- LOGIN
- MemberShip
- 2026-05-02 14:27:20
- Policy
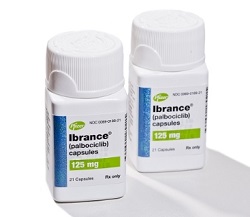
- Breast cancer Tx Ibrance’s AE rate at 86%...6yr PMS results
- by Lee, Hye-Kyung Jun 23, 2023 05:45am
- Post-marketing surveillance results of Pfizer Korea’s breast cancer treatment ‘Ibrance Cap (palbociclib)’ showed an adverse event rate of 86.01% for the drug. The Ministry of Food and Drug Safety prepared a label change order (draft) items based on its reevaluation results and will be conducting an opinion inquiry until the 5th of next month. The results of the post-marketing surveillance study conducted by Pfizer on 293 people for 6 years for its reevaluation showed that Ibrance’s reported adverse event rate was 86.01% (252/293 people, 642 cases), regardless of a causal relationship. Of these, 2.73% (8/293 patients, 11 cases) were serious adverse reactions (ADRs) whose causal relationship cannot be ruled out, and were reports of uncommon reactions such as inflammation of the lungs, febrile neutropenia, neutropenia, pancytopenia, pneumonia, asthenia, nausea, hepatitis, and decreased appetite, etc. Also, 13.6% (40/293 persons, 49 cases) were unexpected adverse drug reactions in which a causal relationship cannot be ruled out, with common reports of upper abdominal pain, constipation, indigestion, joint pain, insomnia, and pruritus. Less commonly, cough, pulmonary embolism, abdominal pain, and hepatitis were also reported. Ibrance is the first-in-class cyclin-dependent kinases (CDK) 4/6 inhibitor that was introduced to the field. It is indicated for the treatment of breast cancer in combination with an aromatase inhibitor as first-line endocrine therapy in postmenopausal women or in combination with fulvestrant in pre- and post-menopausal women with disease progression following endocrine therapy. After receiving the world’s fifth approval in Korea from the Ministry of Food and Drug Safety, it first recorded sales of KRW 6.6 billion in 2017, and then recorded KRW 25.3 billion after receiving reimbursement in 2018, then KRW 56.2 billion in Korea last year. In the first quarter of this year, Ibrance’s sales fell 13% from the previous year to record KRW 12.6 billion. Also, the drug succeeded in renewing its risk-sharing agreement (RSA) with the National Health Insurance Service in 2021, allowing the drug to receive reimbursement coverage until November 5, 2026.
- Policy
- Scemblix is listed in July
- by Lee, Tak-Sun Jun 23, 2023 05:45am
- Novartis 4th generation chronic myelogenous leukemia treatment Scemblix Novartis' 4th-generation chronic myelogenous leukemia drug Scemblix is expected to be listed for reimbursement in July. This drug is used as monotherapy for 3 or more lines, and reimbursement is applied when used in patients with chronic myelogenous leukemia aged 18 years or older. On the 22nd, HIRA announced the revision of the reimbursement criteria for anti-cancer therapy. Scemblix is covered for treating patients with chronic myeloid leukemia aged 18 years or older who are Philadelphia chromosome-positive in the chronic phase and who have previously been resistant or intolerant to two or more TKIs. The administration stage is 3rd or higher, but benefits are recognized if there is no T315I or V299L mutation. Scemblix is approved for the treatment of adult patients with chronic phase Philadelphia chromosome-positive chronic myelogenous leukemia (Ph+ CML) previously treated with two or more tyrosine kinase inhibitors (TKIs). As a result of reviewing HIRA with reference to textbooks, guidelines, clinical papers, etc., the drug is mentioned in textbooks, and in the NCCN guidelines, chronic myeloid leukemia that has previously been resistant or intolerant to two or more TKI agents has been classified as category 2A and explained that it was recommended. In addition, in ASCEMBL targeting chronic myeloid leukemia patients aged 18 years or older, the clinical usefulness of the Asciminib administration group was confirmed and the reimbursement standard was established. This drug passed the 2nd Cancer Disease Review Committee in March and the 4th Pharmaceutical Reimbursement Evaluation Committee in April. It is understood that the drug will be registered as reimbursement in July after NHIS drug price negotiations. Currently, 2nd generation Tasigna and Sprycel, and 3rd generation Iclusig are listed as reimbursement for chronic myelogenous leukemia treatment in Korea, and Scemblix is the first for the 4th generation.
- Policy
- Expansion of # of members of the Committee to around 105
- by Lee, Tak-Sun Jun 22, 2023 05:43am
- The number of members of the Pharmaceutical Reimbursement Evaluation Committee of the Health Insurance Review and Assessment Service will be expanded from around 100 to around 105. It is a policy to strengthen the expertise in evaluating the adequacy of drug treatment benefits by increasing the number of experts recommended by pharmaceutical-related societies by five more. On the 21st, HIRA announced an administrative notice of a partial revision of the committee's operating regulations containing these contents. This committee is a special committee that makes the final decision on whether or not to apply for benefits and whether the benefits of expanded drugs are appropriate. To that extent, the decision of this committee determines the fate of the drug. Drugs that have passed the Drug Evaluation Committee go through negotiations with the National Health Insurance Corporation and are listed on the final reimbursement list. In addition, pharmaceutical companies are always paying attention because it is in charge of the final deliberation of re-evaluation, such as re-evaluation of benefit adequacy and re-evaluation of the maximum amount. The Pharmaceutical Reimbursement Evaluation Committee is held every month, and out of the current 102 members, 17 members will take turns participating in each meeting. Currently, the 8th chairperson is Professor Emeritus Lee of Asan Medical Center in Seoul. This time, HIRA has been reorganized by dividing experts recommended by the Korean Medical Association into detailed specialties. As a result, the Orthopedic Surgery, Colorectal and Rectal Society, Orthopedic Internal Medicine, and Oncology Surgery were added. It is explained that the expansion of the human component of the Pharmaceutical Reimbursement Evaluation Committee was promoted in line with this. In the future, the number of members of the Pharmaceutical Reimbursement Evaluation Committee is expected to increase from the current 102 to 107. In this amendment, the criteria for selecting the chairperson were also relaxed. Previously, there was a criterion that more than two-thirds of the members present to elect the chairperson, but this provision has been deleted. Kim Kook-hee, head of the New Drug Listing Department at HIRA, explained, "Compared to the subcommittee, unnecessary criteria were deleted." In this amendment, the criteria for the application of exclusion, evasion, and evasion are also revised in order to comply with the Public Officials Conflict of Interest Prevention Act to improve fairness, objectivity, and transparency in the operation of the committee. Accordingly, the period corresponding to private stakeholders was extended from 12 months to 2 years.
- Policy
- New drug pre-registration - post-evaluation non-face-to-face
- by Lee, Jeong-Hwan Jun 22, 2023 05:41am
- The government plans to include discussions on the need to apply innovative insurance systems such as new drugs and new medical technology 'seondeungjae-postevaluation' to strengthen treatment coverage for severe diseases such as cancer in the '2nd National Health Insurance Comprehensive Plan' to be established in the second half of this year. The purpose is to draw a blueprint for the future in which a sustainable health insurance policy to supply new drugs and new medical technologies to the people in a timely manner can be discussed at the social consensus body. In particular, it also revealed the direction that measures to activate home medical treatment and institutionalize non-face-to-face treatment will inevitably be included in the 2nd comprehensive health insurance plan to establish a health care policy that goes beyond time and space constraints. The Ministry of Health and Welfare and KIHASA, which initiated the establishment of the 2nd health insurance plan, made this announcement on the 19th at the 'policy debate for health insurance reform desired by the people hosted by Lee Jong-Seong, a member of the People's Power, and hosted by the Future Health Network. On this day, the results of a public awareness survey on national health insurance conducted with 5,000 people across the country were released. As a result of the survey, 85% of the respondents agreed to strengthen the guarantee of new drugs and new medical technologies for the treatment of severe diseases such as cancer or rare diseases. Shin Hyun-woong, a senior research fellow at the National Health Insurance Institute, who is in charge of research on the 2nd health insurance comprehensive plan, revealed the direction of the comprehensive health insurance plan. Researcher Shin Hyeon-wrong explained that although the details cannot be mentioned in detail as the research is still in progress, the outline of the health insurance plan set up by the Yoon government will be partially disclosed. Commissioner Shin said that the 2nd Comprehensive Health Insurance Plan would take a different direction than the previous administration, which focused on increasing the coverage rate by resolving economic accessibility. It was said that the 2nd Comprehensive Plan would contain not only economic feasibility, but also concerns about medical coverage policies that transcend time, space, geography, and service constraints anytime, anywhere. Commissioner Shin cited home medical services and institutionalization of non-face-to-face medical treatment as representative examples. In particular, he said that he would include in the research the health insurance pre-registration and post-evaluation policies for new drugs and new medical technologies, along with measures to resolve the current fee-for-service fee system limitations. Commissioner Shin said, "Currently, the people's medical need is high, but there is a problem that the medical service itself is not created. The essential medical vacuum comes out when you turn on the news." "We will provide medical guarantees that go beyond the limits of time and space. For a health care policy that resolves time and space constraints, home medical care and non-face-to-face care have no choice but to be dealt with," he explained. Commissioner Shin said, “The higher the frequency of the fee-for-service system, the higher the profit. The lower the investment, the lower the investment.” We are thinking about reorganizing the payment system," he added. Commissioner Shin said, "In terms of coverage, we will cover not only treatment but also prevention and health care, as well as mental health. We are considering a system that preemptively guarantees medical safety net funds, anticancer drugs, and expensive drugs for rare diseases." I am doing it," he said. Son Ho-Joon, head of the insurance policy department at the Ministry of Health and Welfare, also announced that he would establish a second health insurance plan to create a structure in which the health insurance system plays a role in ensuring people's medical care. He also said that he would improve the problem of financial leakage, and discuss the registration of health insurance for anticancer drugs, rare disease treatments, and innovative medical technologies and medical practices. Manager Son Ho-Joon said, "We plan to establish a second health care plan that includes not only the financial sustainability of health insurance but also the reason for the existence of the health insurance system." A representative case is to catch the unnecessary leakage of finance and invest in essential childbirth and pediatric medical care.” Manager Son said, "In addition to this short-term approach, a structural and health insurance approach is included in the comprehensive plan. We will also discuss the issue of the payment system and enter into it to ensure the people's essential medical care." It also includes discussing the application of an innovative insurance system for new drugs and new medical technologies to enable the continuous supply of medical services while looking at whether they will play a role.”
- Policy
- MFDS cautious about strengthening regulations
- by Lee, Jeong-Hwan Jun 22, 2023 05:40am
- The Ministry of Food and Drug Safety explained that although the MFDS with the purpose of the legislation to strengthen regulations on drugs that have been conditionally approved for expedited marketing authorizations before completing Phase III clinical trials from the current guideline level to the Pharmaceutical Affairs Act level, its application will require ample collection of opinions from stakeholders. In other words, the MFDS has a cautious stance regarding the reinforcement of related regulations. However, there was also the opinion that mandating all matters related to conditional expedited approval drugs to be decided through the Central Pharmaceutical Affairs Committee could lead to delay and overload of work in practice. Regarding the bill, the Korean Pharmacists Association for a Healthy Society expressed its support for its legislation while Korean Research-based Pharmaceutical Industry Association (KRPIA) took an opposing stance. On the 20th, the Ministry of Health and Welfare's position was included in the review report on the proposal for the amendment to the Pharmaceutical Affairs Act, which included reinforcing regulations of conditionally approved drugs, that was presented by the Democratic Party of Korea Rep. Jong-Yoon Choi. Choi’s bill stipulates that if a pharmaceutical company that has received conditional approval for a Phase III trial wants to extend the data submission period, including those for clinical trial data, it must apply for the extension to the Minister of Food and Drug Safety in advance and the minister shall listen to the opinions of the CPAC and decide whether to extend the period. It also contains a mandatory provision for pharmaceutical companies that have received conditional approval for items shall report their plans to submit data, such as clinical trial data of its users, to the Minister of Food and Drug Safety within 3 months from the date of approval. Also, the report on the implementation status of the reported plan, such as the status of clinical trials, was increased from the current once a year to semi-annually, that is, twice a year, to the Minister of Food and Drug Safety. However, no separate provisions for punishment were prepared for their non-compliance. To the bill, the Expert Committee of the National Assembly's Health and Welfare Committee judged that when considering the characteristics of conditionally approved drugs, there is a need to stipulate provisions in the current management guidelines to check whether the conditions to submit clinical data have been fulfilled. Specifically, to extend the deadline for submitting clinical trial data for currently conditionally licensed drugs, the MFDS first conducts an internal feasibility review, and then, if necessary, consults with the CPAC or external advisors before finally deciding whether to adjust the conditions for approval, such as by extending the submission deadline. The expert committee members agreed that a stricter review of the data submission obligation may be needed so that companies do not neglect the data submission obligation or abuse the extension system. On the part, the experts agreed with the purpose of the amendment, which will stipulate the procedure for extending the data submission period by law rather than just a guideline as in the current state and require CPAC advice when deciding on allowing the extensions. However, the committee also added that the opinion that MFDS’s compulsory consultation with the Central Pharmacy on all matters regardless of the severity of the case, could cause work delay. Regarding the provision to report the clinical trial plan to the Minister of Food and Drug Safety within 3 months from the date of approval of conditional approval drugs, the expert committee said that the provision does not conform to the reality of the situation as a clinical trial of some drugs are not approved at the time the conditional approval is granted. Also, the expert committee diagnosed that increasing the number of reports to the MFDS on the progress of clinical trials from the current once a year to twice a year would be beneficial for management as it will allow the authorities to quickly be known of changes made in clinical trials. At the same time, the expert committee asked for the authorities to comprehensively review the opinion that it may increase the risk of administrative burden on the pharmaceutical industry. Regarding the bill, the Ministry of Food and Drug Safety took a neutral stance, saying, “We will need to sufficiently collect industry opinion,” stating the need to minimize resistance from the pharmaceutical industry and secure receptivity for the regulations. The MFDS said, “We agree with the purpose of the amendment to strengthen the management and supervision of conditional approval drugs. However, further review will be needed in consideration of the working-level business process. "We need to sufficiently collect opinions from the industry to secure regulatory acceptance.” The Korean Pharmacists Association for a Healthy Society agreed to the bill, saying, “The bill strengthens the safety verification of conditionally licensed drugs. We agree with the purpose of the amendment to strengthen the responsibility of the MFDS in verifying drug safety, by requiring CPAC review when deciding whether to extend the submission period for clinical data for conditionally approved drugs." However, the Korean Research-based Pharmaceutical Industry Association opposed the bill. “In the case of conditionally licensed drugs, 6 months is generally too short to report any significant changes that require MFDS attention to the authorities. Semi-annual submission of reports will increase the burden of time and labor for companies."
- Policy
- Imported orphan drug specimen storage standards
- by Lee, Hye-Kyung Jun 22, 2023 05:40am
- The Ministry of Food and Drug Safety (Minister Oh Yoo-gyeong) announces a legislative announcement on the 21st of the amendment to the 'Rules on Safety of Pharmaceuticals, Etc. and, comments are accepted until August 21st. The main contents of this revision are ▲ rationalization of sample storage standards for importers of imported orphan drugs ▲ allowing companies applying for national release approval to directly collect and submit samples for testing ▲ operation of the number of samples approved for national release, processing deadlines, and inspection items in the form of public notice. Currently, all pharmaceuticals must keep a sample volume that can test the test items specified for each product more than twice. Importers may only keep samples for product identification. When applying for national shipment approval for pharmaceuticals such as vaccines, current public officials visit the drug storage facility to collect and collect samples and seal the rest. In order to increase the flexibility and promptness of the operation of the national lot release approval system, ▲the national lot release processing period ▲quantity of test samples ▲approval items, which were regulated by the Ministry of Food and Drug Safety*, will be improved so that the Minister of Food and Drug Safety can announce them in the future. The Ministry of Food and Drug Safety said it would continue to strive for a stable supply of medicines to ensure patient treatment opportunities, and to support the revitalization of the domestic pharmaceutical industry by rationally improving regulations within the scope of ensuring safety. Details on this amendment can be found on the Ministry of Food and Drug Safety website (mfds.go.kr) → Laws and Materials → Administrative Notice.
- Policy
- 85% of the public requests more coverage for severe diseases
- by Lee, Jeong-Hwan Jun 21, 2023 05:52am
- A survey found that more than 8 of 10 Koreans are in favor of increasing health insurance spending on new health technologies and new drugs to treat severe diseases such as cancer and rare diseases. Also, over 80% of the respondents agreed that the proportion of new drugs in total health insurance pharmaceutical spending should be increased and that health insurance should promptly cover new drugs. On the 19th, the Future Health Network (representative Ok-Ryun Moon, Professor Emeritus at Seoul National University), a think tank in the field of healthcare, unveiled the survey results that contained the results above at a ‘Policy Debate for Health Insurance Reform that the People Want’ that was hosted by Rep. Lee Jong-Seong of People Power Party. The survey, which was commissioned to Gallup Korea, researched 5,039 people aged 19 to 65 across the country last April. In the survey, 85% of the respondents agreed (21% strongly agree, 21% strongly agree, 64% agreed) that ‘expanding the coverage of essential healthcare from now on, should focus on severe diseases rather than mild diseases.’ On which requires priority coverage – essential healthcare for severe diseases or frequently occurring mild diseases, 73% responded in favor of severe diseases, which was more than four times higher than the 17% that choose mild diseases. To the question that how a (presumable) KRW 10 million of Korea’s health insurance finances should be allocated, respondents allocated KRW 6,615,000 to severe diseases and KRW 3,385,000 won to mild diseases. When asked would be better to preferentially spend the funds secured by reducing health insurance drug expenses on covering severe disease or mild disease, 72% chose severe diseases, which was 54%p higher than the proportion of those who chose mild disease. Also, 81% agreed with the plan to increase expenditures on new drugs or new health technologies out of the total health insurance budget. 83.8% agreed on the need to increase the proportion of new drugs in Korea’s total health insurance pharmaceutical expenditures. On the reason why the government should strengthen coverage of new drugs and new health technologies, respondents showed a strong agreement of 91.2% to the reason that ‘Those can save the people's lives or guarantee their quality of life.’ Also, 87.1% agreed to the claim that it was 'because it can prevent losses that may arise from non-coverage, such as other medical expenses, care expenses, and social and economic burdens.’ 87.9% of the respondents agreed that the government should promptly apply health insurance coverage when new drugs for severe diseases such as cancer and rare diseases are developed in Korea and abroad. As its measure, 80.0% of the respondents agreed that a pre-listing post-evaluation system should be applied to new drugs and new health technologies that have been approved for their efficacy and safety by overseas health authorities. As for the reason for consent, 45.3% said 'because this will allow timely coverage of new drugs and new health technologies for the patients’, and 25.5 said 'because patients cannot receive sufficient treatment with private insurance alone for severe or rare diseases.' 80.5% of the respondents agreed that the government should further expand its financial support for the national health insurance finances and create a separate medical expense fund. 82.4% of respondents agreed on the need to create a separate medical expense fund for those with severe or rare diseases and the vulnerable with government subsidies. 83.2% of respondents agreed that the pharmaceutical companies' health insurance contributions should fund the catastrophic medical expense support project to support the use of new drugs and new health technologies. Based on the results above, Professor Jin-Hyoung Kang, who was in charge of the presentation, suggested a policy that shifts the principle of health insurance coverage to give priority to severe diseases and essential healthcare, and that it is necessary to create and operate a medical safety net fund. Pressor Kang also suggested promoting a pilot project in the form of a pre-listing and post-evaluation system to promptly apply coverage to new drugs and new health technologies, and devise ways to expedite review such as integrated operation of the HIRA-NHIS committees or parallel review. In addition, Professor Kang out the need to comply with the government's statutory support rate for health insurance to ease the public burden of national insurance premiums. His argument was that the government should take measures such as increasing the government subsidization rate from the current 14% of the expected revenue of health insurance to 20%, in compliance with the legal rate. Meanwhile, the government plans to establish and announce the 2nd Comprehensive National Health Insurance Plan, which will contain the health insurance policy direction for the next 5 years (2024-2028) in the second half of the year.
- Policy
- Mandatory benefit for Erleada impact?
- by Lee, Tak-Sun Jun 20, 2023 05:36am
- As Erleada, a prostate cancer treatment, has received mandatory reimbursement since last April, attention is focusing on whether the co-payment ratio for Xtandi and Zytiga in the same class will be reduced. Currently, Erleada receives mandatory benefits with a co-payment of 5%, and Xtandi·Zytiga receives 30% screening benefits. The Cancer Disease Review Committee of the Health Insurance Review and Assessment Service held the 4th meeting in 2023 on the 14th and decided to reduce the co-payment rate for Xtandi and Zytiga. Earlier in April, Janssen Korea's Erleada was listed as a mandatory benefit with a co-payment rate of 5% for the first time in the Androgen receptor targeted agent series. Accordingly, the same family of drugs, such as Xtandi and Zytiga, which receive screening benefits of 30% of the co-payment rate, applied for the expansion of mandatory coverage. The review committee recommends androgen deprivation therapy (ADT) in combination with Xtandi for the treatment of patients with hormone-responsive metastatic prostate cancer (mHSPC) and Zytiga for the treatment of patients with hormone-responsive high-risk metastatic prostate cancer (mHSPC). ) and combination therapy (combination with prednisolone), it was decided to change the rate of co-payment. On the same day, the review committee also set the reimbursement standards for the new reimbursement application drugs, Jemperli for endometrial cancer treatment and Xpovio for multiple myeloma treatment. On the other hand, Gavreto and Vyxeos Liposomal failed to set reimbursement standards.
- Policy
- Negotiations between Verquvo and Retevmo begin
- by Lee, Tak-Sun Jun 20, 2023 05:36am
- Retevmo, an anticancer drug with mutations in RET, and Verquvo, a treatment for chronic heart failure, have entered into drug price negotiations with the NHIS. It is said that negotiations are still underway for Cibinqo, which started negotiations on drug prices in March, and Onureg, which started negotiations with the company last month. The NHIS recently updated its new drug price negotiation target through its website. The newly updated information is that Verquvo 2.5, 5, and 10mg and Retevmo 40, 80mg were included in the drug price negotiations in June. The two drugs were recognized for their reimbursement adequacy at the 2023 5th Pharmaceutical Reimbursement Evaluation Committee held on the 4th of last month. Verquvo is effective for chronic heart failure, and Retevmo is effective for RET fusion-positive non-small cell lung cancer, RET-mutated medullary thyroid cancer, and RET fusion-positive thyroid cancer. Verquvo is the world's first sGC accelerator to be approved for the treatment of chronic heart failure, and clinical trials have shown that it reduces deaths or hospitalizations due to heart failure by 10% compared to the placebo group. Retevmo was the first RET gene mutation anticancer drug to pass the evaluation committee in Korea. It has become official that drug price negotiations are underway for Onureg 200 and 300mg, which passed the committee last April. This drug is approved for maintenance therapy after induction therapy in adult patients with acute myeloid leukemia. It is understood that the atopic dermatitis treatment Cibinqo 50, 100, and 200mg, which passed the committee in February, is still under negotiation even after 60 days of negotiations. In particular, it was analyzed that this drug would shorten the time until it was listed as reimbursement, as it was known to have accepted the drug price suggested by the committee, but the NHIS negotiations are sluggish.
- Policy
- Rationalization of expedited review of new pharmaceuticals
- by Lee, Hye-Kyung Jun 20, 2023 05:35am
- In the case of a new drug developed by a first-in-class pharmaceutical company, a priority review request can be made to the rapid review division of the Ministry of Food and Drug Safety. The Ministry of Food and Drug Safety recently prepared detailed procedures, such as the method of requesting designation from the Minister of Health and Welfare, when prioritizing new drugs developed by innovative pharmaceutical companies. According to Article 35, Paragraph 4 of the Pharmaceutical Affairs Act, which was revised in July 2021, 'drugs for which the Minister of Health and Welfare has requested designation among new drugs developed by innovative pharmaceutical companies pursuant to Article 2, Subparagraph 3 of the Special Act on the Promotion and Support of the Pharmaceutical Industry' may be designated for priority review. This means that even for a new drug developed by a first-in-class company, the Ministry of Health and Welfare must request designation before the Ministry of Food and Drug Safety can proceed with an expedited review. If this continues, innovative pharmaceutical companies will have to request a request for support from the Ministry of Health and Welfare, and after that, the Ministry of Health and Welfare will request designation, and the Ministry of Food and Drug Safety will have to go through the process of reviewing the rapid review. The Ministry of Food and Drug Safety said, "In order to quickly resolve the difficulties of first-in-class companies, we have prepared a procedure so that an official letter requesting designation can be sent from the Ministry of Health and Welfare's Health Industry Promotion Division to the Ministry of Food and Drug Safety's Rapid Review Division without establishing a separate procedure." When an innovative pharmaceutical company proceeds with a request for review of priority review designation to the Ministry of Food and Drug Safety's rapid review department, the rapid review department requests confirmation of the innovative pharmaceutical company's certification from the Ministry of Health and Welfare and receives a reply and a request for priority review designation directly from the Ministry of Health and Welfare. Therefore, first-in-class companies only need to contact the Ministry of Food and Drug Safety to apply for expedited review, and then apply for product approval. Meanwhile, not only new drugs developed by innovative pharmaceutical companies but also drugs prescribed by the Prime Minister Ordinance that is used for the purpose of treating serious severe diseases or rare diseases under Article 2, Subparagraph 1 of the Rare Disease Management Act are subject to expedited review. The Ministry of Food and Drug Safety shall decide whether to designate the drug within 30 days of receiving the application for priority review and notify the applicant of the result.