- LOGIN
- MemberShip
- 2026-04-25 01:06:10
- Policy
- Support grows for reform of aHUS reimb pre-approval system
- by Jung, Heung-Jun Dec 19, 2025 09:08am
- Concerns about improving the pre-approval review process for Soliris, a treatment for aHUS, has also been raised during last year's NA auditCalls to improve reimbursement access for treatments for atypical hemolytic uremic syndrome (aHUS) are gaining momentum, with the Anti-Corruption and Civil Rights Commission (ACRC) joining the National Assembly in pressing for institutional reform.Previously, the National Assembly had criticized the low approval rate of prior authorization for Soliris, an aHUS treatment, and urged regulatory relaxation.On the 17th, the ACRC has recommended system-wide improvements, including designating aHUS and other “ultra-urgent rare diseases” as a separate category and improving the system to ensure prior reviews are completed within 2-3 days.It ordered the establishment of a 48-hour fast-track review process for prior approval and the creation of a ‘Rare Disease Drug Review Committee (tentative name)’ to ensure such reviews are conducted swiftly.The ACRC has given the Health Insurance Review and Assessment Service (HIRA) an implementation deadline of December next year. If the recommendations are not implemented, the Commission plans to continue monitoring progress.ACRC investigator Joon-hyung Kim said, “We are aware of the issues raised by the National Assembly. We listened to the voices of medical professionals, patients with rare and severe diseases, and patient organizations. We also conducted an on-site investigation at HIRA this summer. Through stakeholder meetings, we consolidated opinions and finalized our recommendations. This is not limited to aHUS alone. There are several other ultra-rare diseases requiring immediate emergency care.“Kim added, ”HIRA is likely aware of the need for improvement, having conducted its own investigation. We have now communicated the recommendations along with a deadline for implementation by December next year."While these are recommendations without legal enforceability, the ACRC stated that it will actively follow up and encourage implementation if reforms are not carried out.Investigator Kim conveyed, “Even if it goes beyond December next year, we will continuously monitor whether implementation occurs and manage the situation to ensure improvements are made.”The prior approval system is a mechanism designed to obtain reimbursement approval before administering ultra-high-priced new drugs, considering the financial stability of the National Health Insurance budget.Last year's National Assembly audit pointed out low approval rates and review delays for treatments like atypical hemolytic uremic syndrome (aHUS) and spinal muscular atrophy (SMA).Meanwhile, the reimbursement criteria for aHUS treatments were partially relaxed this October.
- Policy
- Keytruda completes price negotiations for reimb in KOR
- by Jung, Heung-Jun Dec 17, 2025 09:50am
- MSD Korea’s immunotherapy drug Keytruda (pembrolizumab) has completed price negotiations with the National Health Insurance Service (NHIS), with reimbursement coverage expected to expand to additional indications starting next month.Keytruda previously received approval for reimbursement appropriateness for 11 indications, including gastric cancer and esophageal cancer, at the 9th Drug Reimbursement Evaluation Committee meetingAccording to industry sources on the 16th, MSD Korea has finalized a drug price agreement with the NHIS regarding the reimbursement expansion for Keytruda. Following review by the Health Insurance Policy Deliberation Committee (HIPDC), the Ministry of Health and Welfare is expected to issue a formal notice next month.The 11 additional indications approved by the Drug Reimbursement Evaluation Committee this time include gastric cancer, esophageal cancer, endometrial cancer, colorectal cancer, squamous cell carcinoma, cervical cancer, breast cancer, small intestine cancer, and biliary tract cancer. Approximately 2 years after the initial reimbursement expansion request in 2023, the decision now awaits only the Health Insurance Review and Assessment Service (HIRA) resolution.Previously, Keytruda was granted reimbursement for seven indications across four cancer types: non-small cell lung cancer, Hodgkin lymphoma, melanoma, and urothelial carcinoma.For metastatic or unresectable recurrent head and neck squamous cell carcinoma, reimbursement was granted for first-line treatment as ▲ monotherapy in PD-L1-positive patients, ▲ combination therapy with platinum and fluorouracil-based chemotherapy.Keytruda to show strong momentum in both regulatory approvals and reimbursement expansion in head and neck cancer.In October, the Ministry of Food and Drug Safety approved an expanded indication for Keytruda as perioperative therapy (pre- and post-surgery) in patients with resectable locally advanced head and neck squamous cell carcinoma.Given this expanded approval in head and neck cancer, MSD is expected to pursue further reimbursement expansion for the approved indications. Beyond head and neck cancer, it holds 35 indications across 18 cancer types, leaving significant potential for additional reimbursement expansion.Keytruda’s annual claims exceed KRW 400 billion, and claims are expected to increase starting next year as additional reimbursed indications start being prescribed.
- Policy
- President Lee "Review reimb of hair loss·obesity drugs"
- by Lee, Jeong-Hwan Dec 17, 2025 09:50am
- President Lee Jae Myung has drawn attention by instructing the Minister of Health and Welfare, Jeong Eun Kyeong, to specifically review the possibility of extending National Health Insurance (NHI) coverage to hair loss and obesity treatments.President Lee stated, "I previously made a campaign pledge to support hair loss medication. Isn't hair loss also part of a disease? I hear many young people use it, so have you reviewed the possibility of coverage?" He added, "I would like you to examine the potential costs, and if unlimited support poses a financial burden, consider limiting the number of doses or imposing a total expenditure cap."President Lee asked, "I assume the reason for the lack of coverage is that genetic factors cause baldness. But isn't a genetic disease also caused by genetics? It becomes a matter of defining whether something is a disease or not." He concluded, "This does not seem logical."President Lee further added, "In the past, hair loss was viewed as a cosmetic issue, but these days, it seems to be perceived as a matter of survival." He then asked, "The same seems to be true for obesity treatment. Is coverage for severe obesity medication under review?"Minister Jeong responded that it is necessary to consider medical urgency or priority when covering hair loss medication.Minister Jeong explained, "NHI supports treatment for alopecia areata caused by medical reasons. NHI does not cover hair loss due to genetic factors because its link to medical treatment is considered low." She added, "It is true that many non-covered medical services include treatments for hair loss, acne, and obesity."Minister Jeong said, "Since they are not life-threatening diseases, other treatments deemed cosmetic are also not covered by the NHI," and added, "We will review [NHI coverage] for these conditions."Regarding coverage for obesity medication, Lee Jung-kyu, Director of the NHIS Bureau, replied, "For severe obesity, we currently provide partial coverage for surgical treatments based on the Body Mass Index (BMI) criteria."Minister Jeong further explained, "We are still reviewing these medications. Since an application for reimbursement has just been submitted, we need to proceed with the review for reimbursement appropriateness.
- Policy
- ‘Expand 1st line reimb for anabolic agents to reduce healthcare costs’
- by Jung, Heung-Jun Dec 16, 2025 08:36am
- Calls have been raised for expanding reimbursement coverage for anabolic agents as first-line therapy in order to prevent osteoporotic fractures and the resulting rise in direct and indirect healthcare costs.As reimbursement for bone-forming agents is limited to second-line treatment only, experts argue that coverage should be expanded to include first-line use. Representative agents in this class include Evenity (romosozumab) and Forteo (teriparatide).Seung-hoon Baek, Director of Insurance and Policy at the Korean Society for Bone and Mineral ResearchOn the 15th, Seung-hoon Baek, Director of Insurance and Policy at the Korean Society for Bone and Mineral Research, emphasized the need for a first-line treatment strategy using anabolic agents at a National Assembly policy forum on osteoporosis fracture prevention held on the 15th.Director Baek stated, “Recent domestic and international guidelines recommend anabolic agents as a first-line treatment strategy for the very high-risk group. Global guidelines, including those from the American Association of Clinical Endocrinology, also position them as first-line treatment options.”The KSBMR also established guidelines in 2024 recommending the use of anabolic agents as first-line therapy in high-risk groups meeting criteria such as: ▲ a fragility fracture within the past year ▲ multiple fractures ▲ a bone mineral density T-score below -3.0.Director Baek explained, “If bone resorption inhibitors are administered first, there is a risk that bone formation may also be suppressed. Therefore, administering anabolic agents first is more effective for improving bone density."A study involving 1,000 women aged 75 showed that 43 fractures occurred when antiresorptive agents were used first, compared with 22 fractures when anabolic agents were used as first-line therapy, confirming a significant fracture-reduction effect.However, in Korea, reimbursement for anabolic agents is granted only if they are used after bone resorption inhibitors prove ineffective, which has been cited as a major limitation.Furthermore, the target population must meet all of the following conditions: ▲ Age 65 or older (or postmenopausal women aged 65 or older for romosozumab) ▲ T-score ≤ -2.5 ▲ History of two or more osteoporotic fractures.Director Baek emphasized, “Korea's reimbursement criteria are excessively restrictive compared to major countries overseas. Following the UK and Japan, Australia also expanded reimbursement for romosozumab as a first-line treatment for high-risk groups in early November last year. While there may be an increase in drug costs in the short term, a reduction in healthcare costs is expected in the long term. Overseas, this is the basis for its use in the first-line.”He further elaborated, “Patients who experience osteoporotic fractures incur approximately 80% higher per-patient medical costs compared to those without fractures. Preventing fractures is key to curbing rising healthcare expenditures.”Specifically, experts proposed recognizing it as a first-line treatment and expanding the target population from postmenopausal women aged 65 and over to include those aged 50 and over. The proposed eligibility criteria include: ▲ Relaxing the bone density test requirement from ≤-2.5 to <-3.0 ▲ Expanding from patients with two or more fractures to those with a fracture within the past year ▲ Patients meeting any one of the following: bone density ≤-2.5 and two or more fractures.
- Policy
- ‘Allowing drug wholesaling via platform creates conflicts of interest’
- by Lee, Jeong-Hwan Dec 16, 2025 08:35am
- Joon-Hyuk Kang, Director of Pharmaceutical Policy Division, MOHW"Just as it is clearly a conflict of interest and therefore prohibited for public officials such as lawmakers and ministers to purchase stocks in sectors related to their official duties, it is equally a clear conflict of interest and should be prohibited for platforms to engage in distribution and sales by also operating as pharmaceutical wholesalers. Doctors, pharmacists, and platforms must fulfill their distinct roles in the telemedicine process, and for this, the amendment to the Pharmaceutical Affairs Act must pass the National Assembly."The Ministry of Health and Welfare stated that allowing telemedicine platforms to operate as pharmaceutical wholesalers is not a solution to the ‘pharmacy hopping’ crisis.The Ministry directly challenged the main argument currently being used by some lawmakers and Presidential Chief of Staff Hoon-sik Kang to block the plenary session and processing of the amendment to the Pharmaceutical Affairs Act, which passed the National Assembly's Health and Welfare Committee and Legislation and Judiciary Committee with bipartisan agreement, stating it is factually incorrect. This has drawn intense attention from political circles and the healthcare and pharmaceutical sectors.Regarding how the bill banning platform wholesalers is commonly referred to as the ‘Doctornow Prevention Act,’ the Ministry stated, “It could easily be misinterpreted as a law banning platform brokerage itself. A more accurate description would be a platform conflict-of-interest prevention bill or a ban on collusion between Doctornow and drug wholesalers,” the ministry said.”On the 14th, Joon-Hyuk Kang, Director of Pharmaceutical Policy at the Ministry of Health and Welfare, met with the press corps to explain the ministry's position on the delayed plenary processing of the Pharmaceutical Affairs Act amendment proposed by Rep. Yoon Kim of the Democratic Party of Korea, which has already passed both the Health and Welfare Committee and the Legislation and Judiciary Committee review.Yoon Kim’s bill for the amendment to the Pharmaceutical Affairs Act faces plenary delay due to opposition from some lawmakers across parties and Chief of Staff Hoon-sik Kang.The Ministry maintains that, to establish a safe non-face-to-face medical environment free from platform dependency for patients, medical institutions, and pharmacies, safeguard a fair pharmaceutical distribution system, and prevent patient medication misuse, both the Medical Service Act amendment institutionalizing non-face-to-face care (already passed by the National Assembly) and the Pharmaceutical Affairs Act amendment banning platform wholesalers require urgent plenary session processing.Minister of Health and Welfare Eun-kyeong Jeong also strongly expressed her view during the previous Judiciary Committee meeting regarding the platform wholesaler ban bill. She stated that, similar to doctors and pharmacists, the amendment of the Pharmaceutical Affairs Act is necessary to prohibit platforms from abusing their monopolistic position to engage in specific pharmaceutical distribution and sales activities.Nevertheless, several lawmakers from both major parties, including So-young Lee, Han-kyu Kim, Bo-yoon Choi, and So-hee Kim, argued that “Banning platform wholesaling based solely on concerns over illegal rebates would stifle startup innovation.” Presidential Chief of Staff Hoon-sik Kang also supports these lawmakers’ position.Doctornow, which positions itself as Korea’s leading telemedicine platform, claimed that “operating a wholesaling business is merely a practical measure to resolve pharmacy hopping” and has actively lobbied against the legislation.“Allowing platform wholesalers cannot be the solution to the pharmacy hopping issue”The Ministry of Health and Welfare has fully refuted these arguments from some lawmakers, the Presidential Office, and Doctornow. First, it stated that allowing Doctornow to operate a wholesaler and directly or indirectly intervene in drug distribution and sales cannot be considered a solution to the patient pharmacy hopping crisis.The MOHW believes the claim that platforms should be allowed to operate as wholesalers to address the issue of patients using telemedicine services having to go from pharmacy to pharmacy due to lack of medication is flawed.The ministry questioned why resolving pharmacy hopping must necessarily involve allowing platforms to operate as wholesalers, suggesting that this logic itself requires serious reconsideration by policymakers.While approximately 30,000 pharmaceutical products are distributed in Korea, Doctornow reportedly handles only about 90 products—an imbalance that, according to the MOHW, demonstrates how platform-operated wholesaling could promote illegal or distorted practices.Director Kang explained, “Allowing platforms to operate as wholesalers won't solve the ‘pharmacy hopping’ issue for pharmacies. If frontline pharmacies could freely share their inventory and stock of medicines via platform apps, the ‘pharmacy hopping’ issue could be resolved.”Kang added, “With over 30,000 pharmaceuticals circulating in the market, can platforms like Doctornow, which operate wholesalers, distribute, and sell all 30,000 drugs? Currently, Doctornow handles only about. When a specific platform distributes only 90 out of 30,000 drugs, it can distort prescriptions and dispensing at affiliated medical institutions and pharmacies.“He added, ”But does that mean we should turn the platform into a large wholesaler distributing all 30,000 drugs? This would also create problems in itself. The dual role of platform and wholesaler has clear limitations.“”Serious conflict of interest issues will arise among large capital platforms if legislation fails"The MOHW warned that if the bill fails, conflicts of interest arising from platform involvement in drug distribution and sales could spiral out of control.Beyond Doctornow, larger capital-backed platforms, corporations, or even pharmaceutical companies could collude with platforms to distribute and promote drugs that serve their own interests, the ministry cautioned.Kang stated, “The purpose of the amendment is not to target a specific company like Doctornow, but to prevent broader conflicts of interest that could lead to medication misuse or collusion. Therefore, the bill needs to be reviewed during the plenary session. Just as public officials are prohibited from purchasing stocks related to their official duties due to conflicts of interest, platform-operated wholesaling presents the same problem.”He added, “The potential for illegal rebates by platform wholesalers is merely a tool. The core issue is the potential for patient medication misuse or collusion that could arise if conflicts of interest are left unresolved. During non-face-to-face consultations, platforms should only be granted and exercise authority within their specific roles, just like doctors and pharmacists.”“Platforms hold prescription/dispensing authority equivalent to doctors/pharmacists... reason for wholesaler ban”The Ministry of Health and Welfare judges that platforms like Doctor Now hold influence equal to or greater than that of doctors holding prescription authority and pharmacists holding dispensing authority in the distribution and sale of pharmaceuticals.Because physicians and pharmacists are legally prohibited from engaging in wholesaling, the ministry argues that platforms should be subject to the same restrictions.Director Kang emphasized the urgent need for consensus among the MOHW, the Ministry of SMEs and Startups, and relevant National Assembly committees that platforms can exercise pharmaceutical influence equivalent to healthcare professionals.Kang said, “The MOHW’s position is that platforms exercise prescribing and dispensing influence comparable to physicians and pharmacists. Therefore, they require equivalent regulatory restrictions, including a ban on wholesaling. The ministry had actually proposed amendments to the original bill to better protect legitimate platform functions, leading to its passage through the Health and Welfare Committee and the Legislation and Judiciary Committee.”Kang explained, “The original bill defined even the act of posting drug inventory or price information on platforms as patient solicitation and banned it outright. The Ministry views such information provision as a basic platform function and excluded it during the Welfare Committee review. The provision prohibiting pharmacy owners from offering economic incentives to platforms for patient solicitation was also removed. This was because it was difficult to distinguish between legitimate compensation for pharmacy services and other forms of inducement."He added, “Rather than getting bogged down in peripheral issues like the potential for illegal rebates or the interests of specific companies like Doctornow, I urge politicians and the media to focus on the fact that allowing platforms to operate as wholesalers themselves creates a conflict of interest. We must look toward the passage of the amendment to the Pharmaceutical Affairs Act in the National Assembly as necessary to protect public health in medicines and ensure safe telemedicine.”
- Policy
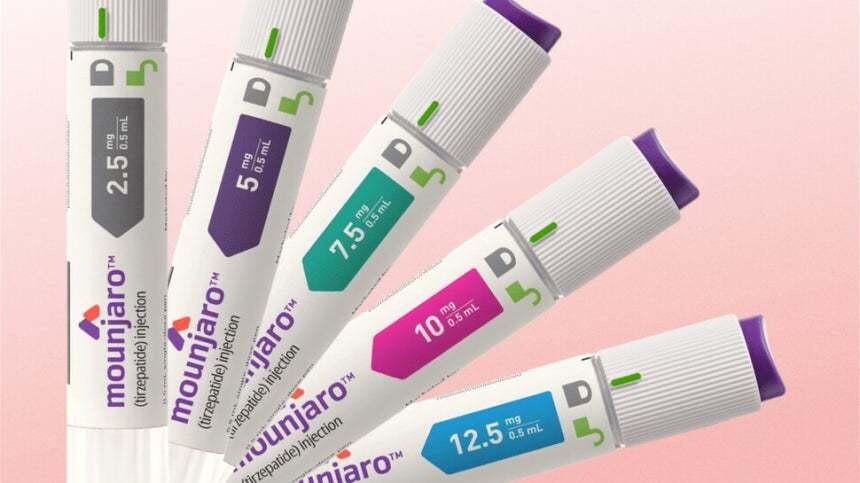
- Vial formulation of Mounjaro approved only for diabetes in KOR
- by Lee, Tak-Sun Dec 15, 2025 09:16am
- Lilly’s ‘Mounjaro Prefilled Pen Inj’Lilly has obtained Korean regulatory approval for a vial formulation of Mounjaro in Korea. Mounjaro is a GLP-1 and GIP dual agonist, and its prefilled pen formulation was launched in August as an obesity treatment.The Ministry of Food and Drug Safety approved six dosage strengths of Mounjaro Vial Inj (tirzepatide) on the 12th. Like the previously approved pre-filled pen, it comes in 2.5mg/0.5ml, 5mg/0.5ml, 7.5mg/0.5ml, 10mg/0.5ml, 12.5mg/0.5ml, and 15mg/0.5ml doses.However, its indication for chronic weight management in adults was excluded. The newly approved Mounjaro vial formulation is indicated solely as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes, either as monotherapy or in combination therapy.Earlier this month, Mounjaro Prefilled Pen received a positive reimbursement assessment as a diabetes treatment from the Drug Reimbursement Evaluation Committee (DREC) under Korea’s Health Insurance Review & Assessment Service (HIRA). Products that pass the DREC review proceed to price negotiations with the National Health Insurance Service (NHIS), followed by final listing approval by the Health Insurance Policy Deliberation Committee.With reimbursement listing now highly likely for the prefilled pen formulation, Lilly is expected to pursue reimbursement for the vial injection formulation as well.Lilly secured three formulations: Mounjaro Prefilled Pen in June 2023, Mounjaro QuickPen in September this year, and now Mounjaro vial formulation.The currently marketed formulation is the prefilled pen formulation, supplied without reimbursement as an obesity treatment. Mounjaro generated sales of KRW 28.4 billion (IQVIA) within two months of launch, fueling strong market momentum alongside Wegovy.Tirzepatide, the active ingredient in Mounjaro, selectively binds to and activates both GIP and GLP-1 receptors, which are targets of endogenous incretin hormones. Through this mechanism of action, it enhances first- and second-phase insulin secretion in a glucose-dependent manner and suppresses glucagon secretion. GLP-1 is a key physiological regulator of appetite and calorie intake.
- Policy
- ‘Gov’t investment and incentives needed to resolve drug shortages’
- by Jung, Heung-Jun Dec 15, 2025 09:16am
- Experts stressed that resolving shortages of essential medicines requires financial investment and policies like drug price incentives on the government’s part.They also argued that reliance solely on the private sector is insufficient, calling for the establishment of public manufacturing infrastructure and proactive cooperation frameworks in areas where dependence on overseas supply is unavoidable.Park Silvia, Research Fellow, Korea Institute for Health and Social AffairsOn the 12th, Park Silvia, a researcher at the Korea Institute for Health and Social Affairs, emphasized the need for policy support to enhance drug supply stability at the Korean Academy of Social and Administrative Pharmacy academic conference.She explained that since the COVID-19 pandemic, countries like the US and Europe are also preparing countermeasures to address pharmaceutical supply disruptions.The US is increasing domestic manufacturing through executive orders and taking measures to ensure excess capacity within its domestic supply chain. To expand domestic production, it provides financial support incentives and has established an evaluation system that rewards excellent manufacturers.This year, regulatory barriers have been lowered to facilitate the establishment of domestic pharmaceutical manufacturing facilities and to shorten approval timelines.Europe is also pursuing strategic projects to strengthen manufacturing capabilities. It has also strengthened supply planning and reporting obligations for license holders and expanded joint purchasing among member states to bridge gaps in access to essential medicines.Park noted that Korea is also seeing a rising number of reports related to drug supply disruptions and shortages, underscoring the urgency of policy responses.Park stated, “Strengthening the essential medicine manufacturing and supply chain has clear limitations when relying solely on corporate willpower. Financial support such as subsidies, grants, low-interest loans, investments, and tax incentives is necessary for developing manufacturing technology and establishing facilities.”She further proposed, “It is necessary to identify priority medicines for focused support and management, centered on national essential medicines. Priorities must be assigned to derive strategies. Additionally, manufacturers' supply risk management plans must be established and their implementation managed.”Park added, "Preferential drug pricing is needed to maintain domestic manufacturing of essential medicines, including APIs. Essential medicines for which domestic manufacturing and diversification are strategically pursued should receive preferential treatment in public procurement.“Finally, Park stressed the importance of the public role, stating, ”Relying solely on private pharmaceutical companies to supply all essential medicines has limitations. Building a public-centered pharmaceutical manufacturing infrastructure is also necessary. Furthermore, in areas where dependence on the global supply chain is unavoidable, a system that ensure active cooperation and solidarity is needed."
- Policy
- Discussions on RWE utilization in reimb decisions
- by Jung, Heung-Jun Dec 15, 2025 09:16am
- Guidelines for using Real World Evidence (RWE) in both the initial listing and subsequent reassessment of drug reimbursement status are expected to be announced in South Korea next year.The research commissioned by the Health Insurance Review and Assessment Service (HIRA) is nearing completion, and the guidelines will be published after gathering industry feedback.However, to use the guidelines for drug reimbursement, significant challenges remain related to securing the reliability of Real-World Data (RWD) and RWE. Furthermore, pushback is anticipated from pharmaceutical companies that are expressing concerns about the burden of generating RWE.On the afternoon of December 12, HIRA officials, the National Health Insurance Service (NHIS), and pharmaceutical companies engaged in a lively debate on the use of RWE for reimbursement decisions at the Korean Society of Social Pharmacy conference.Ra-Won Kang, Department Head of Drug Performance Assessment Management at HIRA.The HIRA announced its plan to publicize the guidelines soon following the completion of research on the use of RWE.Ra-Won Kang, Department Head of Drug Performance Assessment Management at HIRA, stated that the research on RWE utilization is nearing completion, and the guidelines will be published soon.Kang said, "Many major international organizations utilize RWE. In countries like Canada and the UK, RWE is largely used as a crucial basis for decision-making during both initial listing and post-listing reassessment of evidence."Kang emphasized, "The current challenge is how to ensure the reliability of the collection of RWD for the generation of RWE. Research into international cases shows that countries use guidelines tailored to their own circumstances for quality control. HIRA has also developed RWE guidelines research, and once it concludes this year, we plan to publish the guidelines next year after gathering input from stakeholders."Se-Rim Oh, Department Head of Negotiation and Post-Management at the NHIS.The statement conveys the message that RWE utilization is the government’s response to resolving uncertainties about increasing drugs subject to economic evaluation exemptions.Se-Rim Oh, Department Head of Negotiation and Post-Management at the NHIS, explained that the government's interest in utilizing RWE stems from concerns about resolving uncertainties amid the increasing number of drugs subject to economic evaluation exemptions.Oh stated, "Some responsibility lies with pharmaceutical companies. Many drugs have entered the market through the economic evaluation exemption route, even though an economic evaluation could have been conducted. Half of the risk-sharing agreement drugs approved this year and last year entered through this exemption," noting that this increases the uncertainty regarding cost-effectiveness. Oh stated, "RWE should be used if necessary. However, generating data can be expensive and difficult. There are concerns that predictability and acceptability might decrease," and added, "If necessary, establishing a legal basis and creating a government-wide registry would be appropriate." She also proposed that expanding performance-based refund agreements conducted by the NHIS and utilizing periodic performance reassessment data could be viable methods.Industry "RWD data have not been standardized…overseas data should also be allowed"The pharmaceutical industry expressed concern that the RWE guidelines could inadvertently become an additional layer of regulation, similar to clinical trials.Companies have complained about the heavy burden of RWE generation, particularly since RWD standardization has not yet been achieved. They strongly advocated for the recognition of international RWE data.Junghyun Na, Daiichi Sankyo Korea Head, stated, "First, the scope of application must be clearly defined. Also, the data in the field are varied and not standardized. Companies will inevitably face a substantial burden." Na emphasized that infrastructure, such as public platforms, must be built before implementation.Furthermore, companies stressed that if the process by which RWE will be reflected in reimbursement and pricing decisions is not predictable, the investment risk for companies would be significant.Jongryun An, Senior Director at Janssen Korea, explained, "Drugs entering through the economic evaluation exemption are reviewed without consideration for cost-effectiveness, but they typically enter at the lowest possible price. Furthermore, they are subject to total expenditure limits." An argued that measures to control high costs are already in place.An also raised the issue that collecting sufficient domestic data for rare and severe disease treatments in South Korea is challenging due to the small patient pool. An requested, "Please be flexible in accepting global RWE data if it was used in the process of obtaining approval or reimbursement in other countries."Additionally, An argued that the guidelines should be flexible, stating, "Overly detailed or strict guidelines could lead to a situation where no decisions can be made."
- Policy
- Bambec to withdraw from Korean mkt after 31yrs
- by Lee, Tak-Sun Dec 12, 2025 07:54am
- Bambec 10mg (bambuterol hydrochloride), used for asthma, is being withdrawn from the domestic market. This is a strategic withdrawal made by a multinational pharmaceutical company in response to declining competitiveness.Yuhan Corporation reported the discontinuation to the MFDS on December 10, noting that the final supply date was October 31.The company stated, “The discontinuation occurred following AstraZeneca Korea’s decision to cease sales, which led to the termination of the contract manufacturing agreement.”Approved in August 1994, Bambec had been sold in Korea for more than three decades. It is a long-acting β-adrenoceptor agonist (LABA) used for bronchial asthma, chronic bronchitis with bronchospasm, pulmonary emphysema, and other respiratory diseases.In recent years, combination therapies have dominated asthma and COPD treatment, reducing the market need for LABA monotherapy products and weakening their market competitiveness. According to UBIST data, Bambec's outpatient prescription sales reached KRW 1.4 billion in 2024.AstraZeneca sells other respiratory drugs in Korea besides Bambec, including Daxas, Pulmicort, and Symbicort. Compared to other products, Bambec’s sales performance is relatively low, and this relatively small market performance likely contributed to the global headquarters’ strategic decision to discontinue sales.Fortunately, generic versions remain available, so the discontinuation of the original drug is unlikely to create a significant gap. Generic versions with the same ingredients and formulation include Chong Kun Dang’s Asterol, Medica Korea’s Bambi, and Ildong Pharmaceutical's Bambutol.
- Policy
- RSA Collateral calculation method under review
- by Jung, Heung-Jun Dec 11, 2025 08:39am
- The National Health Insurance Service (NHIS) is currently reviewing improvements to the collateral calculation method for the refund-type risk-sharing agreement.Setting collateral in risk-sharing contracts is a crucial safeguard to secure claims in case refund obligations are not met. While a formula exists for setting the collateral amount, shortcomings were identified in some newly established RSA types, prompting NHIS to review improvements.According to industry sources on the 9th, this year’s NHIS audit highlighted deficiencies in the collateral calculation method for certain RSA types. The NHIS was advised to establish alternatives that would secure unpaid refund amounts for risk-sharing types lacking a collateral calculation formula.The NHIS's collateral-related operations are governed by the “Detailed Operational Guidelines for Drug Price Negotiations under Risk-Sharing Agreements.” Article 13 of the guidelines stipulates that the NHIS must receive collateral from companies to ensure the fulfillment of contractual obligations.Furthermore, the collateral amount is calculated using a separate formula, and the amount can be adjusted based on the type, the expected reimbursement amount, and the level of uncertainty.The collateral calculation methods are broadly categorized and specified in the guidelines as: ▲Conditional sustained treatment and refund hybrid type ▲Total expenditure cap type ▲Refund type ▲Patient-Unit usage cap type. For example, the Total expenditure cap type sets collateral at expected claim amount × refund rate × 30%.Within the RSA refund type, ▲the outcome-based reimbursement type is a newly added category for which no standardized calculation method is defined in the guidelines.According to the NHIS, the type of guarantee calculation formula identified as inadequate during the audit is the ‘outcome-based reimbursement type’. The NHIS stated it is currently under internal discussion and plans to revise the guidelines if necessary.An NHIS official explained, "The guidelines lack a calculation formula for the outcome-based reimbursement type. Internal discussions are ongoing, and revisions will be made to the guidelines if necessary."The outcome-based refund type is a contract type in which the applicant refunds a certain percentage of the total claim amount to the NHIS if the treatment effect set for each treated patient is not achieved after tracking and observing the treatment effect over a specified period.The outcome-based refund type is applied to some ultra-high-priced drugs, including Kymriah and Zolgensma.