboration requirements with relevant ministries and agencies to ensure that stable supply policies decided through the council are implemented, and will review measures to strengthen human and material infrastructure for the stable supply of essential medicines. The MFDS stated, “The supply of essential medicines continues to be an ongoing issue, and we expect the government to play a stronger role in improving the national essential medicines system and ensuring a stable supply in response to environmental changes in various fields.”
- Policy
- Psychotropic drug etomidate will be discontinued in KOR
- by Lee, Hye-Kyung Apr 24, 2025 06:01am
- The domestic supply of etomidate, a psychotropic drug scheduled to be newly designated this year, is expected to be discontinued. According to the Ministry of Food and Drug Safety's list of discontinued and shortage drugs, B. Braun Korea reported on the 21st that it would discontinue the supply of ‘Etomidate-lipuro Injection.’ B. Braun Korea explained, “The drug is scheduled to be designated as a psychotropic substance, which will result in the termination of the current sales contract with the domestic distributor by the end of this year. At this time, the possibility of renewing the contract or entering into a new contract for the drug is unclear, with the future import and supply of the drug plan also undecided.” The MFDS conducted a public consultation until the 10th regarding the “Revision of the Enforcement Decree of the Act on the Control of Narcotics” on whether to newly designate etomidate as a psychotropic drug. Etomidate has been illegally administered or misused in some medical institutions, and the MFDS announced that it will proactively designate it as a narcotic and actively manage it to ensure its safe use in Korea. B. Braun Korea explained, “The medication in question is an injection containing etomidate, and there are no other products with the same ingredient. However, medications with similar efficacy and effects, such as propofol, ketamine, and midazolam, are currently in circulation in the country.”
- Policy
- MFDS 'Review time shortened after the GIFT introduction'
- by Lee, Hye-Kyung Apr 23, 2025 06:11am
- Following the introduction of the Global Innovative products on Fast Track (GIFT) for global innovative products by the Ministry of Food and Drug Safety (MFDS) last year, the time it takes to review pharmaceuticals for severe disease has shortened significantly from the average of 115 days to 62.9 days. Furthermore, the number of approved cases for innovative new drugs increased by 3.1-fold, from 8 to 25, compared to 2022. According to the 'GIFT Monitoring and Plans' unveiled by the MFDS on April 22, the number of cases designated as GIFT increased from 6 cases in 2022 to 16 cases in 2024. The number of approved innovative new drugs also surged. (left) Number of cases designated as expedited review (right) Number of approved innovative news drugs Notably, proactively running the system has enabled short review time, which falls within 75% of the regulatory review period (within 120 days). The review period reportedly takes 62.9 days. During the regulatory review period, the time it takes to submit document supplementation is not included. An expedited review also excludes the document supplementation period. The MFDS has been operating the expedited review system since August 2020. It has introduced the GIFT for severe disease in 2022. To date, 65 cases have been designated for expedited review system, with 29 cancer drugs and 21 COVID-19 vaccines ranked by highest. In addition, the MFDS has expanded GIFT program criteria to include advanced biopharmaceuticals. For new drugs developed by innovative pharmaceutical companies, the MFDS supports early entries to the GIFT program. Notably, as the Health Insurance Review and Assessment Service (HIRA) revised the 'Specific evaluation criteria of new drugs and medicines in consideration for negotiation,' GIFT-designated new drugs are now acknowledged for 'innovativeness of new drugs' during the ICER value evaluation during the reimbursement evaluation. Furthermore, the 'Pilot Project for Integration of Product Approvals, Reimbursement Coverage Reviews, and Drug Price Negotiations,' aimed at the swift supply of severe rare diseases treatments, also considers GIFT-designated products for their program. Recordati Korea's Qarziba, the 13th GIFT-designated drug for rare cancer in children, took 89 days until marketing authorization review, and it was approved for reimbursement listing six months after approval. This year's '2nd Pilot Project for Integration of Product Approvals, Reimbursement Coverage Reviews, and Drug Price Negotiations' includes the 24th GIFT drug 'Winrevair,' the 30th GIFT drug 'Fintepla,' and the 33rd GIFT drug 'Rimqarto.' The MFDS stated, "In March, the MOHW revised the pharmaceutical evaluation criteria and newly established drug pricing evaluation for GIFT-designated new drugs developed by innovative pharmaceutical companies," and added, "Criteria for evaluating cost-effectiveness are newly established, such as providing benefits for new drugs when their clinical effectiveness is comparably improved than a substitute drug."
- Policy
- ‘Govt will resolve the supply issue of rare disease drugs’
- by Lee, Jeong-Hwan Apr 23, 2025 06:10am
- A private-public policy consultative body will be established to discuss support measures for manufacturers and sellers of rare disease drugs, medical devices, and special foods. The Korea Disease Control and Prevention Agency announced that a partial amendment to the Enforcement Decree of the Rare Disease Management Act, which provides the basis for the formation and operation of the “Consultation Body for Rare Disease Support Policies,” was approved at the Cabinet Meeting on the 22nd. The amendment was prepared to provide administrative and financial support to manufacturers and distributors to ensure a stable supply of drugs, medical devices, and special foods related to the diagnosis and treatment of rare diseases. Key provisions include the establishment and operation of a “Consultative Body for Rare Disease Support Policies” comprised of relevant central administrative agencies and related institutions to determine necessary matters such as the scope, procedures, and criteria for administrative and financial support for manufacturers and sellers of rare disease medications, medical devices, and special foods. The consultative body will be chaired by the Director-General of the Chronic Disease Control Bureau of the KDCA and consist of no more than 10 members, including officials from relevant central government agencies such as the Ministry of Economy and Finance, the Ministry of Agriculture, Food and Rural Affairs, the Ministry of Health and Welfare, and the Ministry of Food and Drug Safety, as well as other officials from relevant organizations and groups. The task force will discuss and coordinate matters such as: ▲preparing and reviewing detailed support measures for administrative and financial support; ▲sharing and utilizing information on the current status of support for rare diseases among relevant agencies; and ▲determining the scope, procedures, and other necessary matters related to administrative and financial support for the diagnosis and treatment of rare diseases. KDCA Commissioner Young-mi Jee said, “We hope that practical support for those who produce and sell medicines, medical devices, and special foods for the diagnosis and treatment of rare diseases will be strengthened. We will continue to expand cooperation with relevant ministries and private organizations to establish a management system for the entire process that includes the diagnosis, treatment, and support for patients with rare diseases.”